Joycelyn Lac, Carmen Leung, Karen Yan, Anita I Kapanen, and Tiana TilliTo cite: Lac J, Leung C, Yan K, Kapanen AI, Tilli T. Expanding opioid stewardship: collaboration between hospital and primary care pharmacists. Can J Hosp Pharm. 2025;78(2):e3664. doi: 10.4212/cjhp.3664
Between April 2015 and March 2016, one-third of hospital visits for opioid toxicity in British Columbia were for patients with an active opioid prescription at the time of overdose.1 To help reduce opioid-related harms while increasing effective pain management, pharmacist-led opioid stewardship programs have been developed.2 Pharmacist interventions within these programs include therapy adjustments, medication reviews, and academic detailing.3 In hospital and primary care settings, opioid stewardship interventions by pharmacists have led to reductions in both mean daily opioid doses and adverse events, as well as improvements in pain control and quality of life.4–8 Patients and prescribers have reported high rates of appreciation and satisfaction with these interventions.9,10
Although opioid stewardship interventions within individual care settings have been effective, patient journeys span multiple care settings. A growing number of patients within the Canadian health care system are being cared for by primary care teams that include pharmacists.11,12 Collaboration between hospital and primary care pharmacists could provide ongoing opioid stewardship support through transitions of care, a period associated with increases in adverse events and medication errors.13,14 The literature has shown that intraprofessional collaboration between hospital and community pharmacists, as well as pharmacist-led transitions of care, can reduce hospital readmission rates across various conditions.15,16 Furthermore, analgesic titrations take time to complete, often extending beyond a patient’s hospital stay.17 Primary care pharmacists could support completion of hospital-initiated interventions.
This study piloted an intraprofessional opioid stewardship collaboration between hospital and primary care pharmacists for patients who had pain and/or were taking opioids and who transitioned across care settings.
A hospital opioid stewardship program was first established at Royal Columbian Hospital in New Westminster, British Columbia (2018), followed by programs at Surrey Memorial Hospital in Surrey (2019) and St. Paul’s Hospital in Vancouver (2020).2,10,18 An intraprofessional collaboration, as described in this article, was subsequently established in 2021, involving 4 opioid stewardship pharmacists across these tertiary care hospitals and 5 pharmacists at a primary care clinic at the University of British Columbia’s Faculty of Pharmaceutical Sciences. This clinic provides comprehensive medication management through an appointment-based model.
Hospitalized patients were identified for opioid stewardship consultations through referrals from the health care team and/or computer-generated reports identifying patients with high-risk opioid orders (where “high risk” was defined in relation to either the patient or the prescription), based on site-specific protocols.2 Patients were triaged according to the number of high-risk opioid orders and a review of the electronic health record to identify those who might benefit from a full clinical assessment by an opioid stewardship pharmacist.2 Patients followed by acute or complex pain services, palliative care teams, or the addictions medicine service (because of an opioid use disorder) were ineligible.2 At one of the sites, patients admitted to critical care units were also ineligible.2
Patients seen by an opioid stewardship pharmacist during the hospital stay were eligible for referral to the primary care clinic at discharge if they were 18 years or older, were taking one or more opioids or were experiencing pain, had a community prescriber, and provided consent for the referral.
A retrospective chart review was undertaken for patients referred to the primary care clinic between November 1, 2021, and April 19, 2023. Patients seen at the clinic were identified through a query of its electronic medical records system (OSCAR-EMR). Deidentified data were collected from the date of the patient’s initial appointment at the clinic (baseline) until the end of 3 months of follow-up or the end of the overall study period, whichever came first. The study protocol was approved by the University of British Columbia Clinical Research Ethics Board (#H23-01255), which waived the need for informed consent for data collection, and the study was conducted in accordance with ethics principles set forth by the Helsinki Declaration.
The opioid stewardship pharmacists reviewed health records, consulted with patients and health care teams, performed clinical assessments, and developed pain management recommendations. Before hospital discharge, they discussed a referral to the clinic with eligible patients, who received a handout (Appendix 1A) explaining the collaboration. For those who consented, a referral form (Appendix 1B), one or more opioid stewardship consult notes, and the hospital discharge summary were faxed to the primary care clinic. The opioid stewardship pharmacists and clinic pharmacists connected by phone if further case discussion was needed. Clinic staff contacted patients to schedule an initial 60-minute appointment, held in person or virtually, and 30- to 60-minute follow-up appointments as required. Clinic pharmacists assessed continuation of pain care plans and made recommendations to prescribers. Opioid stewardship pharmacists were copied on consult notes from initial appointments, for purposes of continuity, given that clinic pharmacists could not upload their notes to the provincial electronic health system. Pain medication recommendations made by the opioid stewardship pharmacists and the clinic pharmacists were patient-specific and aligned with Canadian guidelines for opioid use in chronic noncancer pain,19 as well as, when available, local or international practice standards for management of various pain syndromes. Initially, a single opioid stewardship pharmacist sent referrals to 1 of 2 designated clinic pharmacists (T.T.). As the program expanded, the opioid stewardship pharmacists, the 2 designated clinic pharmacists, and the clinic medical office assistant met every 1–2 months to discuss the appropriateness of referrals, to address logistics, to develop operational supports (Appendix 1), and to plan expansion of the referral process to all opioid stewardship and clinic pharmacists. After 6 months, all pharmacists in both settings were involved in patient referrals through this collaboration.
The outcomes of interest were patient characteristics, the status of hospital-initiated pain management care plans at the time of each patient’s initial clinic appointment, and pain management–related drug therapy problems identified and subsequent recommendations made by primary care pharmacists to address them.
Two pharmacy student research assistants extracted the data, including primary care pharmacist notes and relevant documents, from patients’ charts (e.g., opioid stewardship faxes, medication lists from PharmaNet [the provincial data system]). Daily opioid use was charted on the basis of patient reports during appointments. Qualitative variables were reported as percentages and quantitative variables as means with standard deviations. Microsoft Excel spreadsheet software (version 16.82) was used for the analyses.
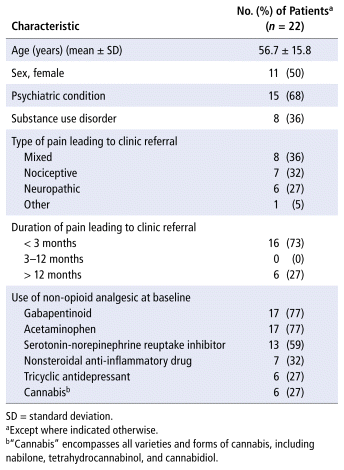
Forty-two patients were referred to the primary care clinic as part of the opioid stewardship collaboration during the study period, of whom 22 were included in this analysis (Table 1). The others declined the service when called to schedule their initial clinic appointment (n = 9), were unable to be reached by the clinic (n = 8), were seen outside the study period (n < 5), or were rehospitalized before they could be seen at the clinic (n < 5). The average time from the date of referral to the first clinic appointment was 16.7 days, with an average of 2.9 appointments per patient over 3 months. The top reasons for referral were opioid tapering (n = 19, 86%), optimization of non-opioid analgesic (n = 10, 45%), and medication review (n = 6, 27%).
TABLE 1 Baseline Characteristics of Patients Seen by Opioid Stewardship Pharmacist in Hospital, then Referred to and Seen by Pharmacist at Primary Care Clinic

The mean total daily dose of opioids was 49.4 mg morphine equivalent at baseline and 41.6 mg morphine equivalent at follow-up. Seventeen patients (77%) were taking opioids (including over-the-counter codeine) at their initial clinic appointment, whereas 12 (55%) patients were known to be doing so by the 3-month follow-up. The 5 patients who discontinued opioid therapy had all been referred for acute pain (i.e., lasting less than 3 months).
Opioid stewardship pharmacists made a total of 122 medication recommendations (mean 5.5 per patient, standard deviation [SD] 2.1), as recorded in their pain management consult notes. The mean proportion of recommendations implemented per patient at the initial clinic appointment was 74%. Of the 34 recommendations not in place at the initial clinic appointment, reasons included persistent pain (n = 9, 26%), patient preference (n = 6, 18%), lack of patient understanding (n = 4, 12%), supply issues (n = 4, 12%), cost barriers (n = 3, 9%), and adverse effects (n = 2, 6%). For the remaining 18% (n = 6) of recommendations not implemented at the initial appointment, the reason was unknown because of unclear documentation regarding whether or not the recommendation had been implemented (or implemented and then discontinued by the time of the initial clinic appointment).
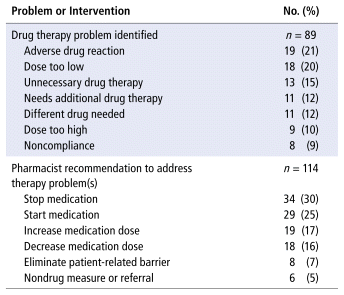
Clinic pharmacists addressed a total of 89 drug therapy problems with 114 recommendations across all patients within their first 3 months of appointments (Table 2). Multiple recommendations may have constituted the plan to address a single drug therapy problem (mean 1.3 recommendations per plan, SD 1.7). For the 62 drug therapy problems with known outcomes, plans were implemented for 43 (69%); for the remaining 19 problems with known outcomes, the plans were not implemented for patient-related reasons (n = 14, 23%) or prescriber-related reasons (n = 5, 8%).
TABLE 2 Drug Therapy Problems Identified and Recommendations Made by Primary Care Pharmacists for Patients Referred by Opioid Stewardship Pharmacists Practising in Hospital
An opioid stewardship collaboration between hospital and primary care pharmacists was successfully piloted. This project helped to promote communication by establishing 2-way access to consult notes and facilitating case discussions by telephone. Addressing logistical challenges during collaboration team meetings led to the development of operational supports, including a patient information handout (Appendix 1A). This handout explained the collaboration, with the aim of promoting informed decision-making by the patient during referrals and serving as a reference once the patient was home. A collaboration-specific notice of appointment was also developed, to inform community prescribers about the clinic’s services and to clarify role expectations, especially with regard to prescribing pain medications (Appendix 1C). Overall, the findings from this evaluation suggest that intraprofessional pharmacist collaboration can improve the implementation and continuity of pain care plans.
More specifically, this retrospective evaluation showed that collaboration between hospital and primary care pharmacists led to refinement of hospital-initiated pain care plans according to patients’ changing needs as they transitioned home. Although the opioid stewardship pharmacists individualized their recommendations, pain care plans were often not fully in place at the time of initial primary care appointments. Reasons included persistent pain, patient-related factors (e.g., preferences, understanding), and medication access issues (e.g., supply challenges, cost barriers) in the home environment. Persistent pain may arise from changing pain needs after discharge, as analgesic requirements may increase as other supports are reduced.20 Additionally, it may be necessary to reduce tapering rates as the total daily opioid dose is decreased.17 Furthermore, opioid-sparing analgesics often require weeks of titration to achieve therapeutic doses and thus may be found to be ineffective or intolerable when assessed at follow-up. The primary care pharmacists’ recommendations completed the hospital pharmacists’ pain care plans by promoting patient-specific refinements over time (Table 2).
These findings support calls for pharmacist-led transitions-of-care services in primary care.16,21 Similar pain management collaborations could focus on individuals with acute pain, given that the primary care pharmacists in this pilot successfully supported opioid discontinuation in this population. Collaborations of this type present an opportunity to prevent long-term opioid use, given that the risk increases with each day that opioids are supplied to opioid-naive adults.22 Future collaborations might also benefit from including community pharmacists in the intraprofessional pain management team.
The strengths of this study included the participation of all pharmacists within the opioid stewardship program and at the primary care clinic, which enhanced generalizability. The limitations included the small sample size, the unknown rate of patient consent for initial referrals, and the high proportion of patients who consented but did not attend their initial appointment. The last of these limitations aligns with findings reported by Heaton and others,15 who noted that less than 30% of patients attended their pharmacist appointments after discharge. Additional limitations included the high numbers of unknown outcomes for recommendations made by hospital and primary care pharmacists. Future evaluations could benefit from prospective methodology with standardized documentation in primary care clinics to record the outcomes of interest and to ensure complete follow-up periods for all participants.
Opioid stewardship interventions should be expanded beyond individual care settings to include intraprofessional collaborations between hospital and primary care pharmacists.
1 Gomes T, Khuu W, Craiovan D, Martins D, Hunt J, Lee K, et al. Comparing the contribution of prescribed opioids to opioid-related hospitalizations across Canada: a multi-jurisdictional cross-sectional study. Drug Alcohol Depend. 2018;191:86–90.
PubMed
2 St. Paul’s Hospital opioid stewardship program: 2 year program report January – December 2021. British Columbia Centre on Substance Use and Providence Health Care; 2022 Jul [cited 2024 Feb 21]. Available from: https://www.bccsu.ca/wp-content/uploads/2022/08/OSP-Y2-Report-Jul-2022.pdf
3 Gondora N, Versteeg SG, Carter C, Bishop LD, Sproule B, Turcotte D, et al. The role of pharmacists in opioid stewardship: a scoping review. Res Social Adm Pharm. 2022;18(5):271447.
4 Bhimiji H, Landry E, Jorgenson D. Impact of pharmacist-led medication assessments on opioid utilization. Can Pharm J (Ott). 2020;153(3): 148–52.
5 Tilli T, Hunchuck J, Dewhurts N, Kiran T. Opioid stewardship: implementing a proactive, pharmacist-led intervention for patients coprescribed opioids and benzodiazepines at an urban academic primary care centre. BMJ Open Qual. 2020;9(2):e000635.
PubMed PMC
6 Perry K, Ferron S, Norquist N, Mullen DM. A pharmacist-assisted initiative to improve chronic pain management and reduce opioid use in primary care. Innov Pharm. 2023;14(1):10.24926/iip.v14i1.5265.
PubMed PMC
7 Dole EJ, Murawski MM, Adolphe AB, Aragon FD, Hochstadt B. Provision of pain management by a pharmacist with prescribing authority. Am J Health Syst Pharm. 2007;64(1):85–90.
8 Chen J, Lu X, Wang W, Shen B, Ye Y, Jiang H, et al. Impact of a clinical pharmacist-led guidance team on cancer pain therapy in China: a prospective multicenter cohort study. J Pain Symptom Manag. 2014;48(4): 500–9.
9 Coulson EE, Kral LA. The clinical pharmacist’s role in perioperative surgical pain management. J Pain Palliat Care Pharmacother. 2020;34(3): 120–6.
PubMed
10 Ramasubbu C, Chernushkin K, Ng K, Legal M. Discerning clinician perceptions of an established opioid stewardship (DISCLOSE) program. Can J Hosp Pharm. 2023;76(1):63–70.
PubMed PMC
11 Rudoler D, Peckham A, Grudniewicz A, Marchildon G. Coordinating primary care services: a case of policy layering. Health Policy. 2019;123(2):215–21.
12 Transforming our primary care system through primary care networks. British Columbia Ministry of Health; 2019 Dec [cited 2024 Feb 23] Available from: https://www2.gov.bc.ca/assets/gov/health/about-bc-s-health-care-system/heath-care-partners/health-newsletter/context-pcn-december-2019.pdf
13 Thurston MM, Dupree LH, Shogbon Nwaesei A, Newsom LC. Incorporation of innovative strategies for patient education in pharmacist-led transition of care initiatives. Ann Pharmacother. 2024;58(6):657–60.
14 Kurteva S, Habib B, Moraga T, Tamblyn R. Incidence and variables associated with inconsistencies in opioid prescribing at hospital discharge and its associated adverse drug outcomes. Value Health. 2021; 24(2):147–57.
PubMed
15 Heaton PC, Frede S, Kordahi A, Lowery L, Moorhead B, Kirby J, et al. Improving care transitions through medication therapy management: a community partnership to reduce readmissions in multiple health-systems. J Am Pharm Assoc. 2019;59(3):319–28.
16 Slazak E, Cardinal C, Will S, Clark CM, Daly CJ, Jacobs DM. Pharmacist-led transitions-of-care services in primary care settings: opportunities, experiences, and challenges. J Am Pharm Assoc. (2003). 2020;60(3):443–9.
17 Wang Y, Wilson DL, Fernandes D, Adkins LE, Bantad A, Copacia C, et al. Deprescribing strategies for opioids and benzodiazepines with emphasis on concurrent use: a scoping review. J Clin Med. 2023;12(5):1788.
PubMed PMC
18 St. Paul’s Hospital opioid stewardship program: 6 month program report January – June 2020. British Columbia Centre on Substance Use and Providence Health Care; 2020 Oct [cited 2024 Oct 16]. Available from: https://www.bccsu.ca/wp-content/uploads/2020/10/OpioidStewardshipProgram-Final.pdf
19 Busse JW, Craigie S, Juurlink DN, Buckley DN, Wang L, Couban RJ, et al. Guideline for opioid therapy and chronic noncancer pain. CMAJ. 2017;189(18):E659–66.
PubMed PMC
20 Meints SM, Edwards RR. Evaluating psychosocial contributions to chronic pain outcomes. Prog Neuropsychopharmacol Biol Psychiatry. 2018;87(Pt B):168–82.
PubMed PMC
21 Ensing HT, Koster ES, Stuijt CCM, van Dooren AA, Bouvy ML. Bridging the gap between hospital and primary care: the pharmacist home visit. Int J Clin Pharm. 2015;37(3):4304.
Crossref
22 Shah A, Hayes CJ, Martin BC. Characteristics of initial prescription episodes and likelihood of long-term opioid use - United States, 2006–2015. MMWR Morb Mortal Wkly Rep. 2017;66(10):265–9.
Crossref PubMed PMC
Address correspondence to: Dr Tiana Tilli, Faculty of Pharmaceutical Sciences, University of British Columbia, 2301–2405 Wesbrook Mall, Vancouver BC V6T 1Z3, email: tiana.tilli@ubc.ca
Competing interests: None declared.
Funding: None received.
Acknowledgements: The authors thank the opioid stewardship hospital pharmacists for their collaboration, the primary care pharmacists for providing patient care during postdischarge appointments, and the medical office assistants in the various primary care clinics for their administrative support. We also recognize Isabella Durante who provided assistance with manuscript referencing.
Submitted: June 11, 2024
Accepted: November 11, 2024
Published: April 9, 2025



© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 2, 2025