Alexandra Charlton, Cheryl Hill, Deonne Dersch-Mills, Aliaksandr Savin, Dalyce Zuk, Sydney Saunders, and Elizer ErpillaTo cite: Charlton A, Hill C, Dersch-Mills D, Savin A, Zuk D, Saunders S, et al. Changes in acute care pharmacist prescribing and laboratory ordering over time: CAPLET Study. Can J Hosp Pharm. 2024;77(4):e3565. doi: 10.4212/cjhp.3565
ABSTRACT
Background
In Alberta, pharmacists may obtain additional prescribing authorization (APA) and a practice identification number (PRAC-ID) for ordering laboratory tests. Pharmacists working within Alberta Health Services were mandated by the employer to attain APA by 2018, whereas laboratory ordering has been in place since 2009. Five acute care sites within the Calgary Zone had a computerized provider order entry (CPOE) system that allowed tracking of these activities.
Objectives
To describe changes in prescribing and laboratory ordering by acute care pharmacists over time and to compare these activities across hospitals, sites, and specialty teams.
Methods
A retrospective, descriptive review of acute care pharmacist orders for medications and laboratory tests was completed using data from the CPOE system for the period 2018 to 2021.
Results
Over the study period, the rates of prescribing and laboratory ordering by pharmacists increased by 67.5% (from 1423 to 2383 per full-time equivalent [FTE]) and by 5.5% (from 235 to 248 per FTE), respectively. Pharmacists at the 5 hospitals increased their prescribing rates during that time (by proportions ranging from 7% to 176%). Cardiology, intensive care, and mental health teams had the largest increases in prescribing rates, whereas mental health, hospitalist, and intensive care teams had the greatest increases in rates of laboratory ordering. In each year of the study, the most frequently ordered medication for adult patients was vancomycin, and the most frequently ordered laboratory test was measurement of vancomycin before dose administration. The proportion of medication orders conveyed verbally decreased from 60.0% to 47.4% over the study period.
Conclusions
The application of expanded scope of practice increased among acute care pharmacists, to a greater extent for prescribing than for laboratory ordering; however, the proportion of verbal medication orders remains high, a situation that should be addressed to improve patient safety. This study showed that prescribing and laboratory ordering are complementary, given that the top medications and laboratory tests were frequently related. The results of this study can be used for practice development and as the basis for further research within an expanded CPOE system.
KEYWORDS: pharmacist prescribing, acute care, laboratory orders, pharmacy practice, expanded scope
RÉSUMÉ
Contexte
En Alberta, les pharmaciens peuvent obtenir une autorisation de prescription élargie (APE) et un numéro d’identification de pratique (PRAC-ID) pour demander des analyses de laboratoire. Les pharmaciens travaillant dans les Services de santé de l’Alberta ont été sommés par leur employeur d’obtenir une APE avant 2018, alors que les demandes d’analyses de laboratoire sont en place depuis 2009. Cinq sites de soins aigus dans la zone de Calgary disposaient d’un système de saisie informatique des ordonnances médicales (CPOE) permettant de suivre ces activités.
Objectifs
Décrire les changements en matière de prescription et de demande d’analyses de laboratoire par les pharmaciens de soins aigus au fil du temps et comparer ces activités entre les hôpitaux, les sites et les équipes spécialisées.
Méthodologie
Un examen rétrospectif et descriptif des prescriptions de médicaments et des demandes d’analyses de laboratoire effectuées par les pharmaciens en soins aigus a été mené à l’aide des données du système de CPOE pour la période 2018 à 2021.
Résultats
Au cours de la période de l’étude, les taux de prescription et de demande d’analyses de laboratoire par les pharmaciens ont augmenté respectivement de 67,5 % (de 1423 à 2383 par équivalent temps plein [ETP]) et de 5,5 % (de 235 à 248 par ETP). Le taux de prescription des pharmaciens de tous les hôpitaux a augmenté au cours de cette période (de 7 % à 176 %). Les équipes de cardiologie, de soins intensifs et de santé mentale ont enregistré les plus fortes augmentations des taux de prescription, tandis que celles de santé mentale, de soins hospitaliers et de soins intensifs ont enregistré les plus fortes augmentations des taux de demande d’analyses de laboratoire. Chaque année de l’étude, la vancomycine était le médicament le plus fréquemment prescrit pour les patients adultes et les analyses de laboratoire les plus fréquemment demandées portaient sur la mesure de la vancomycine avant l’administration de la dose. La part des prescriptions de médicament communiquées verbalement a diminué de 60,0 % à 47,4 % au cours de la période d’étude.
Conclusions
L’application d’un champ de pratique élargi a augmenté chez les pharmaciens de soins aigus, dans une plus grande mesure pour la prescription que pour les demandes d’analyses de laboratoire. Cependant, la part des prescriptions de médicament communiquées verbalement demeure élevée – une situation qui devrait être corrigée pour améliorer la sécurité des patients. Cette étude a démontré que les prescriptions et les demandes d’analyses de laboratoire sont complémentaires, étant donné que les principaux médicaments et les principales analyses sont fréquemment liés. Les résultats de cette étude peuvent être utilisés pour le développement de la pratique et comme base pour des recherches ultérieures au sein d’un système de CPOE élargi.
Mots-clés: prescription par un pharmacien, soins aigus, demandes d’analyses de laboratoire, pratique de la pharmacie, champ d’application élargi
Pharmacists in Alberta can expand their scope of practice to include independent prescribing of medications and ordering of laboratory investigations. Since 2007, Alberta pharmacists have been able to obtain additional prescribing authorization (APA) by meeting specific requirements set out by the provincial regulatory authority.1 No other Canadian college of pharmacy has granted prescribing authority to the extent allowed in Alberta. APA allows pharmacists to prescribe all medications, except opioids and controlled substances,1 provided they inform and collaborate with the patient’s most responsible caregivers. Several studies have described the perceptions of physicians and other prescribers about this practice,2,3 as well as those of pharmacists themselves. A survey study published in 2012 showed that APA was more likely to be adopted by pharmacists in ambulatory care, those with higher education levels, and those who have colleagues with APA.4 Whereas these studies described opinions about pharmacist prescribing, it is also important to quantify pharmacists’ actual use of their advanced scope over time. We undertook this study to describe longitudinal changes in the frequency and types of medications and laboratory tests ordered by inpatient pharmacists at 5 urban acute care sites.
Inpatient pharmacists with APA previously self-reported a median of 4.2 prescriptions per week for every 10 patients, mostly antibiotics and anticoagulants.5 A review of inpatient prescribing conducted in 2017 showed that 172 hospital pharmacists had a median of 2.8 prescriptions weekly, significantly lower than what was self-reported.6 Most prescriptions were for patients in critical care, surgery, and oncology/palliative care. A subsequent analysis showed 726 prescriptions per FTE per year in pediatrics and 380 in neonatology.7 In the study reported here, we sought to objectively describe trends in prescribing from 2018, when Alberta Health Services mandated that all pharmacists in its employ get their APA.
As of 2009, Alberta pharmacists may obtain a Practice Identification Number (PRAC-ID) allowing them to order laboratory investigations. The literature on laboratory ordering by inpatient pharmacists is scarce, and it does not report frequencies or types of tests ordered.8 Surveys conducted by the American Society of Health-System Pharmacists (ASHP) have shown that therapeutic drug monitoring (TDM) by pharmacists has increased over time,9–11 whereas reports from the Canadian Society of Hospital Pharmacists (CSHP) do not provide such information.12,13 We sought to examine inpatient pharmacists’ prescribing and laboratory ordering habits to identify whether the laboratory tests that pharmacists order support the medications they prescribe.
To our knowledge, the dual perspective of examining medications and laboratory tests makes our study the first of its kind; in addition, the longitudinal aspect of this study is important because previous data reflect the behaviour of early adopters of APA, who, it can be inferred, were keen to prescribe. Although later adopters may have been reluctant to prescribe initially, following them for several years should accurately reflect both acceptance of prescribing and practice trends among all pharmacists at the study sites. The aim of this study was to determine if inpatient pharmacists increased their use of APA and PRAC-ID, reflecting increased comfort with these activities. Here, we describe the frequency and types of medications and tests ordered by pharmacists throughout the Calgary Zone.
This study, which was approved by the University of Alberta Health Research Ethics Board 3 (Pro00114367), was a retrospective, descriptive review of data on medication and laboratory ordering obtained from Sunrise Clinical Manager, a computerized provider order entry (CPOE) system used by inpatient pharmacists at all 5 acute care sites within the Calgary Zone of Alberta Health Services. These academic tertiary hospitals are Foothills Medical Centre, Peter Lougheed Centre, South Health Campus, Rockyview General Hospital, and Alberta Children’s Hospital. The CPOE system was used to extract orders entered by pharmacists, on their own or on behalf of others (e.g., verbal orders). Only orders that a pharmacist entered on their own behalf were subject to the full analysis. User name, requester name, order status, order names (CPOE codes), time of order, visit type, bed location, and attending group were all data points for extraction. Schedules were used to identify inpatient pharmacists, their clinical teams, and clinical shifts to calculate annual inpatient clinical full-time equivalents (FTEs) at the site, team, and individual level. Pharmacists’ clinical shifts were tallied, then divided by the maximum number of shifts possible per year and per team, accounting for vacation, sick, and personal time, as well as cross-coverage of areas. The inpatient clinical FTE numbers excluded ambulatory and emergency department pharmacists, as well as dispensary pharmacists. The sample for the study was one of convenience, including all inpatient clinical pharmacists, and was estimated to be in the range of 170 to 180 pharmacists per year.
For the purpose of our analysis, an order was defined as any change to an individual order, including initiation, discontinuation, hold, or re-order, implemented by a Calgary pharmacist using the CPOE system from January 1, 2018, to December 31, 2021. Differentiation between order type could not be completed accurately due to restrictions within the CPOE system. Parenteral nutrition, patch removals, refills, and study drugs were all excluded because they are solely dispensary activities. Orders entered between 1800 and 0500 were excluded because there were no inpatient clinical pharmacist shifts during that period.
To determine our primary outcome, we looked at yearly changes in the number of orders by pharmacists, the types of medications and laboratory tests most frequently ordered, and the percentage of pharmacists who ordered a laboratory test or medication at least once during the year. Our secondary objectives included describing ordering patterns by site and clinical team in 2018 compared with 2021. Team orders were determined by filtering the data by the units for which each team provided clinical coverage. For the team-specific comparisons, we analyzed the data for teams common to all adult sites and those large enough to protect anonymity: cardiology, critical care (intensive care unit [ICU]), medicine, hospitalist, mental health, and surgery. We also determined and compared the percentages of verbal medication orders (orders entered on behalf of another prescriber) and those independently prescribed.
The MedCalc “comparison of two rates” calculator (MedCalc Software Ltd) was used to determine differences in ordering rates per inpatient clinical FTE in 2018 compared with 2021. Z-score tests for 2 population proportions were performed to determine differences in proportional outcomes. For secondary outcomes, we adjusted for multiple comparisons using Bonferroni tests. Statistical significance was defined as p < 0.05.
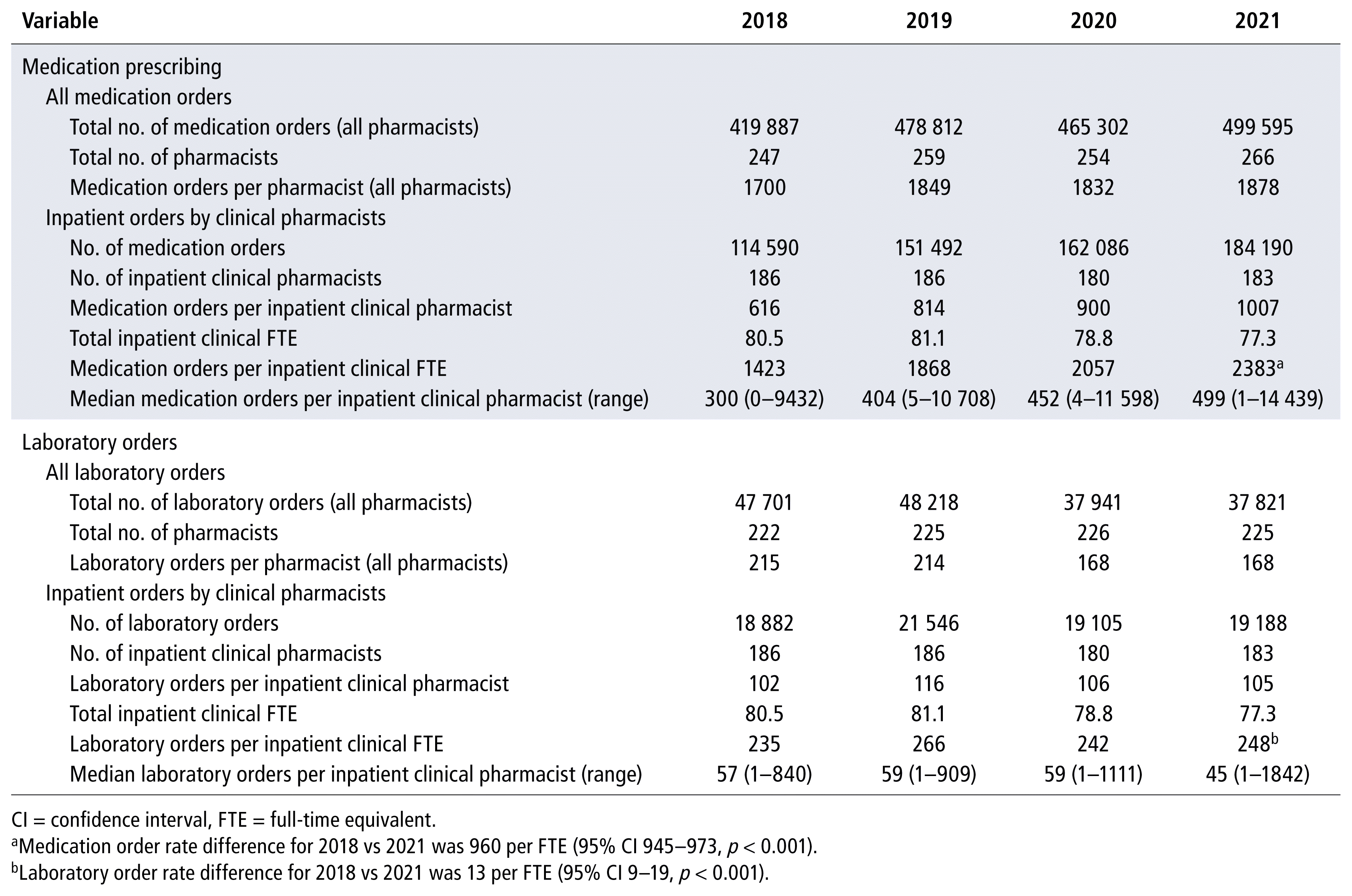
Totals of 1 863 596 medication orders and 171 681 laboratory orders were narrowed according to the exclusion criteria. For secondary outcomes, orders in 2018 and 2021 were further sorted by hospital and by clinical pharmacy team within each hospital. Pharmacist-prescribed medication orders increased each year, from 114 590 (1423 per FTE) in 2018 to 184 190 (2383 per FTE) in 2021, which represented a 67.5% increase in the per-FTE rate (absolute difference 960 per FTE, 95% confidence interval [CI] 945–973 per FTE, p < 0.001) (Table 1). The median number of medication orders by an individual pharmacist also increased, from 300 to 499. The annual number of laboratory orders increased from 18 882 in 2018 to 19 188 in 2021, which represented a 5.5% increase in the per-FTE rate, from 235 to 248 per FTE (absolute difference 13 [95% CI 9–19] per FTE, p < 0.001).
TABLE 1 Yearly Medication and Laboratory Orders, 2018 to 2021

The percentage of pharmacists prescribing at least once was 89.8% (167/186) in 2018, 93.0% (173/186) in 2019, 96.7% (174/180) in 2020, and 94.5% (173/183) in 2021. The difference between 2018 and 2021 was nonsignificant (z = –1.6955, p = 0.09). The percentage of pharmacists who ordered laboratory tests at least once was 89.2% (166/186) in 2018, 88.2% (164/186) in 2019, 94.4% (170/180) in 2020, and 92.3% (169/183) in 2021. Again, the difference between 2018 and 2021 was nonsignificant (z = 1.0302, p = 0.30).
Prescribing patterns across adult sites and teams showed little variation and are therefore reported as a group. Vancomycin for injection, acetaminophen, and polyethylene glycol (PEG) 3350 accounted for the largest proportions of orders in both 2018 and 2021 (Table 2). Bio-K Plus (probiotic) was the fourth most frequently ordered product in 2018, but was replaced in that position by tinzaparin in 2021, likely because an antimicrobial stewardship initiative that had been in place in 2018 was not continued. Warfarin, which was in sixth place in 2018, also fell out of the top 10 in 2021, seemingly replaced by acetylsalicylic acid (ASA) in 2021’s top 10 list. Pantoprazole, senna, piperacillin–tazobactam, lactulose, and prednisone were also on the top 10 lists in both years.
TABLE 2 Ten Most Common Medication and Laboratory Test Orders, 2018 and 2021
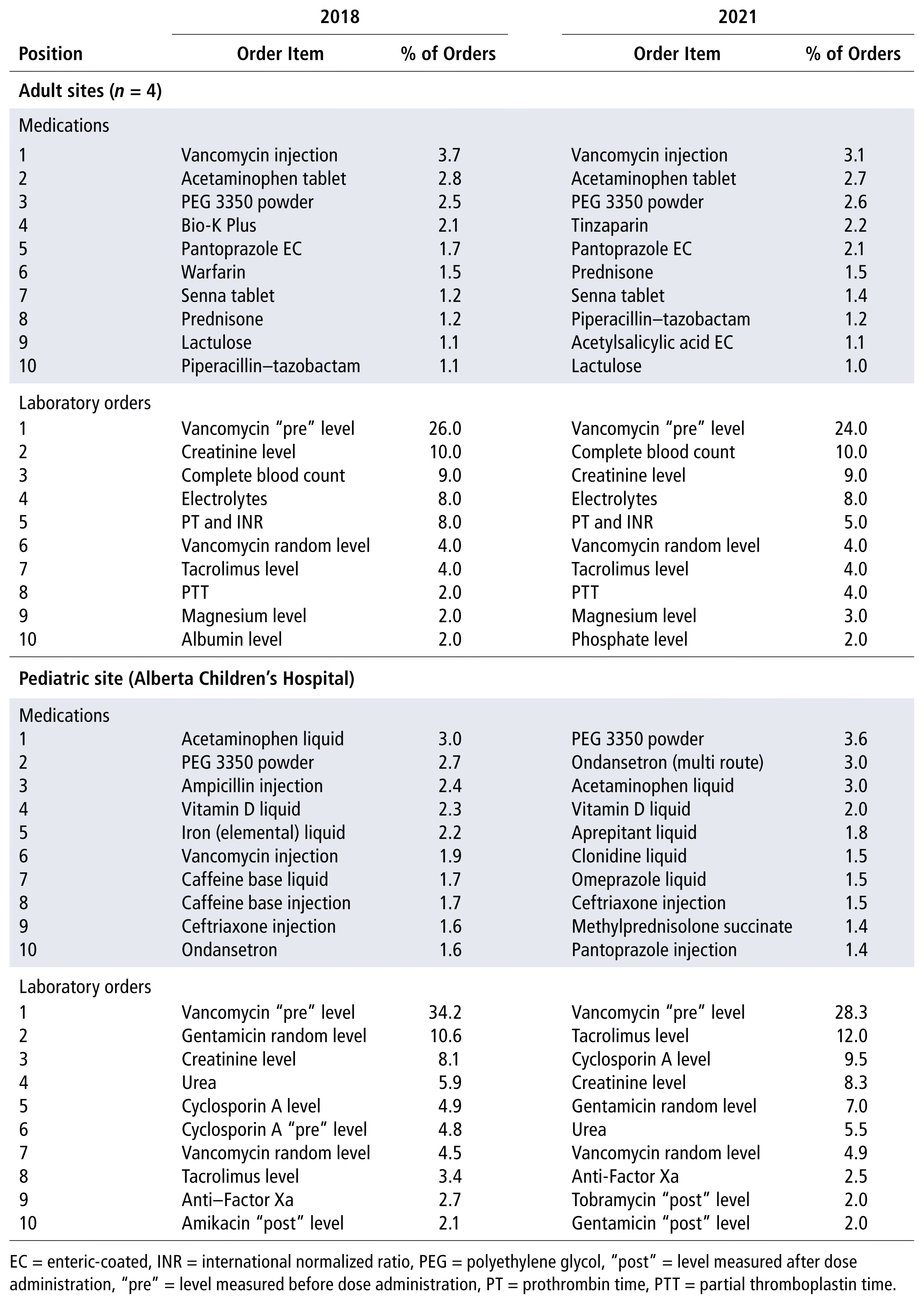
Laboratory ordering was consistent between the 2 years and was similar across the adult sites and among similar teams (Table 2). Measurement of vancomycin before dose administration (“pre” level) was the most frequently ordered laboratory test in both 2018 and 2021, representing a quarter of pharmacist laboratory orders each year. Other tests in the top 10 each year were serum creatinine, complete blood count, electrolytes, prothrombin time and international normalized ratio (PT/INR), vancomycin random level, tacrolimus level, partial thromboplastin time, and magnesium level; albumin, the 10th most frequently ordered test in 2018, was replaced in 10th spot by phosphate in 2021. The patterns of prescribing and laboratory ordering were substantially different at the sole pediatric site, reflecting the different dosage forms and afflictions more common to childhood. The top pediatric medication prescribed at Alberta Children’s Hospital was acetaminophen liquid in 2018 and PEG 3350 in 2021. The top antibiotic was ampicillin in 2018, but ceftriaxone in 2021. In 2021, pediatric pharmacists also regularly ordered aprepitant liquid, clonidine liquid, omeprazole liquid, and methylprednisolone succinate injection. Top laboratory tests at the pediatric site were mostly TDM levels in both 2018 and 2021.
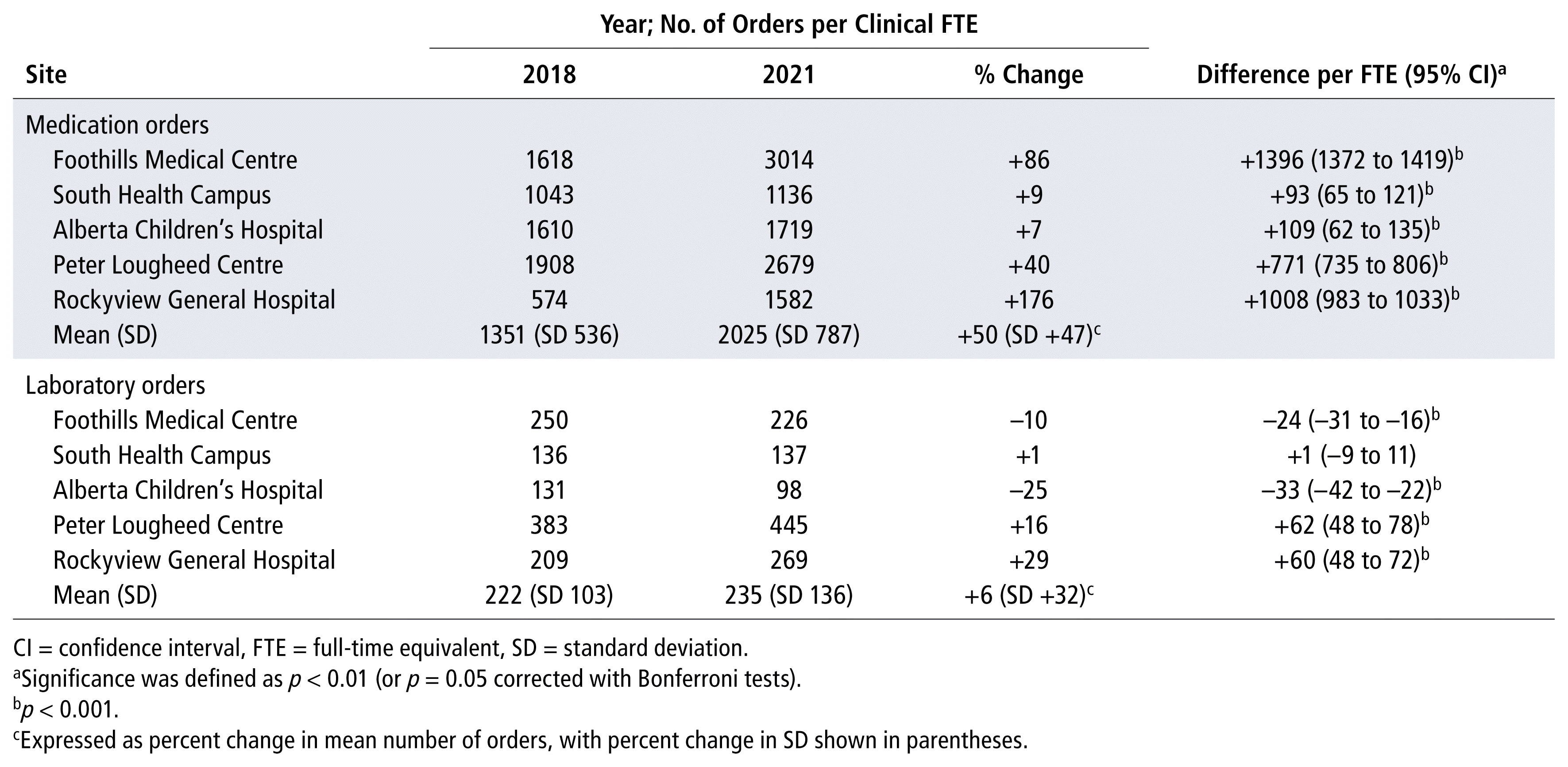
Pharmacist prescribing rates increased over the study period at all hospitals, although to differing extents (Table 3). Rockyview General Hospital had the largest increase (by 176%), while Alberta Children’s Hospital had the smallest increase (by 7%). Across sites, both the mean and the standard deviation of prescribing increased to a similar extent from 2018 to 2021, which suggests little change in the variability of prescribing among sites over time.
TABLE 3 Medication Order Rates by Site, 2018 and 2021
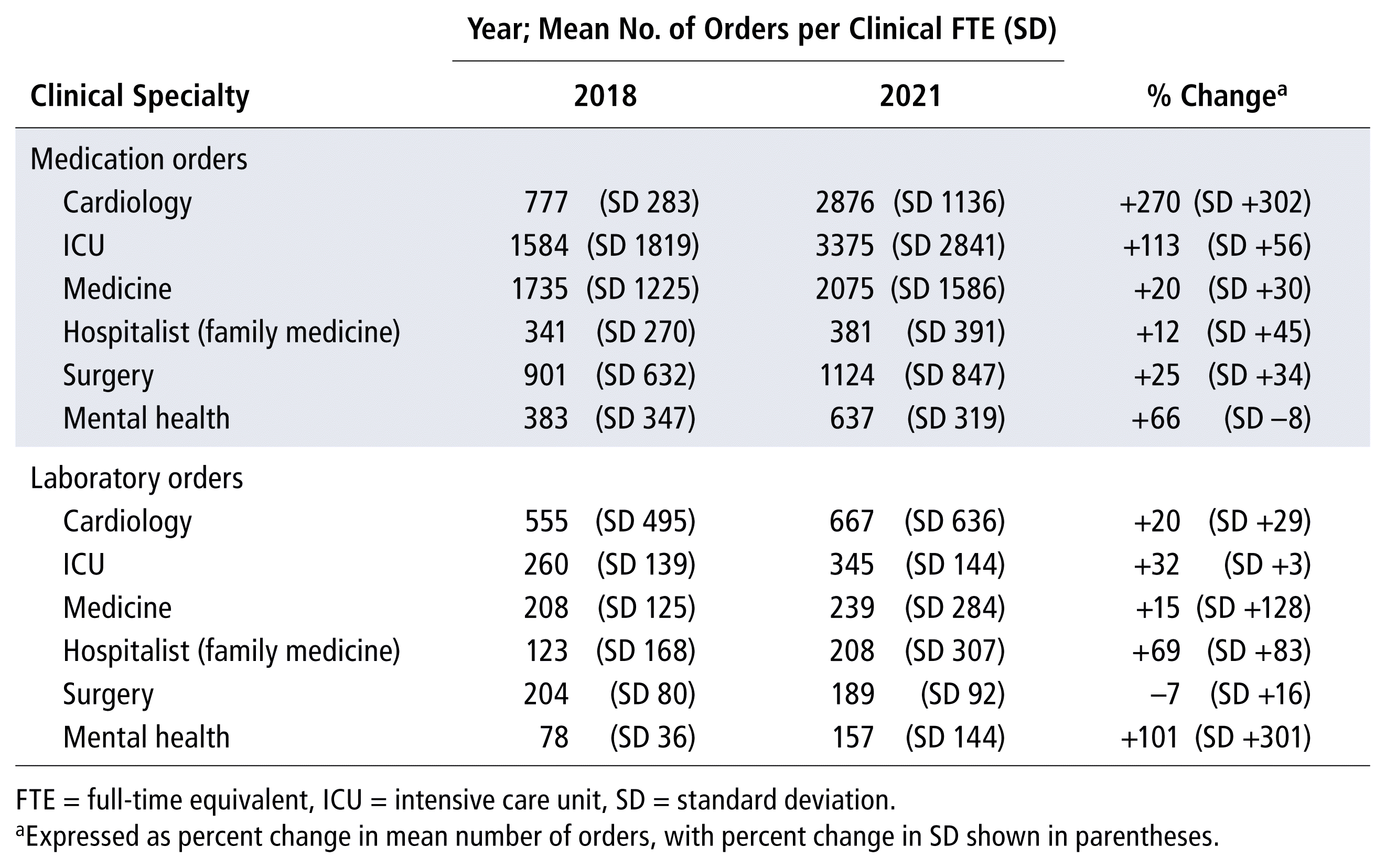
All of the clinical teams increased their average prescribing over time, while most of the teams increased their laboratory ordering rates (Table 4). The largest increase in prescribing rate was seen for the cardiology teams. The mental health teams had an increase in prescribing rate and a decrease in standard deviation, which suggests increasing use of APA with decreased variability in prescribing among sites. For laboratory ordering, the surgery team was the only group that did not show an overall increase in laboratory ordering, with each site showing no significant changes over time.
TABLE 4 Changes in Order Rates by Clinical Specialty at Adult Sites, 2018 and 2021
The percentage of pharmacist-initiated medication orders entered on behalf of another prescriber decreased from 2018 to 2021. After all exclusion criteria were applied, the percentage of prescriptions for which a pharmacist ordered medications on behalf of another prescriber was 60.0% (171 998/286 588) in 2018 and 47.4% (166 162/350 352) in 2021 (z = 100.15, p < 0.001).
In this study, we tracked changes in prescribing and laboratory ordering by pharmacists over multiple years in 5 tertiary hospitals. The primary outcome was statistically significant, with a 67.5% increase in prescribing rate and a 5.5% increase in laboratory ordering rate from 2018 to 2021. The minor increase in laboratory ordering may reflect relatively high comfort with the practice over the entire study period, as it has been available since 2009, whereas APA was not a requirement of employment until 2018. The major increase in prescribing rates, the increase in the proportion of pharmacists prescribing, and the decrease in the proportion of verbal orders suggest that pharmacists have increased their use of APA since the mandate came into effect in 2018. Our study affirms the position statements of the Canadian Pharmacists Association14 and the International Pharmaceutical Federation, 15 which support inpatient pharmacists’ increased accountability and participation in prescribing medications.
This examination of prescribing and laboratory ordering by inpatient pharmacists appears to be the first of its kind in the literature. Pharmacist-ordered laboratory tests are ideally used to assess and monitor the medications that pharmacists prescribe, and that appears to have been the case here, with vancomycin being the most frequently prescribed medication and vancomycin levels the most frequently ordered laboratory tests. This situation was also observed with warfarin prescriptions and PT/INR ordering, whereby the frequency of both decreased over time as direct oral anticoagulants were introduced. Our findings suggest that pharmacist prescribing of medications and ordering of laboratory tests are complementary activities in the overall provision of care. Commonly used order sets, through which laboratory tests and medications are ordered concurrently, are useful in ensuring this complementarity. Our results align with the findings of ASHP surveys, which have demonstrated an increase in pharmacists’ involvement in TDM over time9–11; for example, in 97.3% of hospitals surveyed in 2018, pharmacists routinely monitored medication concentrations or their surrogate markers.11 Our study showed that pharmacists were highly involved in TDM, in that ordering of tests to check vancomycin levels, tacrolimus levels, and PT/INR were among the top laboratory tests at all sites. The same connection can be seen with laboratory investigations, whereby tests such as serum creatinine, electrolytes, and complete blood count were among the top laboratory tests ordered each year and are also important to both prescribing and monitoring medications.
A survey of hospital pharmacists conducted in 2014 showed that pharmacists self-reported prescribing mostly anticoagulants and anti-infectives,5 whereas a quantitative review of pharmacist orders conducted in 2017 found that the most frequently prescribed drug classes were gastrointestinal drugs, central nervous system (CNS) agents, and anti-infectives.6 The latter 3 classes were well represented in our study, with the top gastrointestinal drugs being PEG 3350, pantoprazole, senna, and lactulose, the top anti-infectives being vancomycin and piperacillin–tazobactam, and the top CNS agent being acetaminophen, all of which were consistently prescribed in both 2018 and 2021. Anti-coagulants and antiplatelet agents were also heavily prescribed, with warfarin being part of the list in 2018 and tinzaparin and ASA in 2021. Thus, our study demonstrates the pharmacist’s role in providing expertise with anti-microbial stewardship, comfort measures, anticoagulation, and prophylaxis for deep vein thrombosis. These results may be useful to help explore the reasons why pharmacists prescribe these medications and the prescribing role they take within care teams.
Our secondary outcomes reveal proportional changes among sites and teams, with some notable observations. Although prescribing rates increased at all hospitals, they increased by differing proportions (7%–176%). The overall frequency of ordering laboratory tests increased from 2018 to 2021, but the increase was driven mostly by increases at only 2 sites. Finally, out of all the teams, the cardiology, ICU, and mental health teams had the highest increases in prescribing rates, while there was relatively little change in the hospitalist (family medicine) teams. These differences may be explained by the interplay of factors at the site, team, patient, and pharmacist levels. Site factors could include the workplace environment and initiatives that may support or inhibit the incorporation of APA or PRAC-ID into practice. Team factors may include team dynamics, the teams’ collaborative nature (rounding or non-rounding), pharmacists entering orders on behalf of other team members as a convenience, and the workload of each individual pharmacist within a team. At the patient level, acuity differs for each clinical team, with differing needs for medication changes and laboratory monitoring. At the pharmacist level, factors may include attitudes toward expanded practice, such as those shown in a survey of ambulatory oncology pharmacists conducted in 2016, which listed competence, self-confidence, and the potential impact on patient care or perceived impact on the work environment as factors that facilitated the use of APA.16 This aligns with the top 3 identified enablers of APA use: interdisciplinary team dynamics, competence, and perceived impact on patient care.5 From our data, the site that had the most changes in staff over the study period, Rockyview Hospital, also had the greatest change in prescribing, whereas the site with the least change in prescribing, Alberta Children’s Hospital, had comparatively minimal staffing changes; however, we did not do a quantitative analysis to look for other specific reasons for differences over time. Further research is needed to explore factors that enable or constrain pharmacists in prescribing medications and ordering laboratory tests.
An unexpected result in this study was the high proportion of verbal medication orders. That this only decreased from 60.0% in 2018 to 47.4% in 2021 was surprising, given that a provincial policy regarding verbal orders was issued in February 2018, stating that verbal orders “shall only be accepted … in an emergency situation or an urgent situation where delay in treatment would place a patient at risk of serious harm, and it is not feasible for the prescriber to document the medication order”.17 One possible reason for entering an order for another prescriber could be to increase efficiency, as the rounding teams appeared to do this more frequently than other teams. Another possible reason is that pharmacists who are integrated within tightly functioning teams do not prescribe (but may enter prescriptions into the CPOE system) because their recommendations are integrated into other prescribers’ orders.18 The high proportion of verbal medication orders is a safety issue that requires further investigation by leadership.
This study addressed limitations in the previous literature by taking advantage of a unified CPOE system, but there were still several limitations. For the team comparisons, orders were filtered according to their associated hospital units; as a result, numbers may have been underestimated, because some patients may be on a different unit that does not typically have coverage. Other exclusions were implemented to specifically reflect the activities of inpatient clinical pharmacists, but it is possible that some remaining orders reflected a dispensary activity; if so, our results may have been slightly elevated, as the data were standardized in terms of clinical FTEs. A further limitation was the inability to capture laboratory test orders called in by telephone; as such, our numbers may be conservative, as it is common practice to add telephone laboratory orders to previously documented orders. Lastly, the COVID-19 pandemic may have affected orders in 2020 and 2021. Changes during the pandemic may have included decreased staffing and clinical coverage, as well as unit-specific changes that could not be tracked.
Inpatient clinical pharmacists can use this study to reflect on their own use of their expanded scope of practice, as well as to compare it with the practices of other teams and other sites. At a systems level, managers and clinical practice leaders may use our findings as the basis for quality improvement or standardization of clinical practice. Further research is needed to explore qualitative aspects of pharmacist prescribing and laboratory ordering, such as the appropriateness of prescriptions, the impact of expanded scope, and the contexts in which pharmacists are enabled or constrained in using their practice privileges.
This study has laid the groundwork in showing changes in prescribing and ordering of laboratory tests over time at the city, site, and team level since APA was made a requirement for practice within Alberta Health Services. More specifically, Calgary acute care pharmacists increased their use of expanded scope of practice from 2018 to 2021, with a greater increase in medication prescribing than laboratory ordering. This study showed that the pharmacists used laboratory orders to support their prescribing. We can therefore conclude that these 2 activities are complementary and possibly essential in managing medications. Our study has also shown what pharmacists most frequently order, which underscores their expertise in managing certain aspects of care, such as antimicrobial stewardship, comfort measures, and anticoagulation. A significant safety concern was also identified, specifically the continued entry of verbal orders on behalf of another practitioner, which is a breach of the organization’s policies. Although our results do not demonstrate quality of care, they provide an objective standard that could fuel individual or systemic change. Further research is needed to explore the factors that enable or constrain pharmacists in using their practice privileges more often.
1 Gray M, Mysak T. The road to pharmacist prescribing in Alberta Health Services. Am J Health Syst Pharm. 2016;73(18):1451–5.
Crossref PubMed
2 Faruquee CF, Khera AS, Guirguis LM. Family physicians’ perceptions of pharmacists prescribing in Alberta. J Interprof Care. 2020;34(1):87–96.
Crossref
3 Donald M, King-Shier K, Tsuyuki RT, Al Hamarneh YN, Jones CA, Manns B, et al. Patient, family physician and community pharmacist perspectives on expanded pharmacy scope of practice: a qualitative study. CMAJ Open. 2017;5(1):E205–E212.
Crossref PubMed PMC
4 Hutchison M, Lindblad A, Guirguis L, Cooney D, Rodway M. Survey of Alberta hospital pharmacists’ perspectives on additional prescribing authorization. Am J Health Syst Pharm. 2012;69(22):1983–92.
Crossref PubMed
5 Heck T, Gunther M, Bresee L, Mysak T, Mcmillan C, Koshman S. Independent prescribing by hospital pharmacists: patterns and practices in a Canadian province. Am J Health Syst Pharm. 2015;72(24):2166–75.
Crossref PubMed
6 Saunders S, Dersch-Mills D, Mysak T, Romonko-Slack L, Chernick A, Lazarenko G, et al. CAPABLE: Calgary Zone usage of additional prescribing authorization by pharmacists in an inpatient setting: review of the prescribing landscape and environment. Res Social Adm Pharm. 2020;16(3):342–8.
Crossref
7 Barton A, Dersch-Mills D, Saunders S, Mysak T, Zuk D. Pharmacist prescribing in pediatric and neonatal acute care: an observational study. J Pediatr Pharmacol Ther. 2020;25(7):600–5.
PubMed PMC
8 Donovan J, Tsuyuki RT, Al Hamarneh YN, Bajorek B. Barriers to a full scope of pharmacy practice in primary care: a systematic review of pharmacists’ access to laboratory testing. Can Pharm J (Ott). 2019; 152(5):317–33.
Crossref PubMed PMC
9 Pedersen CA, Schneider PJ, Scheckelhoff DJ. ASHP national survey of pharmacy practice in hospital settings: monitoring and patient education—2012. Am J Health Syst Pharm. 2013;70(9):787–803.
Crossref PubMed
10 Pedersen CA, Schneider PJ, Scheckelhoff DJ. ASHP national survey of pharmacy practice in hospital settings: monitoring and patient education—2015. Am J Health Syst Pharm. 2016;73(17):1307–30.
Crossref PubMed
11 Pedersen CA, Schneider PJ, Ganio MC, Scheckelhoff DJ. ASHP national survey of pharmacy practice in hospital settings: monitoring and patient education—2018. Am J Health Syst Pharm. 2019;76(14):1038–58.
Crossref PubMed
12 Hospital Pharmacy in Canada Survey Board. Hospital pharmacy in Canada report 2016/17. Canadian Society of Hospital Pharmacists; 2018 [cited 2024 Jul 30]. Available from: https://www.cshp.ca/docs/pdfs/Report%202018.pdf
13 Lo E, Rainkie D, Semchuk WM, Gorman SK, Toombs K, Slavik RS, et al. Measurement of clinical pharmacy key performance indicators to focus and improve your hospital pharmacy practice. Can J Hosp Pharm. 2016;69(2):149–55.
PubMed PMC
14 CPhA position statement on pharmacist prescribing. Canadian Pharmacists Association; 2011 [cited 28 May 2022]. Available from: http://www.pharmacists.ca/cpha-ca/assets/File/cpha-on-the-issues/PPPharmacistPrescribing.pdf
15 Revised FIP Basel statements on the future of hospital pharmacy. International Pharmaceutical Federation; 2014 [cited 28 May 2022]. Available from: https://www.fip.org/files/content/pharmacy-practice/hospital-pharmacy/hospital-activities/basel-statements/fip-basel-statements-on-the-future-of-hospital-pharmacy-2015.pdf
16 Au B, Dersch-Mills D, Ghosh S, Jupp J, Chambers C, Cusano F, et al. Implementation of additional prescribing authorization among oncology pharmacists in Alberta. J Oncol Pharm Pract. 2019;25(3):584–98.
Crossref
17 Verbal and telephonic medication orders [procedure]. Alberta Health Services; 2018 [cited 22 May 2022]. Available from: https://extranet.ahsnet.ca/teams/policydocuments/1/clp-verbal-telephonic-medication-orders-ps-93-02-procedure.pdf
18 Guirguis LM, Makowsky MJ, Hughes CA, Sadowski CA, Schindel TJ, Yuksel N. How have pharmacists in different practice settings integrated prescribing privileges into practice in Alberta? A qualitative exploration. J Clin Pharm Ther. 2014;39(4):390–8.
Crossref PubMed
Address correspondence to: Dr Alexandra Charlton, Alberta Health Services, Rockyview Inpatient Pharmacy, 7007 14th Street SW, Calgary AB T2V 1P9, email: AlexandraS.Charlton@albertahealthservices.ca
Competing interests: For activities unrelated to the study reported here, Alexandra Charlton has received writing fees from the Canadian Pharmacists Association. No other competing interests were declared.
Funding: None received.
Submitted: November 23, 2023
Accepted: March 28, 2024
Published: October 9, 2024
© 2024 Canadian Society of Hospital Pharmacists | Société canadienne des pharmaciens d’hôpitaux
Canadian Journal of Hospital Pharmacy, VOLUME 77, NUMBER 4, 2024