Tanya Dhanoa, Rosaleen Boswell, and Arden R BarryTo cite: Dhanoa T, Boswell R, Barry AR. Patients’ beliefs about their heart failure medications: a cross-sectional survey. Can J Hosp Pharm. 2025;78(3):e3692. doi: 10.4212/cjhp.3692
ABSTRACT
Background
The Beliefs about Medicines Questionnaire (BMQ) is a validated tool that has been correlated with medication adherence.
Objectives
To determine patients’ beliefs about their heart failure (HF) medications and their self-reported adherence.
Methods
In this prospective cross-sectional survey of community-dwelling adult patients with any type of HF, beliefs were assessed using the BMQ. Self-reported adherence was assessed using the 5-item Medication Adherence Report Scale (MARS-5). Data were collected between January and May 2024. The primary outcome was the BMQ necessity–concerns differential (NCD).
Results
Thirty-five patients completed the survey. The mean age was 63.9 years, and 22 (63%) of the patients were women. Thirteen patients (37%) self-reported having HF with reduced ejection fraction. The mean NCD was 7.8 (range −20 to +20). The mean BMQ subscale scores were as follows: general-harm, 8.8 out of 25; general-overuse, 8.1 out of 15; specific-necessity, 20.7 out of 25; and specific-concerns, 12.9 out of 25. The mean MARS-5 score was 22.3 out of 25.
Conclusions
The positive value for mean NCD indicated that patients’ beliefs about the necessity of their HF medications exceeded their concerns. Self-reported adherence was high.
KEYWORDS: heart failure, drug therapy, medication adherence
RÉSUMÉ
Contexte
Le Beliefs about Medicines Questionnaire (BMQ) [questionnaire sur les croyances à propos des médicaments] est un outil validé corrélé à l’observance thérapeutique.
Objectifs
Déterminer les croyances des patients au sujet de leurs médicaments pour l’insuffisance cardiaque (IC) et l’observance signalée par le patient.
Méthodologie
Dans cette étude transversale prospective menée auprès de patients adultes vivant à domicile et souffrant de tout type d’IC, l’évaluation des croyances s’est faite à l’aide du BMQ. L’observance signalée par le patient a été évaluée à l’aide de la Medication Adherence Report Scale (MARS-5) [l’échelle à 5 points de rapport d’observance thérapeutique]. Les données ont été recueillies entre janvier et mai 2024. Le résultat principal de l’étude était le différentiel nécessité-préoccupation (DNP) du BMQ.
Résultats
Trente-cinq patients ont répondu au sondage. L’âge moyen était de 63,9 ans, et 22 personnes (63 %) étaient des femmes. Treize patients (37 %) ont déclaré avoir une IC avec fraction d’éjection réduite. Le score moyen du DNP était de 7,8 (plage de −20 à +20). Les scores moyens des sous-échelles du BMQ étaient les suivants : dangerosité-générale : 8,8 sur 25; surutilisation générale : 8,1 sur 15; nécessité spécifique : 20,7 sur 25; et préoccupations spécifiques : 12,9 sur 25. Le score moyen de l’échelle MARS-5 était de 22,3 sur 25.
Conclusions
La valeur positive du DNP moyen indique que les croyances des patients concernant la nécessité de prendre leurs médicaments pour l’IC dépassaient leurs préoccupations. L’observance signalée par le patient était élevée.
Mots-clés: insuffisance cardiaque, thérapie médicamenteuse, observance thérapeutique
Heart failure (HF) is a prevalent chronic medical condition that affects more than 60 million people worldwide and is associated with a 1-year mortality rate of 15%–30%.1 Acute exacerbations of HF are the leading cause of hospitalization in North America among patients older than 65 years of age, and the prevalence has increased in recent years.1,2 Guideline-directed medical therapy for patients with HF, irrespective of left ventricular ejection fraction, has been demonstrated to improve mortality and morbidity, as well as quality of life.3–6 Adherence to these therapies can be influenced by various factors, including patients’ beliefs and perceptions about their medications.7–9 The Beliefs about Medicines Questionnaire (BMQ) is a validated instrument that is used to assess patients’ beliefs surrounding their medications, which has been associated with adherence.10–12 The objectives of this study were to evaluate the beliefs of community-dwelling HF patients about their medications, to determine patients’ self-reported adherence, and to identify factors associated with more or less favourable beliefs.
This cross-sectional study was based on a 23-question online survey that incorporated the BMQ and the 5-item Medication Adherence Report Scale (MARS-5). The survey was created with the University of British Columbia Survey Tool, provided by Qualtrics. The study was approved by the University of British Columbia Behavioural Research Ethics Board (H23-02405).
Adults 18 years of age or older with a diagnosis of any type of HF (reduced, mildly reduced, or preserved ejection fraction) and currently taking 1 or more medications for HF were included. There were no specific exclusion criteria. Recruitment occurred at selected specialized outpatient HF clinics in British Columbia and Alberta. These clinics provided patients with information about the study, and a QR code was also available on posters and pamphlets. Additional online recruitment occurred through REACH BC, a nonprofit platform that connects volunteers with research opportunities, and through social media posts on the Facebook and X platforms. Survey responses with 30% or more questions left unanswered, suspicious response patterns, or exact duplicates were excluded from analysis.
The BMQ consists of 4 subscales: general-harm, general-overuse, specific-concern, and specific-necessity.10,11 Each subscale consists of 3 or 5 questions, and each question is answered using a 5-point Likert scale (ranging from 1 = strongly disagree to 5 = strongly agree). Total possible scores in each subscale range from 5 to 25, with the exception of the BMQ general-overuse subscale (for which the possible score ranges from 3 to 15). Higher values indicate stronger opinions regarding harm, overuse, concern, and necessity. The questions for specific-concern and specific-necessity subscales were modified to be specific to HF medications. The MARS-5 questionnaire asks participants 5 questions about their self-reported medication adherence, to be answered using a 5-point unipolar scale (ranging from 1 = always to 5 = never), with the total possible score ranging from 5 to 25.12 By convention, nonadherence was defined as any score below 23, which was the definition used in a previous study of patients with HF.13 In addition to the BMQ and MARS-5 scores, the following demographic data were collected: gender, education, employment status, type of HF, classification of HF symptoms, length of HF diagnosis, cardiovascular comorbidities, and HF medications. Participants were asked to voluntarily self-report ethnic origin and/or race based on the Canadian Ethnic or Cultural Origin Reference Guide14 and current guidelines.15
The primary outcome was the mean BMQ necessity–concern differential (NCD), where each patient’s NCD was calculated as the specific-concern score subtracted from the specific-necessity score. Secondary outcomes were mean BMQ subscale scores, mean MARS-5 score, and patient factors associated with a higher or lower mean NCD.
Descriptive statistics were used to report participant baseline characteristics and mean BMQ and MARS-5 scores. Linear regression was used to identify participant characteristics associated with mean NCD score using the following covariates: gender, ethnic origin/race, education, employment status, type of HF, length of HF, and HF symptom classification. The association between adherence and specific-necessity score was assessed using a Mann–Whitney U test. Analyses were performed with IBM SPSS Statistics, version 29 (IBM Corporation) and GraphPad Prism, version 10.0.0 (GraphPad Software Inc).
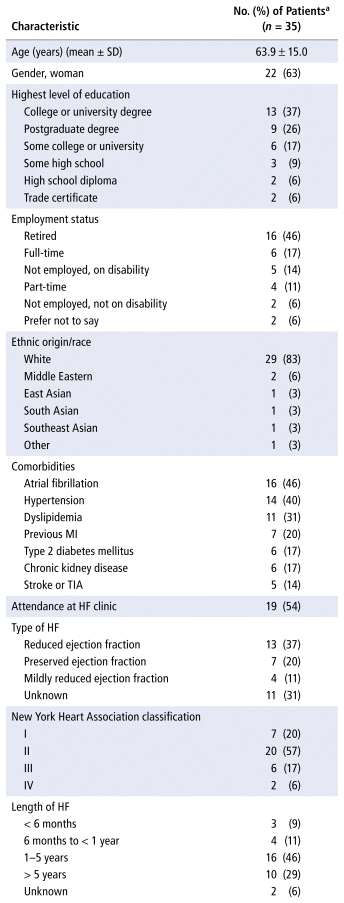
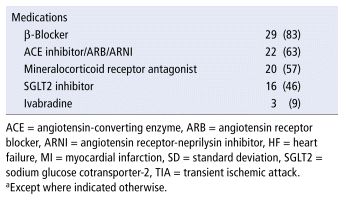
The survey was open from January to May 2024. Sixty patients initiated the survey, and 35 completed it in full. Participants’ mean age was 63.9 years, 63% of the participants were female, 83% were White, 37% had a college or university degree, and 46% were retired (Table 1). More than a third (37%) self-reported having HF with reduced ejection fraction, and 57% self-reported New York Heart Association class II symptoms. Self-reported medication use included β-blocker (83%), renin–angiotensin–aldosterone system inhibitor (63%), mineralocorticoid receptor antagonist (57%), and sodium glucose cotransporter-2 inhibitor (46%).
TABLE 1 Baseline Characteristics


The mean NCD score was 7.8 (range −20 to 20) (Figure 1). The mean BMQ subscale scores were as follows: general-harm, 8.8 out of 25; general-overuse, 8.1 out of 15; specific-necessity, 20.7 out of 25; and specific-concerns, 12.9 out of 25. For the specific-necessity subscale, 86% of the patients (n = 30) agreed or strongly agreed that “my health depends on my heart medicines.” For the specific-concern subscale, 57% of respondents (n = 20) agreed or strongly agreed with the statement, “I sometimes worry about the long-term effects of my heart medicines.” The mean MARS-5 score was 22.3 out of 25, which indicates that most patients were adherent with their therapy, with 69% of respondents (n = 24) having a score of 23 or above. Adherence was associated with a higher specific-necessity score than was nonadherence (20.8 vs 11.9, p = 0.015).
|
| ||
|
FIGURE 1 Mean response scores on the Beliefs about Medicines Questionnaire (BMQ) and its subscales and the 5-item Medication Adherence Report Scale (MARS-5). NCD = necessity–concerns differential. | ||
Postgraduate education was associated with a lower mean NCD than was high school education (p = 0.048). Retirement was associated with a higher mean NCD than full-time employment (p = 0.005), as was longer relative to shorter HF duration (> 5 years or 1–5 years vs < 6 months) (p = 0.006 and p = 0.024, respectively).
Respondents to this cross-sectional survey generally held strong necessity-type beliefs toward their long-term HF medications, with high average self-reported adherence, despite moderate concern-type beliefs. The mean NCD of approximately 8 indicates that participants’ perceptions about the necessity of their HF medications exceeded their concerns about potential adverse effects or drawbacks. This finding suggests a complex cognitive appraisal process whereby individuals acknowledge the importance of their medication regimen while simultaneously harbouring reservations about potential negative consequences.16 Participants demonstrated strong beliefs about the necessity of their medications, as evidenced by the high specific-necessity score of approximately 21.
In a previous study, Percival and others13 used the BMQ and MARS-5 to evaluate beliefs about HF medications among 43 patients in Australia. Of those patients, 86% were considered to be adherent, whereas only 69% of patients in the current study were deemed to be adherent (MARS-5 score ≥ 23). The study by Percival and others13 demonstrated that participants’ higher necessity-type beliefs toward their pharmacotherapy were associated with being adherent rather than nonadherent, as we observed in the present study. However, Percival and others13 did not report demographic data relating to ethnic origin/race, income, or education; furthermore, region-specific culture and beliefs may differ from those of our Canadian population.
We planned to perform linear regression to assess whether beliefs about HF medications varied with ethnic origin/race. Previous literature has shown that race can influence the allocation of HF therapy.17 Barry and others18 conducted a similar study of patients’ beliefs about their preventive pharmacotherapy after an acute coronary syndrome, and found that patients of South Asian and Middle Eastern ethnic origins exhibited a significantly higher mean NCD relative to those of European origin. However, in the current study, we were unable to examine the relationship between ethnic origin/race and beliefs about HF medications due to the limited sample of non-White respondents (n = 6).
The social determinants of health can greatly influence health outcomes, particularly in patients with chronic diseases such as HF.19,20 These determinants include income, social status, education and literacy, childhood experiences, social supports, gender, and ethnicity/race. It is essential that health care providers recognize the complexity of how the social determinants of health may influence patients’ perceptions about the importance of their medications relative to other basic needs. In the current study, mean NCD was higher among patients who were retired than among those with full-time employment, while—somewhat paradoxically—mean NCD was lower among patients with postgraduate education than among those who had only completed high school. Also, mean NCD was higher among patients with longer duration of HF, which suggests that those with increased experience of HF may have stronger beliefs about the necessity of their HF medications, possibly due to improved symptomatology or function. The higher mean NCD among retired patients may simply reflect a longer duration of HF.
This study had limitations that merit discussion. The low response rate may have introduced selection bias. Also, a high number of patients initiated but did not complete the survey, possibly due to a language barrier or the length of the survey. Most of the patients were White, which may limit the generalizability of the results. Sampling bias may have occurred, as the survey required English language comprehension, digital literacy, and access to an internet-connected device, all of which may have selected for more educated, predominantly English-speaking participants. Finally, there was a potential responder bias, in that patients who were more engaged with their health (and thus may hold more favourable beliefs about their medications or be more adherent) may have been more likely to respond to the survey.
This survey demonstrated that community-dwelling patients with HF generally held strong necessity-type beliefs about their HF medications, despite having moderate concerns about long-term use of these drugs. These findings corresponded to a positive NCD and high self-reported adherence. Some disparities in NCD were related to patients’ employment, education, and duration of HF. Together, these findings underscore the multifaceted nature of medication beliefs and adherence behaviours, highlighting the need for individualized HF medication management strategies to enhance patient outcomes.
1 Savarese G, Becher PM, Lund LH, Seferovic P, Rosano GMC, Coats AJS. Global burden of heart failure: a comprehensive and updated review of epidemiology. Cardiovasc Res. 2023;118(17):3272–87.
Crossref
2 Agarwal MA, Fonarow GC, Ziaeian B. National trends in heart failure hospitalizations and readmissions from 2010 to 2017. JAMA Cardiol. 2021;6(8):952–6.
Crossref PubMed PMC
3 Ezekowitz JA, O’Meara E, McDonald MA, Abrams H, Chan M, Ducharme A, et al. 2017 comprehensive update of the Canadian Cardiovascular Society guidelines for the management of heart failure. Can J Cardiol. 2017;33(11):1342–433.
PubMed
4 McDonald M, Virani S, Chan M, Ducharme A, Ezekowitz JA, Giannetti N, et al. CCS/CHFS heart failure guidelines update: defining a new pharmacologic standard of care for heart failure with reduced ejection fraction. Can J Cardiol. 2021;37(4):531–46.
PubMed
5 Heidenreich PA, Bozkurt B, Aguilar D, Allen LA, Byun JJ, Colvin MM, et al. 2022 AHA/ACC/HFSA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2022;145(18):e895–e1032.
PubMed
6 Vaduganathan M, Docherty KF, Claggett BL, Jhund PS, de Boer RA, Hernandez AF, et al. SGLT-2 inhibitors in patients with heart failure: a comprehensive meta-analysis of five randomised controlled trials. Lancet. 2022;400(10354):757–67.
Crossref PubMed
7 Ekman I, Andersson G, Boman K, Charlesworth A, Cleland JG, Poole-Wilson P, et al. Adherence and perception of medication in patients with chronic heart failure during a five-year randomised trial. Patient Educ Couns. 2006;61(3):348–53.
Crossref
8 George J, Shalansky SJ. Predictors of refill non-adherence in patients with heart failure. Br J Clin Pharmacol. 2007;63(4):488–93.
Crossref
9 MacDonald BJ, Barry AR, Turgeon RD. Decisional needs and patient treatment preferences for heart failure medications: a scoping review. CJC Open. 2023;5(2):136–47.
Crossref PubMed PMC
10 Horne R, Weinman J, Hankins M. The beliefs about medicines questionnaire: the development and evaluation of a new method for assessing the cognitive representation of medication. Psychol Health. 1999; 14(1):1–24.
Crossref
11 Horne R, Weinman J. Patients’ beliefs about prescribed medicines and their role in adherence to treatment in chronic physical illness. J Psychosom Res. 1999;47(6):555–67.
Crossref
12 Horne R, Weinman J. Self-regulation and self-management in asthma: exploring the role of illness perceptions and treatment beliefs in explaining non-adherence to preventer medication. Psychol Health. 2002; 17(1):17–32.
Crossref
13 Percival M, Cottrell WN, Jayasinghe R. Exploring the beliefs of heart failure patients towards their heart failure medicines and self care activities. Int J Clin Pharm. 2012;34(4):618–25.
Crossref PubMed
14 Ethnic or cultural origin reference guide, Census of Population, 2021. Statistics Canada; 2022 Mar 30 [updated 2022 Oct 26, cited 2024 Jul 22]. Available from: https://www12.statcan.gc.ca/census-recensement/2021/ref/98-500/008/98-500-x2021008-eng.cfm
15 Stanbrook MB, Salami B. CMAJ’s new guidance on the reporting of race and ethnicity in research articles [editorial]. CMAJ. 2023; 195(6):E236–8.
Crossref PubMed PMC
16 Horne R, Chapman SC, Parham R, Freemantle N, Forbes A, Cooper V. Understanding patients’ adherence-related beliefs about medicines prescribed for long-term conditions: a meta-analytic review of the Necessity-Concerns Framework. PLoS One. 2013;8(12):e80633.
Crossref PMC
17 Breathett K, Yee E, Pool N, Hebdon M, Crist JD, Knapp S, et al. Does race influence decision making for advanced heart failure therapies? J Am Heart Assoc. 2019;8(22):e013592.
Crossref PubMed PMC
18 Barry AR, Wang EHZ, Chua D, Zhou L, Hong KMH, Safari A, et al. Patients’ beliefs about their cardiovascular medications after acute coronary syndrome: a prospective observational study. CJC Open. 2023; 5(10):745–53.
Crossref PubMed PMC
19 Social determinants of health and health inequalities. Government of Canada, Public Health Agency of Canada; 2024 [cited 2024 Jul 22]. Available from: https://www.canada.ca/en/public-health/services/health-promotion/population-health/what-determines-health.html
20 White-Williams C, Rossi LP, Bittner VA, Driscoll A, Durant RW, Granger BB, et al. Addressing social determinants of health in the care of patients with heart failure: a scientific statement from the American Heart Association. Circulation. 2020;141(22):e841–63.
Crossref PubMed
Address correspondence to: Dr Arden Barry, Faculty of Pharmaceutical Sciences, The University of British Columbia, 2405 Wesbrook Mall, Vancouver BC V6T 1Z3, email: arden.barry@ubc.ca
Competing interests: For activities not directly related to the study reported here, Arden Barry has received speaker’s honoraria from the Canadian Society of Hospital Pharmacists (now the Canadian Society of Healthcare-Systems Pharmacy), the American College of Clinical Pharmacy, and Pharmacy Practice + Business magazine; and Tanya Dhanoa received travel support from the Canadian Society of Transplantation. No other competing interests were declared.
Funding: The creation of patient recruitment materials for this study was supported by start-up funding from the Faculty of Pharmaceutical Sciences, The University of British Columbia.
Submitted: July 30, 2024
Accepted: May 12, 2025
Published: August 13, 2025
© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 3, 2025