
Alison Bentley, Celia L Culley, and Valeria StoynovaTo cite: Bentley A, Culley CL, Stoynova V. Counting the carbon: quantifying financial and environmental implications of wasted inhaler doses in the hospital setting. Can J Hosp Pharm. 2025;78(2):e3606. doi: 10.4212/cjhp.3606
ABSTRACT
Background
Inhalers contribute to health care–related environmental impacts, particularly through greenhouse gas emissions. They are dispensed in multidose formats, which leads to waste, yet little is known about the environmental impact of inhaler waste in the hospital setting.
Objectives
The primary objective was to quantify wasted inhaler actuations on adult medicine and respiratory wards at a community and a tertiary hospital. Secondary objectives were to quantify the cost and carbon footprint of wasted doses, to determine the rate of duplicate inhaler dispensing, and to quantify the prevalence of dispensed inhalers remaining unused.
Methods
For this multicentre, retrospective chart review, the pharmacy informatics team generated a report of adult inpatients for whom one or more inhalers were dispensed from the pharmacy to the respiratory and general medicine wards at a 500-bed tertiary hospital or to the medicine–surgery ward at a 48-bed community hospital over 3 nonconsecutive months (during fiscal year 2021/22). The number of inhalers dispensed was compared with the number of doses documented on patients’ medication administration records.
Results
In this study, 23 031 actuations (211 inhalers) were dispensed for 132 patients. Of these, 81.9% were wasted, at a total cost of $6172.82 over the 3 months of the study. For 22 patients (16.7%), at least one inhaler was dispensed, yet no doses were administered; for 16 (12.1%), a duplicate inhaler was dispensed. The carbon footprint of the wasted doses was 1 226 342 g carbon dioxide equivalent, equivalent to driving 5951 km by car.
Conclusions
This study showed significant inhaler waste in the hospital setting, which contributes to the health care–related carbon footprint without contributing to patient care. These results raise important questions about how to continue providing high-quality patient care while minimizing carbon footprint and health care costs.
Keywords: drug waste, multidose medications, inhalers, greenhouse gas emissions, climate change
RÉSUMÉ
Contexte
Les inhalateurs contribuent aux impacts environnementaux liés aux soins de santé, notamment par les émissions de gaz à effet de serre. Ils sont délivrés en formats multidoses, ce qui entraîne du gaspillage, mais on ne connaît que peu de choses sur l’impact environnemental du gaspillage d’inhalateurs en milieu hospitalier.
Objectifs
L’objectif principal consistait à quantifier le nombre de pulvérisations gaspillées dans les services de médecine adulte et de pneumologie d’un hôpital communautaire et d’un hôpital tertiaire. Les objectifs secondaires consistaient quant à eux à quantifier le coût et l’empreinte carbone des doses gaspillées, à déterminer le taux de distribution d’inhalateurs en double et à quantifier la prévalence des inhalateurs délivrés, mais non utilisés par les patients.
Méthodologie
Pour cette étude rétrospective multicentrique basée sur l’examen des dossiers, le service informatique de la pharmacie a produit un rapport sur les patients adultes hospitalisés à qui la pharmacie des services de pneumologie et de médecine générale d’un hôpital tertiaire de 500 lits ou du service de médecine-chirurgie d’un hôpital communautaire de 48 lits avait délivré au moins un inhalateur au cours de trois mois distincts (pendant l’exercice 2021–2022). Le nombre d’inhalateurs délivrés a été comparé au nombre de doses documentées dans les fiches d’administration des médicaments des patients.
Résultats
Dans cette étude, 211 inhalateurs (23 031 pulvérisations) ont été délivrés pour 132 patients. Parmi ce nombre, 81,9 % des pulvérisations ont été gaspillées, pour un coût total de 6 172,82 $ sur les trois mois à l’étude. Pour 22 patients (16,7 %), au moins un inhalateur a été délivré sans qu’aucune dose n’ait été administrée; pour 16 patients (12,1 %), un inhalateur a été délivré deux fois. L’empreinte carbone des doses gaspillées s’élevait à 1 226 342 grammes d’équivalent dioxyde de carbone, soit l’équivalent de 5951 km parcourus en voiture.
Conclusions
Cette étude a mis en évidence un gaspillage important d’inhalateurs en milieu hospitalier, qui contribue à l’empreinte carbone des soins de santé, sans contribuer aux soins pour les patients. Ces résultats soulèvent des questions importantes sur la manière de continuer à offrir des soins de haute qualité, tout en réduisant l’empreinte carbone et les coûts pour les soins de santé.
Mots-clés: gaspillage de médicaments, médicaments multidoses, inhalateurs, émissions de gaz à effet de serre, changement climatique
Climate change is increasingly affecting human health on a global scale.1 Canada is no exception; critical climate events such as wildfires, floods, and heat domes lead to increasing rates of respiratory disease, cardiovascular disease, and mental health complications.2 These illnesses in turn lead to additional strain on an already overburdened system through increased health care utilization3 and supply chain disruptions.4
In a vicious cycle, the health care system is exacerbating the ongoing climate crisis through outsized carbon emissions.2 The Canadian health care system is the third largest greenhouse gas (GHG) emitter per capita worldwide, producing 33 billion tonnes of carbon dioxide equivalent (t CO2 eq) annually, which represents just under 5% of national GHG emissions.5 A quarter of these emissions are directly related to prescription and nonprescription medications,5 which makes pharmacy professionals uniquely well positioned to promote sustainable health care practices. National organizations such as the Canadian Society of Healthcare-Systems Pharmacy (formerly the Canadian Society of Hospital Pharmacists) and the Canadian Association of Pharmacy for the Environment are addressing opportunities for sustainable pharmacy practices, and there is increased uptake of climate-resilient and low-carbon pharmacy initiatives.6,7
Among the targets of possible interventions, inhalers have been singled out for their outsized climate impact. On a macro scale, inhalers contribute disproportionately to the health care–related carbon footprint. For example, one study from the United Kingdom indicated that 3.5% of the entire carbon footprint of the National Health Service is related exclusively to metered-dose inhalers (MDIs).8
Three multidose inhaler device categories are currently available in Canada: MDIs, dry powder inhalers (DPIs), and soft mist inhalers (SMIs). MDIs contain hydrofluoroalkane, a potent GHG responsible for delivering the active ingredient with each actuation. Depending on the type and volume of propellant per device, each MDI can have the carbon footprint equivalent of a typical Canadian gasoline-powered car travelling between 47 and 169 km.9 DPIs and SMIs rely on the patient’s inspiratory capacity or a spring-loaded mechanism, respectively, to deliver medication to the lungs. The absence of GHG propellant in these devices creates a substantially smaller carbon footprint (by the equivalent of 1.4 to 33 km per device).9 However, it is important to consider impacts in other environmental spheres; for example, SMIs, DPIs, and, to a lesser extent, MDIs all have impacts on marine eutrophication and fossil depletion due to raw material procurement and production.10,11
Recommendations for climate-conscious inhaler practices are increasingly available, including society position statements,12,13 clinical practice guidelines,14 and knowledge translation tools.15,16 In the outpatient setting, interventions focus on confirming the diagnosis, trialling low-carbon options where appropriate, emphasizing inhaler technique, and promoting safe disposal practices.15,17
In the hospital setting, inhalers are a necessary and irreplaceable part of care, yet inhaler waste and inhaler loss are known to contribute disproportionately to climate impact without adding to patient care.1 Depending on the local process for drug distribution and the capacity for staff to return unused medications to inventory, there is potential for unused medications to be discarded. Medications that are only partially used, such as multidose products, may be given to patients for use at home after discharge or may be discarded in waste bins. Published literature on hospital-generated pharmaceutical waste in Canada is limited; however, a 353-bed hospital in Minnesota, United States, reported a total of 50 106 kg (110 233 lb) of pharmaceutical waste in 2007.18 Once collected, pharmaceutical waste must then be safely transported, sometimes long distances, to licensed incinerators for safe destruction, which further adds to the carbon footprint.
A handful of retrospective studies have addressed the financial burden of inpatient inhaler waste, but little is known about the associated environmental impacts.19–22 To our knowledge, our study is the first to quantify the environmental implications of wasted inhaler doses in the inpatient setting. A better understanding of the magnitude of waste could help inform steps toward the design of targeted interventions to minimize health care–related environmental impacts while preserving high-quality patient care.
A retrospective chart review was conducted for 3 months during the 2021/22 fiscal year in 3 acute care wards in Island Health, a health authority located in British Columbia and serving a population of more than 885 000 people.23 We included the only adult respiratory ward and 1 of the 2 general medical wards of a 500-bed tertiary hospital (Royal Jubilee Hospital) because they were most likely to have patients admitted for respiratory indications. We also included the adult medicine–surgery ward of a 48-bed community hospital (Saanich Peninsula Hospital), which is the only inpatient acute care ward in this facility.
The pharmacy informatics team generated a list of all inhalers dispensed to the specified wards. We did not include inhalers dispensed from wardstock due to limitations in the available software. Additionally, the community hospital site has a lock-and-key non-automated wardstock system, which operates only during pharmacy closure hours, meaning it is not possible to generate a wardstock report of which inhalers were dispensed to which patients.
Inpatients were selected for review if they had at least 1 inhaler dispensed from the hospital pharmacy during August 2021, January 2022, or March 2022. These months were chosen to capture 3 different seasons with differing degrees of inpatient respiratory admissions, to reduce seasonality bias: specifically, wildfire season with poor air quality (August), the typical period of winter respiratory illnesses (January), and allergy season (March).
All inhalers available on the hospital formulary during the study periods were included in the data collection. Most of the inhalers on formulary at the time of the study are listed in Table 1; some additional formulary inhalers were available but not dispensed during the study periods. Notably, the salbutamol MDI on formulary is the low-volume formulation, which emits 48.6 g CO2 eq per actuation.9 Patients meeting the study’s inclusion criteria were identified through a report generated by pharmacy informatics, and the associated paper charts were procured from medical records.
TABLE 1 Characteristics of Patients and Inhalers Dispensed

The Research Ethics & Compliance Office at Island Health deemed this project to be a quality improvement study, as per Article 2.5 of TCPS 2 (Tri-Council Policy Statement, which provides guidance on research with human participants),24 and thus exempt from institutional research ethics board review. All data were entered and stored in a password-protected REDCap (Research Electronic Data Capture, version 13.1.25) software tool. Each patient was assigned a numeric study identification number, and no identifying information such as name, personal health number, or medical record number was recorded in this software.
The primary objective was to determine the incidence of “wasted inhaler doses”, defined as doses that were dispensed from the hospital pharmacy during the 3 months of the study but never used. This outcome was calculated by subtracting the number of used actuations from the total number of actuations available and dividing this result by the total number of actuations available during the 3 months of the study. “Used actuations” were defined as actuations documented, in the paper medication administration record (MAR), as having been administered. The “total number of actuations available” was defined as the number of actuations per individual inhaler multiplied by the number of inhaler devices dispensed per participant during admission (e.g., 2 salbutamol inhalers with 200 actuations each dispensed to a single patient would correspond to a total of 400 salbutamol actuations available).
Although it is possible that some inhalers were sent home with patients (i.e., at the time of hospital discharge), Island Health does not currently have a policy in place to send patients home with multidose medication products dispensed in hospital; this practice is neither codified nor encouraged. Thus, any doses remaining in the inhaler at the time of discharge were considered wasted for the purposes of this study.
At the time of this study, every inhaler dispensed from the pharmacy, for distribution to both sites, was placed inside a plastic bag with a tamper seal set across the opening. These bags do not fit in the patient-specific medication drawers; therefore, the seal is immediately broken on arrival to the ward. Island Health does not reprocess or recirculate inhalers with broken tamper seals, which means that the number of inhalers with intact tamper seals that could be returned to inventory was negligible. There is also no predefined process for returning unused inhalers for recirculation. As a result, if no actuations were documented on a patient’s MAR, all doses were deemed to have been wasted.
The study had 4 secondary objectives:
One author (A.B.) performed data extraction from the paper charts. Data were captured from the patients’ MARs and chart notes, as well as best possible medication histories on admission (if available). Any discrepancies or ambiguities in the data were discussed between 2 authors (A.B., C.L.C.), agreed upon, and resolved. The data were analyzed using descriptive statistics.
During the 3 months of the study, 140 eligible patients had at least 1 inhaler dispensed from the hospital pharmacy. Following requests for paper charts, 8 patients were excluded from the study: 5 patient charts were stored off site and were not accessible in the available timeframe; 2 patients remained in hospital at the time of data collection, with paper charts unavailable through medical records; and 1 patient did not have dispensing of an inhaler documented on their MAR for the duration of their admission. Patient demographic characteristics and information about inhalers dispensed were recorded for all 132 patients (Table 1).
A total of 211 inhalers (totalling 23 031 actuations) were dispensed for the 132 patients. In total, 81.9% of all inhaler actuations dispensed were wasted. Depending on device type, up to 97.0% (range 40.0%–97.0%) of actuations per inhaler remained unused. These doses were wasted without contributing to patient care (Table 2).
TABLE 2 Wasted Actuations and Equivalent Greenhouse Gas Emissions over 3 Months
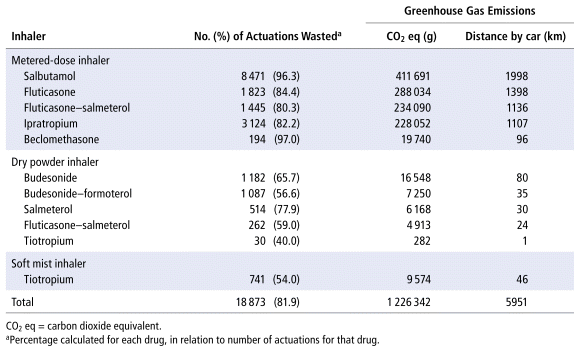
Our study showed that the wasted inhaler doses generated 1 226 342 g CO2 eq, equivalent to driving 5951 km in a typical Canadian gas-powered car,9 a distance greater than the drive from Victoria, British Columbia, to Halifax, Nova Scotia (Figure 1). This waste corresponded to a cost of $6172.82 over the 3 months of the study for the 3 adult wards.
|
| ||
|
FIGURE 1 Visual representation of 5951 km. Map data © 2025 Google, INEGI. | ||
We found that 16 patients (12.1%) had a duplicate inhaler dispensed, meaning an identical inhaler was dispensed from the pharmacy department within a timeframe where the original inhaler was not expected to be empty. Another 22 patients (16.7%) had at least 1 inhaler dispensed yet no doses documented on their MAR, meaning the inhalers were disposed of without contributing to patient care.
This multicentre retrospective chart review of 3 inpatient wards over 3 nonconsecutive months identified substantial environmental and financial waste. The magnitude of inhaler waste calculated here is similar to that reported previously—for example, 96.3% of dispensed salbutamol actuations wasted at our institutions, compared with 95% quoted in the existing literature21—which implies that unused multidose medication waste of this magnitude is prevalent across inpatient settings.
This paper adds to the existing body of literature on inhaler waste19–22 by detailing the magnitude of environmental impacts from unused doses for a total of 3 months within a single organization, the carbon footprint of which was equivalent to a driving 5951 km or slightly greater than the driving distance across the country, from coast to coast. If our results were extrapolated to all wards at both sites for the 2021/22 fiscal year (207 833 patient bed-days), the total cost of wasted doses would be $137 829.36, with GHG emissions of 27.4 t CO2 eq (equivalent to 132 921 km driven by a typical Canadian gas-powered car).
We also found that 12.1% of inhalers were dispensed in duplicate, meaning that 1 in 8 inhalers represented second units dispensed to the same patient before their first inhaler was finished, which suggests that inhaler loss or misplacement is contributing to the carbon footprint. A further 16.7% of inhalers dispensed had no corresponding doses documented in the patients’ MARs, meaning that 1 in 6 inhalers dispensed from pharmacy were disposed of in their entirety without contributing to patient care.
With regard to the carbon footprint, we found that MDIs represented 47.8% of inhalers dispensed in this study, yet they contributed 96.3% of the carbon footprint of wasted doses. This is likely due to their substantially greater carbon footprint and the greater number of actuations per device relative to other device types.
This study also highlights the impact of multidose medication product waste at the time of discharge. We found that the median length of stay was 10 days, which is in line with the Canadian average hospitalization of 7.2 days.26 Yet an inhaler can contain up to 3 months’ worth of actuations, meaning the majority of doses not used in hospital will be wasted because they cannot be reused for a different patient. At our centre, and many others across the country, there is currently no clear guidance on how to safely discharge patients home with their remaining multidose medication products due to concerns about outpatient labelling best practices and inhaler auto-substitutions in hospital, among others. These issues raise important questions about medication waste, affordability, and health equity, given the rising cost of prescription inhalers.
This study further highlights that inhaler waste and inhaler loss contribute disproportionately to the carbon footprint of hospital care and increasing health care costs, without contributing meaningfully to patient care. Devising strategies that target inhaler waste and inhaler loss is increasingly gaining traction nationally as a way to promote sustainable health care practices and improve patient outcomes.16 Some alternatives include using inhalers with fewer actuations per device, using MDIs with lower propellant volumes or lower carbon intensity propellants, considering nebules where clinically appropriate, encouraging the use of spacer devices to maximize medication delivery to the lung, and encouraging proper technique to maximize effectiveness and minimize waste. Other strategic approaches include supporting the safe reprocessing of used and unused inhalers (e.g., through “common cannister protocols”)27–30 and the development of policies and procedures that support discharging patients home with partially used multidose medication where appropriate. Such solutions need not be complicated; simply moving the location of the tamper seal at our institution has the potential to increase the pool of inhalers that can be returned to circulation.
Our study had several limitations. Only inhalers dispensed directly from the pharmacy were included in the analysis; no wardstock medications were captured. At our centres, both salbutamol and ipratropium MDIs are wardstock medications available in all 3 wards included in this study. Due to the frequent use of these devices, it is anticipated that a large number of inhalers (and therefore a large amount of waste) were not captured, which likely led to underestimation of the true financial and environmental burden. Conversely, our study might also have had a risk of overestimation of waste, because we assumed that any doses not administered were wasted. For instance, it is possible that unused inhalers with intact tamper seals were returned to pharmacy for reprocessing and were redispensed for other patients, although the current inhaler management processes at our centre (as outlined in the Methods section) make this unlikely. It is also possible that some partially used inhalers were sent home with patients when they were discharged. However, our health authority has no procedures supporting these practices, so we assumed that this did not occur and might thus have somewhat overestimated the amount of waste. We also did not consider the cost of pharmaceutical waste disposal or the environmental impact of transporting waste to a licensed incinerator, both of which would further augment our estimates of cost and carbon footprint. In some instances, the inhaler is left at the patient’s bedside, and documentation of self-administered doses may be unreliable.
To our knowledge, this is the first study assessing the environmental impact of wasted inhaler doses in the inpatient setting. It raises important questions about pharmaceutical waste, its environmental and financial impacts within the health authority, and differing inter-patient health equity. Given that more than 1 in 5 adults in Canada31 do not have insurance to cover the cost of outpatient medications, the health care system should seek to use opportunities to reduce waste and improve access to prescribed medications that have already been dispensed for an individual patient and would otherwise be wasted.
This retrospective chart review illustrated that wasted actuations, duplicate dispensing, and inhaler loss contribute disproportionately to rising health care costs and greenhouse gas emissions without benefiting patients. It raises important questions about pharmaceutical waste and health care sustainability, and offers insights into how minimizing waste can promote environmental stewardship while maintaining high-quality patient care.
1 Pörtner HO, Roberts DC, Tignor MMB, Poloczanska E, Mintenbeck K, Alegria A, et al. Climate change 2022: impacts, adaptation and vulnerability. Working Group II contribution to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change. Cambridge University Press; 2022 [cited 2023 Apr 24]. Available from: https://www.ipcc.ch/report/ar6/wg2/
2 Howard C, Buse C, Rose C, MacNeill A, Parkes M. The Lancet Countdown on health and climate change: policy brief for Canada. Canadian Medical Association and Canadian Public Health Association; 2019 Nov 2 [cited 2023 Aug 30]. Available from: https://policybase.cma.ca/viewer?file=%2Fmedia%2FPolicyPDF%2FPD20-06.pdf#page=1&search=&phrase=false
3 Sorensen CJ, Salas RN, Rublee C, Hill K, Bartlett ES, Charlton P, et al. Clinical implications of climate change on US emergency medicine: challenges and opportunities. Ann Emerg Med. 2020;76(2):168–78.
PubMed
4 Mehtsun WT, Hyland CJ, Offodile AC. Adopting a circular economy for surgical care to address supply chain shocks and climate change. JAMA Health Forum. 2023;4(11):e233497.
PubMed
5 Eckelman MJ, Sherman JD, MacNeill AJ. Life cycle environmental emissions and health damages from the Canadian healthcare system: an economic–environmental–epidemiological analysis. PLoS Med. 2018;15(7):e1002623.
PubMed PMC
6 Call for expressions of interest – Sustainability Task Force. Canadian Society of Hospital Pharmacists; 2023 Feb 7 [cited 2024 Aug 30]. Available from: https://www.cshp.ca/Site/Content/News/news-items/Call-Sustainability-TF.aspx?WebsiteKey=0c648ab0-50ba-4f43-9d77-13eecc1832e4
7 Park J, Miller F. Climate resilient, low carbon sustainable pharmacy playbook. A step-by-step guide for pharmacy professionals. Version 1.0. CASCADES (Creating a Sustainable Canadian Health System in a Climate Crisis) Canada; 2023 [cited 2023 Aug 30]. Available from: https://cascadescanada.ca/resources/climate-resilient-low-carbon-sustainable-pharmacy-playbook/
8 Tennison I, Roschnik S, Ashby B, Boyd R, Hamilton I, Oreszczyn T, et al. Health care’s response to climate change: a carbon footprint assessment of the NHS in England. Lancet Planet Health. 2021;5(2):e84–e92.
PubMed PMC
9 Stoynova V, Chang B. Detailed inhaler comparison chart (.xls) [spreadsheet]. CASCADES (Creating a Sustainable Canadian Health System in a Climate Crisis) Canada; [cited 2024 Jan 31]. Available from: https://view.publitas.com/5231e51e-4654-42c2-accd-b722e21f3093/detailed-inhaler-comparison-chart-preview/page/1
10 Jeswani HK, Azapagic A. Addendum to “Life cycle environmental impacts of inhalers” [J. Clean. Prod. 237 (2019) 117733]. J Clean Prod. 2023;389:135918.
11 Jeswani HK, Azapagic A. Life cycle environmental impacts of inhalers. J Clean Prod. 2019;237:117733.
12 Update to the BTS environment and lung health position statement – low carbon inhalers. British Thoracic Society; 2020 [cited 2023 Jan 16]. Available from: https://www.brit-thoracic.org.uk/news/2020/update-to-the-bts-environment-and-lung-health-position-statement-low-carbon-inhalers/
13 Gupta S, Couillard S, Digby G, Tse SM, Green S, Aceron R, et al. Canadian Thoracic Society position statement on climate change and choice of inhalers for patients with respiratory disease. Can J Respir Crit Care Sleep Med. 2023;7(5):232–9.
14 Asthma diagnosis, education and management [guideline]. Province of British Columbia, Ministry of Health; 2023 Jul 26 [cited 2024 Jan 31]. Available from: https://www2.gov.bc.ca/gov/content/health/practitioner-professional-resources/bc-guidelines/asthma
15 Green S, Bursque G, Chang B, Khan N, Miller FA, Wilson J, et al. Climate conscious inhaler prescribing in outpatient care playbook A step-by-step guide to more sustainable inhalers in primary care. Version 3.0. CASCADES (Creating a Sustainable Canadian Health System in a Climate Crisis) Canada; 2023 [cited 2024 Jan 31]. Available from: https://cascadescanada.ca/resources/sustainable-inhaler-prescribing-in-primary-care-playbook/
16 Stoynova V, Culley C. Climate conscious inhaler practices in inpatient care playbook. A step-by-step guide on sustainable inhalers in inpatient care. Version 1.0. CASCADES (Creating a Sustainable Canadian Health System in a Climate Crisis) Canada; 2023 [cited 2024 Jan 31]. Available from: https://cascadescanada.ca/resources/climate-conscious-inhaler-practices-in-inpatient-care-playbook/
17 Stoynova V, Culley C. Mitigating the climate impact of asthma therapy. University of British Columbia, Faculty of Medicine; 2022 Jun 28 [cited 2024 Jan 31]. Available from: https://thischangedmypractice.com/mitigating-the-climate-impact-of-asthma-therapy/
18 Burke MJ. Drug free: how North Memorial tackled its pharmaceutical waste problem. Health Facil Manage. 2008;21(10):67–68, 70.
PubMed
19 Aeng ESY, Dhaliwal MM, Tejani AM. A cautionary tale of multiple-dose drug products: fluticasone and salmeterol combination inhaler waste. J Eval Clin Pract. 2020;26(6):1699–702.
Crossref PubMed
20 Aeng ESY, McDougal KC, Allegretto-Smith EM, Tejani AM. Hidden costs of multiple-dose products: quantifying ipratropium inhaler wastage in the hospital setting. Can J Hosp Pharm. 2021;74(2):117–21.
Crossref PubMed PMC
21 Sakaan S, Ulrich D, Luo J, Finch CK, Self TH. Inhaler use in hospitalized patients with chronic obstructive pulmonary disease or asthma: assessment of wasted doses. Hosp Pharm. 2015;50(5):386–90.
Crossref PubMed PMC
22 Drummond I, Aeng ESY, Yeh P, Chen C, Tejani AM. Hiding in plain sight: quantifying salbutamol and ipratropium inhaler wastage in hospitals. Can J Hosp Pharm. 2023;76(4):314–6.
PubMed PMC
23 About us [website]. Island Health; [cited 2023 Aug 30]. Available from: https://www.islandhealth.ca/about-us
24 Chapter 2: Scope and approach. In: Tri-Council policy statement: ethical conduct for research involving humans – TCPS 2 (2022). Government of Canada, Panel on Research Ethics; 2022 [cited 2023 Aug 30]. Available from: https://ethics.gc.ca/eng/policy-politique_tcps2-eptc2_2022.html
25 Leduc ER. Medi-Mouse: a powerful little site for busy doctors [drug search tool]. Self-published; [cited 2024 Jan 31]. Available from: https://medi-mouse.com/drugfind.php
26 Hospital stays in Canada – series. Canadian Institute for Health Information; [cited 2023 Apr 25]. Available from: https://www.cihi.ca/en/hospital-stays-in-canada
27 Larson T, Gudavalli R, Prater D, Sutton S. Critical analysis of common canister programs: a review of cross-functional considerations and health system economics. Curr Med Res Opin. 2015;31(4):853–60.
PubMed
28 Grissinger M. Shared metered dose inhalers among multiple patients: can cross-contamination be avoided? P T. 2013;38(8):434–42.
PubMed PMC
29 Neel S, Tauman A. Can successful implementation of the common canister program deliver cost containment and improved infection control? Hosp Pharm. 2012;47(9):700–11.
30 Elbeddini A. Sterilization plan of the used metered dose inhalers (MDI) to avoid wastage amid COVID-19 pandemic drug shortage. J Pharm Policy Pract. 2020;13:19.
PubMed PMC
31 Cortes K, Smith L. Pharmaceutical access and use during the pandemic. Statistics Canada; 2022 [cited 2024 Mar 5]. Available from: https://www150.statcan.gc.ca/n1/en/catalogue/75-006-X202200100011
Address correspondence to: Dr Alison Bentley, Port McNeill Hospital, 2750 Kingcome Place, Port McNeill BC V0N 2R0, email: Alison.Bentley@islandhealth.ca
Competing interests: For activities not directly related to the study reported here, Celia Culley has received grants from the South Island Facilities Engagement Initiative and CASCADES Canada; honoraria from the BC Branch of the Canadian Society of Hospital Pharmacists (now the Canadian Society of Healthcare-Systems Pharmacy [CSHP]) and the Therapeutics Initiative; and travel funding from CSHP, the BC Branch of CSHP, and Island Health; and has served in a leadership role with the Canadian Association of Pharmacy for the Environment and the CSHP. For activities not directly related to the study reported here, Valeria Stoynova has received grants from CASCADES Canada, the South Island Facilities Engagement Initiative, and The Ottawa Hospital Academic Medical Organization; speaking honoraria from Health Quality BC, the CSHP, the Canadian Society of Internal Medicine (CSIM), the Vancouver Physicians Society, and the Victoria Division of Cardiology; and travel funding from CSHP and CSIM; and has been a member of advisory boards for the BC Guidelines and Protocols Advisory Committee and CASCADES Canada. No other competing interests were declared.
Funding: None received.
Acknowledgments: The authors would like to acknowledge Kyle McWilliams and Nadia McTaggart for their contributions to this project, including editorial, operational, and clinical knowledge.
Submitted: March 5, 2024
Accepted: November 11, 2024
Published: April 9, 2025
© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 2, 2025