Theresa J Schindel, Phillip Woods, Amary Mey, Michelle A King, Margaret Gray, Javiera NavarreteABSTRACT
Background
Pharmacists in many countries have long been involved in some aspect of assisted dying. Since 2016, when Canada enacted legislation permitting medical assistance in dying (MAiD), the number of patients seeking the procedure has increased yearly. Despite the global nature of pharmacists’ involvement, little is known about how they experience MAiD practice.
Objective
To study how pharmacists experience the practice of caring for patients who seek MAiD.
Methods
This qualitative study used semistructured interviews with pharmacists who had cared for patients seeking MAiD. Interviews, conducted between June 2019 and October 2020, were audio-recorded and transcribed verbatim. Data were examined using a modified framework analysis approach. Data were coded and sorted using Quirkos and Microsoft Excel software. Themes were defined through an iterative process involving constant comparison.
Results
Nineteen hospital pharmacists representing a range of practice settings in Alberta participated in the study. The experience of caring for patients seeking assistance in dying brought to light 3 themes: finding a place in the process, serving in a caring role, and bearing emotional burdens. Pharmacists’ experiences were personal, relational, emotional, and dynamic.
Conclusions
Each of the pharmacists experienced MAiD practice in a unique way. Although their roles in MAiD were primarily medication-focused, their experiences highlighted the centrality of patient choices, autonomy, and needs. The results of this study will inform pharmacists (including those not yet engaged in MAiD practice) about the role, and will also be valuable for pharmacy organizations and educators seeking to support pharmacists and the profession, as well as policy-makers seeking to expand pharmacists’ roles in MAiD.
KEYWORDS: medical assistance in dying, assisted suicide, qualitative research, pharmacists, professional role
RÉSUMÉ
Contexte
Les pharmaciens de nombreux pays participent depuis longtemps à certains aspects de l’aide médicale à mourir (AMM). Depuis que le Canada a adopté une loi l’autorisant en 2016, le nombre de patients qui demandent l’intervention a augmenté chaque année. Malgré la nature mondiale de l’implication des pharmaciens, on sait peu de choses sur la façon dont ils vivent la pratique de l’AMM.
Objectif
Étudier comment les pharmaciens vivent la pratique de la prise en charge des patients qui sollicitent l’AMM.
Méthodes
Cette étude qualitative a utilisé des entretiens semi-structurés avec des pharmaciens qui avaient pris en charge des patients ayant fait une demande d’AMM. Un enregistrement sonore des entretiens, menés entre juin 2019 et octobre 2020, a été effectué et ils ont été transcrits mot à mot. Les données ont été examinées en adoptant une approche d’analyse du cadre modifié. Les données ont été codées et triées à l’aide des logiciels Quirkos et Microsoft Excel. Les thèmes ont été définis par un processus itératif impliquant une comparaison constante.
Résultats
Dix-neuf pharmaciens d’hôpitaux représentant un éventail de milieux de pratique en Alberta ont participé à l’étude. L’expérience de la prise en charge de patients cherchant à recevoir l’aide médicale à mourir a mis en lumière 3 thèmes : trouver sa place dans le processus; jouer un rôle de proche aidant; et supporter des charges émotionnelles. Les expériences des pharmaciens étaient personnelles, relationnelles, émotionnelles et dynamiques.
Conclusions
Chaque pharmacien a vécu la pratique de l’AMM d’une manière unique. Bien que leurs rôles dans l’AMM étaient principalement axés sur la médication, leurs expériences ont mis en évidence la centralité des choix, de l’autonomie et des besoins des patients. Les résultats de cette étude informeront les pharmaciens (y compris ceux qui ne sont pas encore engagés dans la pratique de l’AMM) sur le rôle. Ils seront également précieux pour les organismes pharmaceutiques et les éducateurs cherchant à soutenir les pharmaciens et la profession, ainsi que pour les décideurs politiques qui cherchent à élargir les rôles de pharmaciens dans l’AMM.
MOTS CLÉS: aide médicale à mourir, suicide assisté, recherche qualitative, pharmaciens, rôle professionnel
Since 2016, when Canada enacted legislation permitting medical assistance in dying (MAiD), other jurisdictions around the world have introduced similar laws.1,2 For example, in Australia, numerous states have recently passed voluntary assisted dying laws or are at different stages of active parliamentary consideration.3 This increased implementation of assisted dying practice by many nations or their subjurisdictions demonstrates the effects of changing societal views and needs over time.4–6 Such developments motivate parallel changes in pharmacy practice on a global scale,7–10 including in hospitals.11,12
Pharmacists have been involved in some aspect of assisted dying since the late 1990s, including in the Netherlands, where their involvement was common even before MAiD was fully legalized.13 In Alberta, the number of MAiD provisions has increased each year since the practice became legal.14 By the end of 2020, MAiD had been provided in a total of 1507 cases in the province, 60% of them in Alberta Health Services (AHS) facilities, including hospitals.14 However, little is known about pharmacists’ roles in MAiD15 or how pharmacists experience MAiD practice. Most published research regarding roles and practice experiences has focused on physicians and nurses.16,17 In a recent mapping review, Woods and others2 demonstrated the absence of studies exploring pharmacists’ lived experiences in assisted dying practice, a finding noted by others.16,18 In Canada, pharmacists’ roles,19 knowledge and attitudes,11,20 perceptions,21,22 and positions on conscientious objection23 have been explored. Few pharmacists have been included in research exploring perceptions of allied health care professionals participating in MAiD,24 their roles,15 and the meaning of their roles.18 Given the increase in legalized assisted dying practices globally and the number of pharmacists involved in this practice, research that explores and reveals the experiences of pharmacists participating in MAiD is overdue.
This study is part of a multiphase international project seeking to explore the lived experiences of pharmacists in assisted dying practice. The first phase was conducted in Australia, where researchers gathered the perspectives of pharmacists anticipating implementation of MAiD.25 These data were developed into a theoretical framework of inquiry to study the perspectives of pharmacists experiencing MAiD practice.25 The objective of the study reported here was to explore how pharmacists experience the practice of caring for patients who seek MAiD.
Qualitative research methodology was used. The study processes closely adhered to the 32 consolidated criteria for reporting qualitative research (see Appendix 1, available at https://www.cjhp-online.ca/index.php/cjhp/issue/view/211).26 This study was approved by the University of Alberta, Research Ethics Board 1 (Pro00085742).
In 2016, the province of Alberta implemented a comprehensive MAiD program that requires a consistent, compassionate, patient-centred approach.27 Within this program, the Care Coordination Service provides a single point of contact for families and health care providers. A care navigator supports the process for practitioners, including the pharmacy team, linking them to education, resource materials, and grief and bereavement services. Pharmacists’ responsibilities touch on all steps of preparation for the procedure, which may include checking medications prepared by a pharmacy technician, dispensing medications, reviewing medications with the physician or nurse practitioner who will be providing MAiD, arranging for the preparation and delivery of medications and necessary supplies, meeting with providers to review standardized prescriptions and protocols, and documenting that legal requirements have been met.28 Pharmacists may support MAiD at their usual AHS practice sites or may need to travel to other AHS sites.
Hospital pharmacists in Alberta were eligible to participate if they had provided care for patients requesting, contemplating, or receiving MAiD (without necessarily participating in the MAiD procedure). A convenience sample29 was recruited by means of newsletters and social media of the Canadian Society of Hospital Pharmacists, Alberta Branch, as well as through information sessions presented at various AHS hospital sites. All participants provided written informed consent and received no compensation for their participation in the study.
One team member (T.J.S.) and a trained research assistant conducted the interviews in person at a location of each participant’s choice or remotely (by Skype teleconferencing software) using a predefined semistructured interview guide (Appendix 2, available at https://www.cjhp-online.ca/index.php/cjhp/issue/view/211). All interviews were audio-recorded and transcribed verbatim.
We applied a 2-phase constructivist approach to analyze the interview data.30,31 In the first phase, a modified version of the framework method described by Gale and others32 was utilized. In this study, the framework included 8 dimensions of inquiry previously designed by Woods and others25 (Appendix 3, available at https://www.cjhp-online.ca/index.php/cjhp/issue/view/211). Two researchers (T.J.S., J.N.) independently coded and sorted the data using Quirkos33 (v.2.4.28) and Excel spreadsheet software (v.16.47.1; Microsoft Corporation), then discussed the coding and interpretation of the data with a third team member (P.W.) until consensus was reached and saturation34 of the dimensions had been achieved. The second phase involved thematic analysis35 and constant comparison across participants and dimensions of inquiry.25 Reviewing, discussing, and writing activities facilitated reflexivity as team members considered their own views of MAiD practice at every stage of the research (see Appendix 1).36
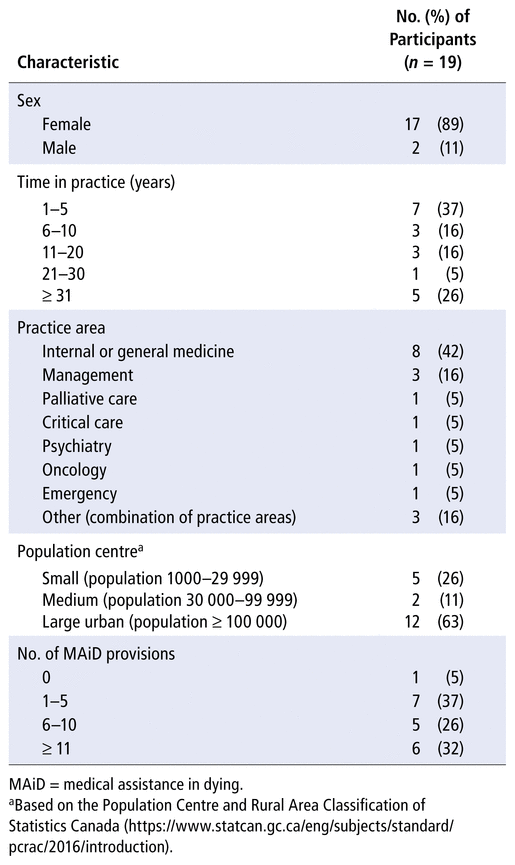
Nineteen pharmacists participated in the study between June 2019 and October 2020. Interviews lasted 30–78 minutes (average 47 minutes). Variety was evident in participants’ practice experiences and career durations, practice settings, and amount of experience with MAiD (Table 1). All participants were involved in some way with patients who were seeking MAiD. One participant objected to MAiD and did not participate in provision of this service. The analysis brought to light 3 themes representing pharmacists’ experiences: finding a place, serving in a caring role, and bearing emotional burdens. Additional supporting data are presented in Table 2.
TABLE 1 Participant Characteristics

TABLE 2 Participant Quotations by Theme

I thought okay, do I want to? … I thought about it a bit … if they [patients] have been approved, and it is appropriate, and they have made this big hard decision for themselves, and it is going to affect their family, I didn’t want it to be a barrier. (Participant 6)
Participants in this study considered their place personally and professionally within MAiD. Finding a place was an evolutionary process with respect to how participants viewed MAiD and experienced their role in relation to themselves; the patients; the pharmacy and health care teams; and their family, friends, and community. This process began with deciding if they would participate in MAiD provisions and how the role might evolve over time.
When MAiD was first implemented, participants contemplated adding their names as potential contacts for MAiD provision. Some participants decided unequivocally yes or no, whereas others felt uncertain. Several considerations influenced participants’ decisions to participate in MAiD, including personal values, beliefs about MAiD, experiences with the death of a patient or family member, and legal responsibilities of pharmacists. Patients’ stories were also important in participants’ decision-making. Other factors included compassion and respect for patients’ wishes and autonomy, knowledge of the clinical context, and familiarity with the patient through a previous relationship or current involvement with their care.
Organizational momentum created by the MAiD process itself contributed to the decision-making process for some participants, especially those in management positions or those who were the only consenting pharmacists at their practice sites. Some perceived a lack of choice and an obligation to participate when others were unavailable or unwilling. Others revisited the decision-making process each time they were contacted with a request to participate in a MAiD provision.
I guess most of our role as medical professionals is we want to treat things, we want to cure things, we want to fix things. In some cases we want to relieve things. But I mean ultimately and every time we are doing something it is because we are trying to get closer to a goal of therapy. And sometimes the goal of therapy or the goal of the patient is “I just want to feel better this way”, and in this case it is, “I just want it to end”. (Participant 3)
Caring in the context of MAiD represented a role in service of another, without sharing in the decision-making process. Pharmacists perceived themselves in a caring, patient-centred role, regardless of whether they had served in a MAiD provision. All MAiD activities were focused on serving the patients’ choices, autonomy, and needs.
Pharmacists’ roles are specified in the AHS MAiD policy,28 which outlines legal requirements, responsibilities, and expectations related to dispensing. Participants described their medication supply activities as being more technical and transactional than their other patient care responsibilities. Although supplying medications for MAiD was familiar in some ways, it felt different because pharmacists were authorizing unfamiliar doses and were performing repeated checks to ensure the medications were ready for the provision. Kits were carefully curated to contribute to a smooth and peaceful experience for patients and providers, for example, by sequencing medications according to protocols and including additional labelling or supplies.
Some participants supported MAiD provision from a distance—working in a location separate from patients, families, providers, and other team members (for example, at an adjacent location in the hospital). Some participants felt isolated and removed from the patients and team members. Others felt distanced from the provision, but not removed from the process; these participants emphasized and acknowledged their role as integral to the MAiD process and team effort.
Participants had opportunities to expand their involvement in MAiD beyond the responsibilities outlined by AHS.28 For example, they could choose to be physically present at the provision to support the patient and the provider. Some participants desired to contribute more directly to patient care throughout the MAiD process. As they gained experience with MAiD, their familiarity and confidence grew, as did their understanding of their own role and place in MAiD. It was a dynamic and evolving role. With each additional MAiD provision, the focus on the patient was more significant than the focus on the logistics associated with supplying medication.
I don’t even know if I would describe it as discomfort. I was just [unusually] affected. Did I cry? I think I did. It was sad … We are ending a life here even though imminently life is going to end. And you know that there are several ways it can end, and it can be very, very sad. It could be very traumatic, it could go very wrong, and this patient has the option to end it the day she wants and the way she wants and peacefully, painlessly, peacefully pass on and [I’m] happy for her. But it just kind of surprised [me] that I would have [gone] through the same emotions. (Participant 1)
Participants described their experiences with MAiD as involving a range of emotions. They highlighted paradoxical feelings that were difficult to reconcile: accepting the inevitability of death while confronting the emotions associated with the end of a life. Negative emotions were described as sad, heavy, exhausting, and draining. Some participants experienced positive emotions associated with knowing that they had supported a patient’s last wish or alleviated suffering.
Participating in MAiD affected pharmacists’ emotions at various points in the process, including before the procedure and while preparing, delivering, and returning medication kits, as well as during the MAiD provision itself. Many participants recalled the first provision as the most difficult, especially when they realized the gravity of their role in MAiD at some crystallizing moment. Some participants experienced a delayed emotional response in the hours and days following the provision, although emotional burdens eased over time with subsequent provisions.
Emotional burdens felt greater in certain situations, such as when participants had pre-existing relationships with patients or their family members. The emotions of others also affected participants’ experiences. Witnessing others’ struggles and experiences of grief as they participated in MAiD and observing family dynamics or disagreements contributed to a heightened emotional state. The confidentiality and sensitivity related to MAiD created a sense of secrecy. Conversations around assisted dying were often restricted to those directly involved in the provisions. Many of the participants felt they could not openly discuss their experiences with nonparticipating colleagues. Thus, some concealed their involvement, suppressed emotions, or both.
Collaborative working relationships with physicians or nurse practitioners promoted sharing of information about patients. Hearing patients’ stories from these professionals, to learn more about their conditions and clinical status, was reassuring for participants. However, the extent to which they could develop these relationships varied according to the particular work environment. Some participants were unfamiliar with other team members and patients, especially when supporting a provision at an unfamiliar site or unit. Providing and receiving support from other pharmacists and team members influenced their experiences in a positive way.
Participants took action to ease their emotional burdens. Diverting focus to a required task, such as documentation or the preparation of medication kits, helped them in the moment. To alleviate the emotional burden, some created physical distance from the provision, while others chose to participate closely in the provision. They processed their emotions following a MAiD provision through informal conversations with team members or their managers. During formal debrief sessions, they shared experiences and honoured patients. Some spoke with family members. Talking about the experience helped participants feel they were part of the provision from beginning to end and provided some closure.
We explored pharmacists’ experiences of caring for patients seeking assistance in dying. Participants revealed their experiences to be personal, relational, emotional, and dynamic. Previous qualitative research exploring other health care providers’ experiences has yielded similar findings.15 Within the theme of “finding a place”, participants’ realizations about themselves and their beliefs merged with the influences of their practice contexts as they helped care for patients seeking an assisted death. Their understanding of patients’ stories was interwoven with reflections on their own beliefs about MAiD, their personal values, and their own experiences with death. The role of personal beliefs and values in pharmacists’ decisions to participate in assisted dying was highlighted by Isaac and Chaar23 and by Peters and others.37 Realizations are shaped by contextual factors, including changes in public culture38; legal, policy, and procedural requirements28; professional ethical codes39; and practice environments.
The theme of “serving in a caring role” was related to participants’ commitment to care for patients seeking an assisted death. The role was unique, in that caring was experienced as “a way of helping people by entering their world”.40 Whether participants were physically and emotionally distant or felt integral to the provision of MAiD, they felt connected to their patients. However, an adjustment from their experience of everyday pharmacy practice was required in terms of how to provide care in the context of MAiD. The pharmacy profession has evolved, and pharmacists must now find a balance between medication supply and patient care.9 Both roles rely on collaboration and relationships with patients and other members of the health care team. The primary responsibility of pharmacists in the context of MAiD, as reported by study participants, was to supply medications. Zworth and others19 emphasized a dispensing role for pharmacists in this context. By contrast, pharmacist participants in the study by Selby and others15 emphasized clinical relationships with patients, minimizing their dispensing role. In our study, participants gave extraordinary attention to their dispensing tasks, thoroughly checking, carefully arranging, and thoughtfully transporting MAiD kits, to facilitate a smooth provision and thereby to enable a peaceful death. The dispensing role associated with MAiD stood out as a unique and meaningful experience, an active manifestation of the caring role and separate from previous experiences with medications for other purposes. In contrast, Selby and others15 reported that the 3 pharmacists in their study, all of whom had previous clinical relationships with the patients receiving MAiD, did not perceive dispensing as a part of a genuine MAiD experience.
Despite the focus on medication, participants in the current study experienced their involvement in MAiD as a caring, patient-centred role, similar to findings reported by Mills and others18 and Selby and others.15 Pharmacists provided support to others and helped to mitigate distress. Some attended provisions to support other team members, patients, and families. Participants’ roles in MAiD evolved with experience, suggesting that in the future, pharmacists may expand their roles to encompass direct interaction with patients and other responsibilities associated with MAiD.
The theme of “bearing emotional burdens” captured the emotional side of participants’ experience in MAiD practice. Emotions are fundamental to an individual’s personal and social engagement with the world.41 Emotions were described variously as out of the ordinary, both positive and negative, greater in some circumstances but less in others, sometimes immediate but at other times delayed. Emotions enable individuals to determine the gravity of an experience for themselves.42 As a unique service, MAiD has a weightiness that must be borne by those whose practice incorporates it. This theme revealed what mattered most for each participant. They spoke of their emotions easing over time as their familiarity with MAiD practice increased. Some spoke of how this change in emotional intensity drew their attention away from themselves and toward the patients and others. Verweel and others22 highlighted concerns regarding professional distress in the context of MAiD. For participants, emotional burdens were reconciled through relational means: talking with other involved caregivers, acknowledging shared experiences of active MAiD participation, and connecting with patients’ stories regarding their journeys toward a desired death. Mills and others24 reported that pharmacists found value in discussing their experiences with others involved in MAiD.
Support for professionals caring for patients seeking MAiD may be provided through carefully planned formal or informal conversations, including debriefing in an open environment where opinions and feelings may be discussed.15,24 Further consideration of ways to enhance education and training related to MAiD is warranted.2,11,15,22,42 Including MAiD in health sciences curricula and professional development programs provides opportunities for students and practising pharmacists to reflect on their roles, ponder their place in the MAiD process, and increase their preparedness.
This study contributes to the understanding of pharmacists’ roles in MAiD and the lived experiences of pharmacists, addressing previously identified gaps in the literature.2,15,22 A unique theoretical framework, based on interviews with expert and senior Australian pharmacists anticipating their experiences with assisted dying practice,25 enabled exploration of the actual roles and experiences of pharmacists. Deployment of this framework delivered new and insightful understandings of MAiD practice, including the gravity associated with the dispensing role and the emotional aspect of these experiences.22
The limitations of this study relate to the sample and the context. Participants were self-referred, all were practising in hospitals, and 1 had chosen not to participate in the provision of MAiD. While the themes embodied the experiences of all participants in this study, the sample may not have adequately captured the experiences of all pharmacists participating in the care of patients requesting MAiD. Future research would benefit from including pharmacists practising in different settings (specifically community pharmacies), those of different genders, and those objecting to MAiD.
Several changes to MAiD that came into effect with the assisted dying legislation of March 2021, including removal of the requirement that natural death be foreseeable and elimination of the 10-day reflection period in some situations,43 occurred after this study was complete. Pharmacists’ experiences with MAiD practice in situations where death is not imminent warrant investigation. Research to study the roles and experience of other pharmacy team members, including pharmacy technicians, in other jurisdictions will also facilitate deeper understanding of the influence of practice context, education, roles, and cultural norms on MAiD practice.
This study explored how hospital pharmacists experience the practice of caring for patients who seek MAiD. The experience involved an active, iterative, and reflective process concerning pharmacists’ decisions to participate in MAiD. The role focused on medication supply and documentation, yet it was experienced as a caring role in service of another’s decision and needs. Pharmacists experienced a range of emotions, both positive and negative. The results of this study will inform pharmacists about their role in MAiD and the range of experiences associated with assisted dying practice. Pharmacy educators, leaders, and policy-makers may apply these results to their own contexts to further support pharmacists and potentially expand their roles in MAiD. Further research will deepen understanding of the possibilities for pharmacists’ roles within MAiD practice.
1 Isaac S, McLachlan A, Chaar B. Australian pharmacists’ perspectives on physician-assisted suicide (PAS): thematic analysis of semistructured interviews. BMJ Open. 2019;9(10):e028868.
Crossref PubMed PMC
2 Woods P, Schindel TJ, King MA, Mey A. Pharmacy practice in the domain of assisted dying: a mapping review of the literature. Res Social Adm Pharm. 2020;16(3):267–76.
Crossref
3 White B, Willmott L. Voluntary assisted dying could soon be legal in Queensland. Here’s how its bill differs from other states. The Conversation [published by Academic Journalism Society]; 2021 May 19 [cited 2021 Aug 16]. Available from: https://theconversation.com/voluntary-assisted-dying-could-soon-be-legal-in-queensland-heres-how-its-bill-differs-from-other-states-161092
4 Emanuel EJ, Onwuteaka-Philipsen BD, Urwin JW, Cohen J. Attitudes and practices of euthanasia and physician-assisted suicide in the United States, Canada, and Europe. JAMA. 2016;316(1):79–90.
Crossref PubMed
5 Downie J. Medical assistance in dying: lessons for Australia from Canada. QUT Law Rev. 2017;17(1):127–46.
Crossref
6 Li M, Watt S, Escaf M, Gardam M, Heesters A, O’Leary G, et al. Medical assistance in dying – implementing a hospital-based program in Canada. N Engl J Med. 2017;376(21):2082–8.
Crossref PubMed
7 Marriott JL. What can be done to help the pharmacy profession advance globally? Am J Pharm Educ. 2018;82(8):908–9.
Crossref
8 Mossialos E, Courtin E, Naci H, Benrimoj S, Bouvy M, Farris K et al. From “retailers” to health care providers: transforming the role of community pharmacists in chronic disease management. Health Policy. 2015;119(5):628–39.
Crossref PubMed
9 Schindel TJ, Yuksel N, Breault R, Daniels J, Varnhagen S, Hughes CA. Perceptions of pharmacists’ roles in the era of expanding scopes of practice. Res Social Adm Pharm. 2017;13(1):148–61.
Crossref
10 Varadarajan R, Freeman RA, Parmar JR. Aid-in-dying practice in the United States: legal and ethical perspectives for pharmacy. Res Social Adm Pharm. 2016;12(4):e17.
Crossref
11 Gallagher A, Gould O, LeBlanc M, Manuel L, Brideau-Laughlin D. Knowledge and attitudes of hospital pharmacy staff in Canada regarding medical assistance in dying (MAiD). Can J Hosp Pharm. 2019; 72(1):16–26.
PubMed PMC
12 Leadership in exceptional circumstances as Voluntary Assisted Dying begins in Australia [media release]. Society of Hospital Pharmacists of Australia; 2019 Jun 20 [cited 2021 Aug 16]. Available from: https://shpa.org.au/publicassets/1a32de55-df53-ec11-80dd-005056be03d0/shpa_media_release_-_leadership_in_exceptional_circumstances_as_vad_begins_in_australia_-_20jun2019_0.pdf
13 deBoer A, Lau HS, Porsius A. Physician-assisted death and pharmacy practice in the Netherlands. N Engl J Med. 1997;337(15):1091–2.
Crossref
14 Data & statistics: medical assistance in dying. Alberta Health Services; 2021 [cited 2021 Aug 16]. Available from: https://www.albertahealthservices.ca/info/Page14930.aspx
15 Selby D, Wortzman R, Bean S, Mills A. Perception of roles across the interprofessional team for delivery of medical assistance in dying. J Interprof Care. 2021 Dec 16;1–8. doi 10.1080/13561820.2021.1997947.
Crossref PubMed
16 Brooks L. Health care provider experiences of and perspectives on medical assistance in dying: a scoping review of qualitative studies. Can J Aging. 2019;38(3):384–96.
Crossref PubMed
17 Fujioka JK, Mirza RM, McDonald PL, Klinger CA. Implementation of medical assistance in dying (MAiD): a scoping review of health care providers’ perspectives. J Pain Symptom Manage. 2018;55(6):1564–76.
Crossref PubMed
18 Mills A, Bright K, Wortzman R, Bean S, Selby D. Medical assistance in dying and the meaning of care: perspectives of nurses, pharmacists, and social workers. Health (Lond). 2021 Mar 8;1363459321996774.
19 Zworth M, Saleh C, Ball I, Kalles G, Chkaroubo A, Kekewich M, et al. Provision of medical assistance in dying: a scoping review. BMJ Open. 2020;10(7):e036054.
Crossref PubMed PMC
20 Murphy AL, O’Reilly C, Martin-Misener R, Ataya R, Gardner D. Community pharmacists’ attitudes on suicide: a preliminary analysis with implications for medical assistance in dying. Can Pharm J. 2018;151(1):17–23.
Crossref
21 Turner A, Kielly J, Bugden S, Matthews M, Davis E. Pharmacists perceptions towards their preparedness to participate in medical assistance in dying [abstract]. Can Pharm J. 2019;152(5 Suppl):S3.
22 Verweel L, Rosenberg-Yunger ZRS, Movahedi T, Malek AH. Medical assistance in dying: examining Canadian pharmacy perspectives using a mixed-methods approach. Can Pharm J. 2018;151(2):121–32.
Crossref
23 Isaac S, Chaar B. Should pharmacists be allowed to conscientiously object to medicines supply on the basis of their personal beliefs? The “pro” side. Can J Hosp Pharm. 2018;71(2):149–50.
24 Mills A, Wortzman R, Bean S, Selby D. Allied health care providers participating in medical assistance in dying: perceptions of support. J Hosp Palliat Nurs. 2020;22(3):220–8.
Crossref PubMed
25 Woods P, King MA, Mey A, Schindel TJ. “If I were to do this, how would I experience it?” Developing a theoretical framework for exploring pharmacists’ practice in the domain of assisted dying. Res Social Adm Pharm. 2021;17(4):685–93.
Crossref
26 Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19(6):349–57.
Crossref PubMed
27 Silvius JL, Memon A, Arain M. Medical assistance in dying: Alberta approach and policy analysis. Can J Aging. 2019;38(3):397–406.
Crossref PubMed
28 Policy: Medical assistance in dying. Alberta Health Services; 2016 [revised 2021; cited 2021 Aug 16]. Available from: https://extranet.ahsnet.ca/teams/policydocuments/1/clp-med-assist-in-death-hcs-165-01.pdf
29 Saumure K, Given LM. Convenience sample. In: Given LM, editor. The SAGE encyclopedia of qualitative research methods. SAGE Publications, Inc; 2008. p. 125.
30 Charmaz K. The power of constructivist grounded theory for critical inquiry. Qual Inq. 2017;23(1):34–45.
Crossref
31 Lincoln YS, Lynham SA, Guba EG. Paradigmatic controversies, contradictions, and emerging confluences, revisited. In: Denzin NK, Lincoln YS, editors. The SAGE handbook of qualitative research. 4th ed. SAGE Publications, Inc; 2011. p. 97–128.
32 Gale NK, Heath G, Cameron E, Rashid S, Redwood S. Using the framework method for the analysis of qualitative data in multi-disciplinary health research. BMC Med Res Methodol. 2013;13(1):Article 117.
Crossref PubMed PMC
33 Qualitative analysis software made simple [homepage on Internet]. Quirkos; [cited 2021 Aug 16]. Available from: https://www.quirkos.com/
34 Saunders B, Sim J, Kingstone T, Baker S, Waterfield J, Bartlam B, et al. Saturation in qualitative research: exploring its conceptualization and operationalization. Qual Quant. 2018;52(4):1893–907.
Crossref PubMed PMC
35 Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101.
Crossref
36 Amin MEK, Nørgaard LS, Cavaco AM, Witry MJ, Hillman L, Cernasev A, et al. Establishing trustworthiness and authenticity in qualitative pharmacy research. Res Social Adm Pharm. 2020;16(10):1472–82.
Crossref PubMed
37 Peters KA, Lee DS, Irwin AN. Pharmacist experiences and perspectives with Oregon’s Death with Dignity Act. J Am Pharm Assoc. 2020;60(6):874–9.
Crossref
38 Wiebe E, Green S, Wiebe K. Medical assistance in dying (MAiD) in Canada: practical aspects for healthcare teams. Ann Palliat Med. 2021;10(3):3586–93.
Crossref
39 Code of ethics. Alberta College of Pharmacy; 2009 [cited 2021 Aug 16]. Available from: https://abpharmacy.ca/code-ethics
40 Benner PE. Interpretive phenomenology: embodiment, caring, and ethics in health and illness. SAGE Publications, Inc; 1994. p. x.
41 Sherman N. Wise emotions. In: Brown WS, editor. Understanding wisdom: sources and science spiritual principles. Templeton Press; 2000. p. 319–39.
42 Brown J, Goodridge D, Thorpe L. Medical assistance in dying in health sciences curricula: a qualitative exploratory study. Can Med Educ J. 2020;11(6):e79–e89.
PubMed PMC
43 Medical assistance in dying. Government of Canada; 2021 [cited 2021 Aug 16]. Available from: https://www.canada.ca/en/health-canada/services/medical-assistance-dying.html
Competing interests: None declared. ( Return to Text )
Funding: This study was supported by the CSHP Foundation and the Quality Use of Medicines Network, School of Pharmacy and Pharmacology, Griffith University, Queensland, Australia. ( Return to Text )
The research team extends sincere gratitude to the pharmacists who gave their time and shared their experiences with medical assistance in dying, Jordan Kelly for assisting with participant recruitment and data collection, and Cathryn Gunn for editing the manuscript in advance of submission.
Canadian Journal of Hospital Pharmacy, VOLUME 75, NUMBER 4, Fall 2022