Ariane Fung , Ai-Leng Foong-Reichert , Sherilyn K D Houle , Kelly A GrindrodABSTRACT
Background
Past research on disciplinary action by pharmacist regulatory bodies has shown that most cases concern community pharmacists, with few occurring in a hospital setting.
Objective
To investigate how discipline-related issues involving pharmacists are dealt with by hospital pharmacy departments in Canada.
Methods
Hospital pharmacy directors and managers from small, medium, and large hospitals across Canada were invited to participate in semi-structured telephone interviews. The interview questions focused on the discipline process in participants’ organizations, the situations when reporting to the regulatory body is deemed to be warranted, possible penalties, and recommendations for improving the regulatory body or organizational discipline process.
Results
Ten participants, from British Columbia, Saskatchewan, Ontario, New Brunswick, Prince Edward Island, and Newfoundland and Labrador, agreed to be interviewed. Five key themes emerged as contributing to lower rates of hospital pharmacist discipline cases being escalated to the regulatory college level: robust organizational discipline processes independent from the regulatory college, a practice environment promoting competence, union representation, preference for a remedial approach to discipline, and lack of clarity about when to report to the regulatory authority.
Conclusions
This study identified a number of reasons why discipline of hospital pharmacists by a regulatory body may be less prevalent than discipline relating to community pharmacists. The main reasons may be lack of clarity about when to report a case to the regulator and a lack of transparency, given that many cases are handled internally within hospitals. Environmental supports for competence and employee protections (e.g., through a union) may also reduce discipline cases.
KEYWORDS: hospital pharmacy, disciplinary action, organizational discipline, pharmacy
RÉSUMÉ
Contexte
Des recherches antérieures sur les mesures disciplinaires prises par les organismes de réglementation des pharmaciens ont montré que la plupart des cas concernaient des pharmaciens communautaires, et que peu se produisaient en milieu hospitalier.
Objectif
Examiner comment les questions disciplinaires impliquant des pharmaciens sont traitées par les départements de pharmacie hospitalière au Canada.
Méthodes
Les directeurs et gestionnaires de pharmacies de petits, moyens et grands hôpitaux au Canada ont été invités à participer à des entrevues téléphoniques semi-structurées. Les questions portaient sur le processus disciplinaire en place dans les organismes des participants; les situations où le signalement à l’organisme de réglementation était jugé justifié; les sanctions possibles; et les recommandations pour améliorer le processus disciplinaire de l’organisme de réglementation ou de l’organisme.
Résultats
Dix participants de la Colombie-Britannique, de la Saskatchewan, de l’Ontario, du Nouveau-Brunswick, de l’Île-du-Prince-Édouard et de Terre-Neuve-et-Labrador ont accepté d’être interrogés. Cinq thèmes clés ont été identifiés comme contribuant au taux plus faible de cas de discipline des pharmaciens hospitaliers remontés au niveau de l’organisme de réglementation: des processus disciplinaires organisationnels solides indépendants de l’organisme de réglementation; un environnement de pratique favorisant la compétence; la représentation syndicale; la préférence pour une approche corrective de la discipline; et le manque de clarté quant au moment où il faut signaler à l’autorité de réglementation.
Conclusions
Cette étude a identifié un certain nombre de raisons pour lesquelles les mesures disciplinaires relatives des pharmaciens hospitaliers par un organisme de réglementation peuvent être moins répandues que celles liées aux pharmaciens communautaires. Les principales raisons pourraient être le manque de clarté quant au moment de signaler un cas à l’autorité réglementaire et un manque de transparence, étant donné que de nombreux cas sont traités en interne dans les hôpitaux. Les soutiens environnementaux pour la compétence et la protection des employés (par exemple, par l’entremise d’un syndicat) peuvent également réduire les cas de discipline.
MOTS CLÉS: pharmacie hospitalière, mesure disciplinaire, discipline organisationnelle, pharmacie
Hospital pharmacists are much less likely than community pharmacists to be disciplined by a regulatory body. Although 15% of licensed Canadian pharmacists work in hospitals,1 a Canadian review of regulatory body disciplinary cases from 2010 to 2017 showed that only 1% (6/558) of cases occurred in a hospital setting.2 Of the 558 cases, 503 (90%) occurred in a community setting, 2 in long-term care, 1 in a family health team, and 46 in an unspecified place of practice.2 Studies from the United Kingdom have also found that most pharmacist disciplinary cases concern community pharmacists. One UK study found only 1 case (0.3%) involving a hospital pharmacist within the 12-year study period, whereas 86.3% involved community pharmacists, and the remainder involved students or an undetermined place of practice.3 A second UK study found that 8 cases (6.8%) involved hospital pharmacists, 89 cases (76.1%) involved community pharmacists, and the rest involved pharmacists in primary care, industry, academia, or an undetermined place of practice.4
Given the lack of data on this topic, the objective of this study was to investigate how discipline-related issues involving pharmacists are dealt with by hospital pharmacy departments in Canada.
This study received ethics clearance through the University of Waterloo Research Ethics Committee. Our reporting follows the consolidated criteria for reporting qualitative research (COREQ) checklist.5 We identified a purposive sample of select hospital pharmacy directors to ensure representation from various Canadian provinces and from large (> 500 beds), medium (201–500 beds), and small (< 200 beds) hospitals.6 A purposive sample “purposefully” or intentionally selects information-rich cases so as to include a certain range of cases.7
Seventeen participants were contacted by email using contact information retrieved from professional connections or publicly available sources. A follow-up email was sent 1 week after the initial invitation, for those who had not responded. Written or verbal informed consent was obtained from all those who agreed to participate. Open-ended, semi-structured interviews were conducted from October to December 2020 by telephone or video call; the interviews were audio-recorded, with participants’ consent. The lead authors (A.F. and A.F.-R.) conducted all interviews. Audio recordings were transcribed by a professional transcribing company, and the transcriptions were reviewed for accuracy by the lead authors. The duration of each interview was determined from the audio recording.
We initially arranged for a minimum of 10 interviews, with the option to pursue more interviews if needed to reach saturation. Although thematic analysis was not performed concurrently with data collection, saturation was determined according to the opinion of the 2 interviewers, who kept interview notes and discussed key points after each interview and identified that after 8 interviews, no new major points were being discovered.
The data were analyzed systematically using thematic analysis, in accordance with the Framework Method.8 These steps consist of transcription, familiarization with the content of each interview, coding, development of a working analytical framework, application of the framework, charting of data into the framework matrix, and interpretation of the data. Codes were created after 3 interviews had been conducted and were then applied to the transcripts of 2 of these 3 interviews. The codes were refined and applied to the third transcript, at which point they were found to be sufficient to encompass the data for all 10 interviews. Each transcript was coded in Word software (version 16.43, Microsoft Corporation), with coding performed independently by the lead authors. Themes were continually refined through consensus discussion to ensure consistency. Quotations used in the final manuscript and their context were returned to participants to verify transcription and interpretation and to allow participants to add comments or corrections. Study results were made available to participants upon request.
The interview guide (Appendix 1) was developed with pre-existing knowledge about themes of disciplinary action involving community pharmacists.2–4 We used an iterative approach to modify the interview guide throughout the data collection process to incorporate new themes that emerged. Not all interview questions were intended to yield a reported result or contribute to a theme, as some questions were general and intended to help familiarize the interviewers with processes at participants’ hospitals.
Each interview was divided into 4 sections. The first section sought to generate an understanding of current discipline processes for pharmacists within each organization and insight as to why hospital pharmacists are subject to regulatory body discipline less frequently than community pharmacists. The second section focused on reasons why pharmacists are disciplined. In the third section, hypothetical case-based scenarios were presented to the participants, with the aim of gathering data on whether and how a pharmacist would be penalized and whether the scenario would be reported to the regulatory body. The last section discussed ways to improve the disciplinary process. The interview guide was pilot-tested by 2 hospital pharmacists who otherwise were not involved in the study, to ensure clarity of the questions.
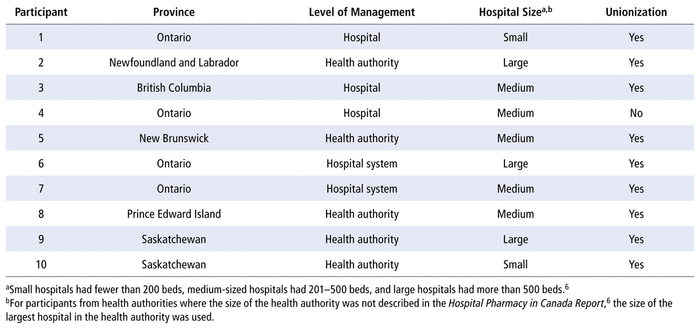
Of the 17 participants we contacted, 10 agreed to participate in an interview (Table 1). Two regional hospital directors were working at the provincial level, 2 were regional pharmacy directors of a large health authority, and the others were pharmacy directors of their respective hospitals. Interviews ranged in duration from 24 to 43 minutes (mean 33 minutes).
TABLE 1
Characteristics of Hospitals Represented by Participants

The data analysis highlighted 5 themes describing why discipline of hospital pharmacists is less prevalent than discipline of community pharmacists, as discussed in the sections below.
Organizational discipline encompasses the processes used to correct employee behaviour when there is a justifiable reason for such correction. It involves confirming that the employee committed an offence, that the offence warrants correction, and that the penalty is appropriate.9–11 Progressive discipline is typically used, whereby disciplinary measures are gradual and appropriate to the offence.11,12 All participants described an organizational discipline process independent of the regulator that was used to handle most cases of pharmacist misconduct or incompetence.
Participant 9: I’m unaware of any instances in my 30-year history that ever went to the college. And the reason for that is we would have nipped that in the bud far before it’s gone to the college.
Participants described various penalties imposed by the hospital, including a reprimand or discussion with the employee, restrictions or conditions on practice (e.g., restricting the employee’s access to narcotics, relocating the employee to a different clinical setting), remediation, suspension, and termination.
Another organizational attribute of hospitals is that they have formal processes to receive and address patient complaints, which likely diverts complaints from a pharmacy regulatory body.
Participant 2: The fact that there is an opportunity for a client or a client family member who has concerns about the appropriateness or quality of the service that they received [decreases reports to the college], because I think that can be very de-escalating.
Participants described organizational discipline processes involving all or some of the following parties: the employee in question; a pharmacy director or manager; and representatives of human resources, quality and risk management, professional practice, labour relations, and the union. All but one participant reported that pharmacists in their organization were unionized. Participants stated that terms negotiated through the union directed the discipline process, including whether or not cases were reported to the regulator.
Participant 9: There are very clear pathways to move into progressive discipline. And within those pathways, it is all within the contract, the next steps that will be taken.
Participant 1: I think one of the potential differences is the fact that all pharmacists in my site are part of the union. So, there’s obviously that human resources and union component [that] has to be established first before the college would be approached.
Participants also described how the union can influence and limit the penalties that can be applied in a disciplinary case.
Participant 9: And within a unionized environment, there is a defined process that is utilized prior to separation. It takes a significant series of actions and it takes a significant demonstration of attempts to remediate.
This theme focused on how the hospital environment reinforces competence and minimizes reliance on a traditional regulatory discipline process.
First, lower discipline rates for hospital pharmacists were credited to a probationary period during which newly hired pharmacists could be terminated if they did not meet required competence standards. Additionally, participants cited the hiring of residency-trained pharmacists as a reason for lower discipline rates.
Participant 4: We also have probationary periods when they first start, and we’re very careful to monitor those probationary periods to ensure that they’re performing at the levels we need. And if not, then we just terminate their employment before they actually reach that level.
Participant 7: I think residency-trained pharmacists come in with a much better clinical skill set and knowing the boundaries of that skill set.
The collaborative nature of clinical decision-making in hospitals may also support safer or more competent practice.
Participant 1: In community, you frequently just practise by yourself. You just kind of have to make a decision in the moment and you don’t have access to other people, but in hospital there are so many people around all the time.
The highly collaborative nature of hospital practice leads to a shared liability, both among health care providers, but also with the organization itself. This leads to a shared sense of responsibility for medication errors or clinical incidents, as there are many clinicians involved in the care of a patient.
Participant 6: What I do know is that going to the college level of discipline for a hospital pharmacist is a really rare event, because most of the time they’re working within a team or a collaborative practice environment ... they have readily available backups to help support them through that situation.
That said, the organizational safeguards that are in place in hospital environments can lead to different reasons for discipline than in community practice, with a few participants specifying privacy and confidentiality violations as a common reason for discipline.
Participant 6: We tend to have a different role in the community, so there’s not a lot of dispensing errors as the main driver of a patient complaint. Where we will wind up having more potential challenges are if somebody goes sifting for personal health information on an individual who’s been admitted to our hospital.
These same safeguards may ensure there is less opportunity for intentional misconduct, such as narcotic theft and diversion in hospital. Although it is a common reason for discipline among community pharmacists, participants attributed the lower rate of this violation in hospitals to increased controls and policies.
Participant 2: And part of that I think is because of the rigorous control that exists within this institution around controlled substances. It’s highly automated, very highly documented with a lot of oversight.
However, the size of the hospital is key. Participants mentioned that a smaller hospital might not have the same resources to support professionalism and competence.
Participant 7: We would like to do a lot more education on … professional responsibilities, rights, scope, all of that. That’s where we don’t have the resources that a larger hospital that has dedicated resources for education, teaching.
Participants described hospitals having a nonpunitive atmosphere that tends to emphasize remediation and rehabilitation. Most reported that cases are typically handled within the organization and are not reported to the regulatory authority, unless termination of employment is involved.
Participant 9: If a lack of competence was demonstrated, we would put that person into a further training perspective and then take it from there.
The focus on remediation and rehabilitation stems from hospitals working toward a culture of safety and away from one of placing blame on a specific health professional for a particular negative outcome.
Participant 2: The culture within our practice is, very much so, learning from clinical type[s] of errors and process errors and improving the system and putting supports in place to prevent them, rather than punitive because a disciplinary response would certainly discourage reporting of such occurrences, which doesn’t help anybody.
Although it was not a universal opinion, one participant viewed reporting to the regulator as punitive, and thus a deterrent to reporting. A less punitive approach could support hospitals in reporting concerns to a college.
Participant 7: I believe there is still quite a bit of bias in the pharmacist and technician community that the college reporting system is for bad members. If the college tried to shift that perception a little bit by offering help to individual members that an employer [reports] or self-referral … then I might change my answer.
None of the participants had dealt with a case where an inpatient pharmacist was reported to the regulator (although two had dealt with cases in which an outpatient hospital pharmacist was reported). In addition, a few participants expressed uncertainty about when to report a case to the regulator and noted that this study had prompted reviews of their organizational procedures.
Participant 7: It’s just our thinking on, “Why have we never [reported to the college]?” ... It’s like, “Well, should that be a last resort or should it be built into the process earlier on if our performance development reveals professional practice issues or deficiencies?” Again, we’re right in the middle of this right now because your email sort of started the conversation.
Participants agreed that an isolated clinical error would not be reported to the regulatory body, but would be discussed with the health professional, investigated as a medication incident, and addressed with remediation. Participants also agreed that cases of gross or repeated incompetence that did not improve with remediation could be reported to the regulator. However, when asked whether they would report a pharmacist with a history of incompetence who changed employment of their own accord, not through termination, participants disagreed on whether this would be reported to the regulator. Nine of the 10 participants agreed that a substance use disorder would be reported, and participants agreed that cases involving theft of a narcotic (e.g., diversion or trafficking) could also be reported to the regulator.
Some participants explained that their organizations had clearly defined processes for reporting to the regulator.
Participant 4: We actually have a professional practice framework in the hospital so that there is clear guidance as to when we have to report to the college.
Others identified that increased clarity on this process within their organization, developed in conjunction with the regulator, could improve the discipline process.
Participant 10: Development of an algorithm that if A happens, this is the road it takes, if B happens, this is the road it takes would be useful. It feels that it would be really hard to apply because every situation offers its own nuances but it would provide some guidance and a starting point.
However, the main confusion was about issues that fall outside clear violations.
This study identified possible reasons why pharmacists in Canadian hospitals are less likely than community pharmacists to be disciplined through the relevant regulatory body. This difference may be due to organizational discipline processes, union representation, the nature of the practice environment, a nonpunitive approach to discipline, and lack of clarity about when reporting to the regulator is warranted. This study highlights how hospitals often assume the disciplinary role of the regulator in all but the most serious cases. By comparison, community pharmacies are, anecdotally, less widely unionized and would therefore lack the organizational structure to handle complaints or discipline, leading to a higher proportion of regulatory involvement. In their review of pharmacist discipline, Phipps and others4 also speculated that this was the reason for fewer hospital discipline cases in the United Kingdom.
Hospital pharmacy directors in our study emphasized the value of collaborative practice for promoting competence and safety. Austin and Gregory,13 in their work on competence drift, noted that professional isolation or working alone increases a pharmacist’s risk of becoming disengaged from the profession, resulting in a higher risk of not meeting competence standards. They attributed this higher risk to fewer opportunities for peers to observe their practice, fewer opportunities to compare themselves with peers, and fewer role models in practice.13 Phipps and others4 also highlighted that the higher discipline rate in the community setting could reflect a higher risk when working alone compared with working in a collaborative hospital environment. Outside pharmacy, the same can be said for physicians; for example, Alam and others14,15 found that the medical specialists most likely to be disciplined in Canada were family doctors and psychiatrists, who often work alone, have more frequent patient interactions, and develop long-term relationships with their patients. Furthermore, physicians in ambulatory care settings have higher discipline rates than those working in inpatient settings, where a multidisciplinary, multispecialty team reduces risk by aiding in clinical decision-making or detecting mistakes, or where the patient may be unable to determine which clinician was responsible for an incident.16 These considerations further support the integration of hospital pharmacists into collaborative teams.
Participants’ agreement that isolated clinical incidents would not be reported to the regulator supports a previous review of pharmacist discipline, which found that most cases involved multiple or repeated violations.2 However, there was a lack of clarity among participants in our study about what would actually be reported to a regulator. For example, provinces typically require health professionals to report other health professionals if there is a concern about incompetence or incapacity, or any concern about their ability to provide care, as outlined by provincial laws, regulations, codes of ethics, and standards of practice. However, few participants in the study were able to describe the specific reporting requirements in their respective provinces.
While the organizational structure of hospitals may support competence and reduce the need for discipline, hospital processes lack transparency. Despite significant efforts to make cases of complaints and discipline involving health care professionals public, handling of cases by hospitals means that fewer hospital pharmacists have a public discipline record.
Interprovincial differences in oversight of hospitals by regulatory bodies could influence reporting to those bodies. In some provinces, hospital pharmacists are regulated by the regulatory body, but hospitals are not; it is possible that in such provinces fewer incidents involving hospital pharmacists would be reported to the regulator. In contrast, the Ontario College of Pharmacists regulates both hospitals and hospital pharmacies.17 Even so, the regulation of hospitals by this college only began in 2016, and it is possible that fewer hospital cases might be reported to the regulator in the years after such a change, as a sort of “legacy” effect as institutions adjust to the new regulatory regime.4,17
While disciplinary action by regulatory bodies aims to protect the public, other factors influence organizational discipline. For example, workplaces with a higher union presence have fewer dismissals and disciplinary sanctions.18 Also, studies of nurse discipline found that organizational discipline issues were often dealt with informally by managers and were deliberately not escalated to formal organizational discipline, to decrease costs and keep the number of disciplinary actions low.19,20 A conflict-of-interest issue arises when organizations attempt to protect both public and organizational interests.
A few limitations of our study should be considered. First, we interviewed a broad sample of hospital pharmacy directors to explore this topic across Canada, and thus could not identify granular processes within a single region. Second, the generalizability of these results may be limited, given that participants generally spoke from their experience in large hospitals. This limitation was mitigated somewhat by the inclusion of pharmacy directors who worked solely in small hospitals, but only 3 participants had this background. Third, we were unable to identify participants in all provinces, although this limitation was mitigated by the inclusion of a sample of managers from different hospital and provincial structures. Finally, our methodology was subject to certain biases, such as choosing participants on the basis of availability and the use of semi-structured interviews, whereby not every participant was asked the same set of questions.
The results of this qualitative study indicated that hospitals have clear organizational discipline processes that can support employees in maintaining competence and protect against discipline imposed by regulatory bodies. However, the study also suggests that there is both a lack of clarity about when hospitals should report pharmacists to their regulator and a lack of transparency about the reasons why hospital pharmacists are disciplined within their institutions. Specific characteristics such as collaborative practice and unionization appear to protect against disciplinary action. Future research could expand upon this study to include a larger sample, with small, medium, and large hospitals from all provinces, to gain a better understanding of hospital discipline processes in Canada and to clarify the relationship between organizational discipline and regulatory body discipline.
1 National statistics. National Association of Pharmacy Regulatory Authorities; updated 2021 Jan 1 [cited 2021 Apr 27]. Available from: https://napra.ca/national-statistics
2 Foong EA, Grindrod KA, Houle SKD. Will I lose my license for that? A closer look at Canadian disciplinary hearings and what it means for pharmacists’ practice to full scope. Can Pharm J (Ott). 2018; 151(5):332–44.
Crossref
3 Tullett J, Rutter P, Brown D. A longitudinal study of United Kingdom pharmacists’ misdemeanours—trials, tribulations and trends. Pharm World Sci. 2003;25(2):43–51.
Crossref PubMed
4 Phipps DL, Noyce PR, Walshe K, Parker D, Ashcroft DM. Pharmacists subjected to disciplinary action: characteristics and risk factors. Int J Pharm Pract. 2011;19(5):367–73.
Crossref PubMed
5 Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19(6):349–57.
Crossref PubMed
6 Hospital Pharmacy in Canada Survey Board. Hospital pharmacy in Canada report 2016/2017. Canadian Society of Hospital Pharmacists; 2018 [cited 2021 Apr 27]. Available from: https://cshp.ca/sites/default/files/HPC%20Survey/Report%202018.pdf
7 Patton MQ. Qualitative research and evaluation methods. 3rd ed. Sage Publications; 2002.
8 Gale NK, Heath G, Cameron E, Rashid S, Redwood S. Using the framework method for the analysis of qualitative data in multi-disciplinary health research. BMC Med Res Methodol. 2013;13:117.
Crossref PubMed PMC
9 Beletz E. Discipline: establishing just cause for correction. Nurs Manag. 1986;17(8):63–7.
10 Harding AD, Batista CS. Nursing practice remediation: administration and regulation. Nurs Manag. 2016;47:10–1.
Crossref
11 Julius DJ. Managing in a unionized setting. Part I: The discipline process. AORN J. 1988;48(5):919–29.
Crossref PubMed
12 Kjervik DK. Progressive discipline in nursing: abitrators’ decisions. J Nurs Adm. 1984;14(4):34–7.
Crossref PubMed
13 Austin Z, Gregory PAM. The role of disengagement in the psychology of competence drift. Res Social Adm Pharm. 2019;15(1):45–52.
Crossref
14 Alam A, Khan J, Klemensberg J, Griesman J, Bell CM. The characteristics of physicians disciplined by professional colleges in Canada. Open Med. 2011;5(4):E166–72. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3345379/pdf/OpenMed-05-e166.pdf
PubMed PMC
15 Alam A, Khan J, Liu J, Klemensberg J, Griesman J, Bell CM. Characteristics and rates of disciplinary findings amongst anesthesiologists by professional colleges in Canada. Can J Anaesth. 2013;60(10):1013–9.
Crossref PubMed
16 Liu JJ, Alam AQ, Goldberg HR, Matelski JJ, Bell CM. Characteristics of internal medicine physicians disciplined by professional colleges in Canada. Medicine (Baltimore). 2015;94(26):e937.
Crossref
17 College oversight of hospital pharmacists. Ontario College of Pharmacists; updated 2020 Aug 27 [cited 2021 May 15]. Available from: https://www.ocpinfo.com/protecting-the-public/inspections/hospital-assessments/hospital-oversight/
18 Knight KG, Latrielle PL. Discipline, dismissals and complaints to employment tribunals. Br J Ind Relat. 2000;38(4):533–55.
Crossref
19 Cooke H. Examining the disciplinary process in nursing: a case study approach. Work Employ Soc. 2006;20(4):687–707.
Crossref
20 Traynor M, Stone K, Cook H, Gould D, Maben J. Disciplinary processes and the management of poor performance among UK nurses: bad apple or systemic failure? A scoping study. Nurs Inq. 2014;21(1):51–8.
Crossref
Ariane Fung and Ai-Leng Foong-Reichert are co–first authors on this article. ( Return to Text )
Competing interests: Kelly Grindrod holds a position as Ontario College of Pharmacists Professor in Pharmacy Innovation with the University of Waterloo School of Pharmacy. No other competing interests were declared. ( Return to Text )
Funding: Ai-Leng Foong-Reichert was funded through an Ontario Graduate Scholarship. ( Return to Text )
Canadian Journal of Hospital Pharmacy , VOLUME 75 , NUMBER 2 , Spring 2022