Lillian Lo, Sarah Masson, Matthew Brons, and Benjamin LeungTo cite: Lo L, Masson S, Brons M, Leung B. Exploring polypharmacy in the BC correctional health setting. Can J Hosp Pharm. 2025;78(2):e3708. doi: 10.4212/cjhp.3708
ABSTRACT
Background
Greater burdens of comorbidity and exposure to unique environmental factors predispose incarcerated individuals to polypharmacy and inappropriate prescribing. There is limited literature investigating polypharmacy within the correctional health setting.
Objectives
To determine the median number of medications prescribed per client at facilities in British Columbia, to determine the proportion of clients meeting the definition for polypharmacy, to identify the top medication categories prescribed, and to screen for potential drug therapy problems among those with polypharmacy.
Methods
An observational point prevalence study of adult clients with one or more active medications on the census date at 5 correctional health facilities in British Columbia was conducted. Clients were excluded if they had one-time or no medication orders on the census date.
Results
Of the 500 clients screened, 420 were included in the final analysis. Across the centres, the median number of medications ranged from 3 to 5 per client, and the rate of polypharmacy ranged from 23% to 41%. Of the scheduled medications, opioid agonist therapy and psychotropics were the leading categories prescribed across all facilities. Non-opioid analgesics were the top “as needed” medications prescribed at 4 of the 5 facilities. The leading potential drug therapy problem identified was drug interactions resulting in additive sedation.
Conclusions
Polypharmacy was present within all facilities in this study, with more than 25% of clients affected at 3 of the sites. The top medications prescribed aligned with those identified in the literature; however, there remain opportunities for therapy optimization.
Keywords: polypharmacy, correctional health, incarceration
RÉSUMÉ
Contexte
Le fardeau plus important associé aux comorbidités et à l’exposition à des facteurs environnementaux uniques prédispose les personnes incarcérées à la polypharmacie et à des prescriptions inappropriées. La littérature sur la polypharmacie dans le cadre des services de santé dans le milieu correctionnel est limitée.
Objectifs
Déterminer le nombre médian de médicaments prescrits par client dans des établissements en Colombie-Britannique; déterminer la part de clients répondant à la définition de la polypharmacie; recenser les principales catégories de médicaments prescrits; et procéder au dépistage des problèmes potentiels de thérapie médicamenteuse chez les clients présentant de la polypharmacie.
Méthodologie
Une étude observationnelle de prévalence ponctuelle des adultes prenant un ou plusieurs médicaments actifs à la date du recensement a été menée dans 5 établissements de santé correctionnelle en Colombie-Britannique. Les clients étaient exclus s’ils n’avaient qu’une prescription unique ou aucune ordonnance médicamenteuse à la date du recensement.
Résultats
Sur les 500 clients testés, 420 ont été inclus dans l’analyse finale. Dans les différents centres, le nombre médian de médicaments variait de 3 à 5 par client, et le taux de polypharmacie variait de 23 % à 41 %. Parmi les médicaments programmés, la thérapie agoniste des opioïdes et les psychotropes étaient les principales catégories prescrites dans tous les établissements. Les analgésiques non opioïdes étaient les médicaments les plus prescrits « au besoin » dans 4 des 5 établissements. Les interactions médicamenteuses entraînant une sédation additive constituaient le principal problème potentiel de la thérapie médicamenteuse recensé.
Conclusions
La polypharmacie était présente dans tous les établissements de cette étude, avec plus de 25 % des clients touchés dans 3 des sites. Les principaux médicaments prescrits étaient en accord avec ceux indiqués dans la littérature; cependant, il reste des occasions d’optimiser la thérapie.
Mots-clés: polypharmacie, santé correctionnelle, incarcération
Polypharmacy is commonly defined as taking 5 or more medications, including prescription, over-the-counter, and/or traditional and complementary therapies.1 Irrespective of the appropriateness of the individual medications, polypharmacy is associated with various risks, including death, adverse drug reactions (ADRs), admission to hospital, drug–drug or drug–disease interactions, and poor adherence.2,3
Clients in correctional health settings may experience polypharmacy.4,5 Internal (unpublished) data from the British Columbia Correctional Health Services revealed an average of 6.6 medications prescribed per client in 2022. Incarcerated individuals often suffer a higher burden of comorbidities than the general population,6 specifically more communicable diseases and mental health and substance use disorders.1 Although greater health demands may necessitate multiple medications, concerns about polypharmacy exist.6 For instance, prescribing multiple agents before initial regimens are optimized has been identified as an issue in the correctional health literature.4 An Australian systematic review on the prescribing of psychotropic drugs in the corrections setting revealed polypharmacy as a common theme, specifically the use of multiple PRN (“as needed”) medications.5 Furthermore, there are concerns that psychotropics may be inappropriately prescribed to subdue clients rather than to treat their underlying medical condition.7 Excessive or inappropriate prescribing may also contribute to misuse or diversion of medications, as well as interactions with illicit substances.8
There is minimal literature investigating medication use patterns in the correctional health setting.2,7,9 This study was undertaken to characterize the medication therapy of clients in correctional facilities in British Columbia, with a particular focus on polypharmacy.
An observational, point prevalence, multicentre review of prescription data from electronic medical records (EMRs) was conducted. To ensure adequate representation by sex, client status (sentenced, remanded), and geography, 5 provincial facilities that receive medical services from BC Correctional Health Services were selected: Alouette Correctional Centre for Women (ACCW), Fraser Regional Correctional Centre (FRCC), Prince George Regional Correctional Centre (PGRCC), Surrey Pretrial Services Centre (SPSC), and Vancouver Island Regional Correctional Centre (VIRCC). ACCW is the only all-women’s facility in British Columbia, mostly with remanded clients. FRCC is an all-male facility for sentenced clients, whereas the remaining sites house primarily remanded males. These facilities are managed by BC Mental Health and Substance Use Services (BCMHSUS). All provincial facilities are served by one centralized pharmacy. Facilities do not use preprinted order sets; instead, all medications are prescribed on an individual basis.
Consistent with the literature, we identified a single census day for each facility to calculate medication prevalence.2,9 To maximize the data available for assessment, the BCMHSUS analytics team identified the highest bed count day between July and December 2022 at each site to be the census date. These dates were July 27 for FRCC, November 16 for VIRCC, November 21 for SPSC, December 9 for ACCW, and December 11 for PGRCC. Selection was limited to July 2022 onward because prescribers were mandated to include diagnosis information in the EMR prescription field after this date, and this information informed our secondary outcome assessment. For each date, the analytics team randomly selected a convenience sample of 100 clients per facility for screening. Clients who were 18 years or older with one or more medications (scheduled or PRN) active on the census date were included in our analysis. Those with one-time orders and those not taking medications were excluded.
The University of British Columbia Children’s and Women’s Clinical Research Ethics Board deemed this project to be a quality improvement initiative, which was thus exempt from ethics approval.
The primary outcomes were the median count of medications (scheduled and PRN) and the proportion of clients with polypharmacy (based on scheduled medications only) at each facility on the census date. Secondary outcomes were the top 5 prescribed medication classes for scheduled, PRN, and high-risk medications at each facility and potential drug therapy problems (DTPs) among clients with polypharmacy.
High-risk medications were categorized as “high-alert”, “independent double check”, or “double check”, as per BCMHSUS drug policies.10,11 High-alert medications (e.g., methadone) have an increased risk of causing significant harm if administered in error.10 Independent double check medications (e.g., parenteral narcotics) require 2 clinicians to separately verify the medication and address any discrepancies before administration.11 Double check medications (e.g., insulin, oral narcotics) require 2 clinicians to verify the medication together before administration.11 In screening for potential DTPs, medications were assessed according to their dose, their appropriateness for the indication(s) listed, potential interactions, and duration of therapy. DTPs were categorized according to the Canadian consensus on clinical pharmacy key performance indicators.12
The BCMHSUS analytics team extracted de-identified prescription data from the clients’ EMRs, which included details about medication regimens, prescription durations, and diagnoses (where available). A pharmacy resident investigator (L.L.) categorized the data in an Excel spreadsheet (Microsoft Corporation) and screened for potential DTPs, with clinical pharmacist investigators (M.B., B.L.) randomly auditing data for 10% of the records. Discrepancies were resolved by consensus.
The following baseline characteristics were collected: age, sex, Indigenous self-identification, facility, and diagnoses (where available). Medications were categorized by their respective drug classes; those that did not fall into the prespecified categories were sorted as “other.” Multiple strengths or routes of administration for the same medication were counted as one entry. Long-acting injectable antipsychotics and injectable opiate agonist therapy (OAT) given before the census date were included if the next dose was ordered for the correct interval. Once the 5 most commonly prescribed medication classes were determined, the proportion of clients taking at least one medication from each of the given classes at each facility was calculated.
Means and medians were used to describe continuous variables, and proportions were used for dichotomous variables. All analyses were performed using Microsoft Excel.
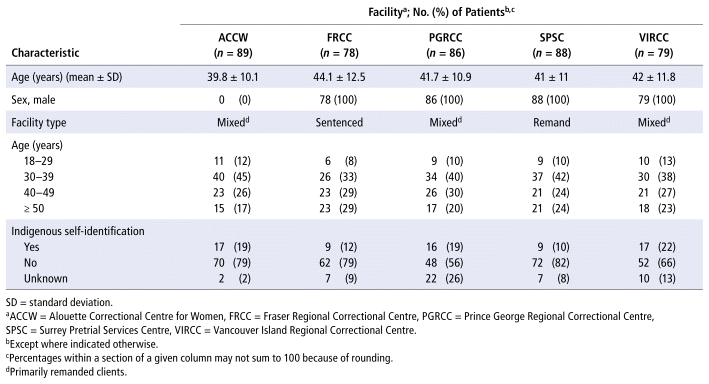
Of the 500 clients screened, 420 met the inclusion criteria for our analysis (Table 1); the remaining 80 were not taking any medications. Indigenous self-identification (First Nations, Métis, Inuit) ranged from 10% to 22% at each facility.
TABLE 1 Baseline Characteristics

The median number of medications ranged from 3 to 5 per client (Table 2). VIRCC had the greatest proportion of clients with polypharmacy (41%), followed by ACCW (36%), FRCC (28%), SPSC (24%), and finally PGRCC (23%). Polypharmacy was most prevalent in the 30- to 39-year age group at ACCW, FRCC, and VIRCC, and among those 40 years of age or older at PGRCC and SPSC. Among those who self-identified as Indigenous, VIRCC had the greatest proportion with polypharmacy.
TABLE 2 No. of Medications and Rate of Polypharmacy, by Age Group
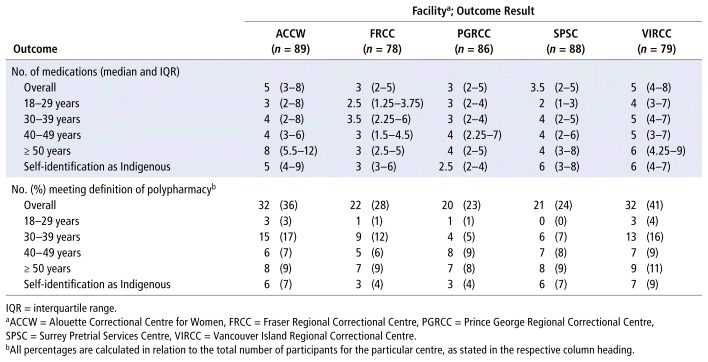
Except at PGRCC, OAT was the most commonly prescribed scheduled medication, followed by either second-generation antipsychotics or “other antidepressants”, which encompassed medications other than selective serotonin reuptake inhibitors, serotonin–norepinephrine reuptake inhibitors, and tricyclic antidepressants (Table 3). Trazodone and mirtazapine were the most common agents in the category of other antidepressants. Beyond the psychotropics, melatonin, the sole agent in the “sleep” category, and antihistamines, predominantly hydroxyzine, were frequently prescribed. Wide use of topical dermatological products, including corticosteroids and acne compounds, was seen across the centres as well.
TABLE 3 Top Categories of Scheduled, PRN, and High-Risk Medications
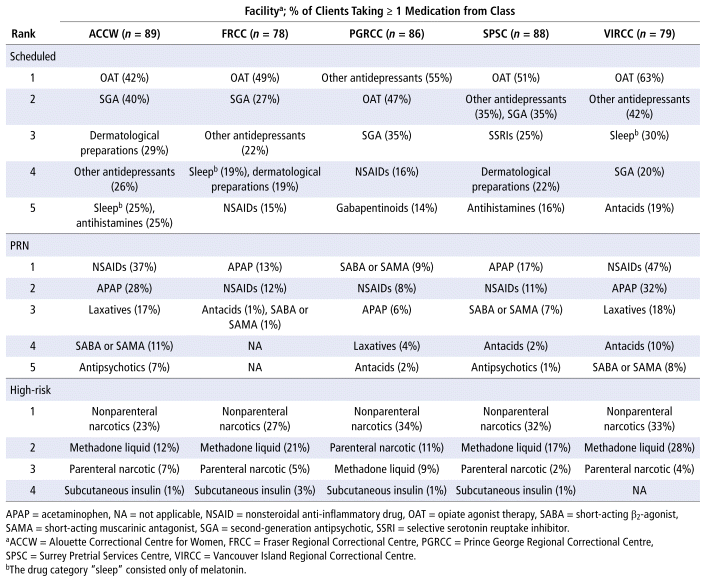
Of the PRN medications, non-opioid analgesia (acetaminophen, nonsteroidal anti-inflammatory drugs [NSAIDs]) was the most frequently prescribed medication category at 4 facilities (Table 3). All centres had short-acting β2-agonists and short-acting muscarinic antagonists, as well as a gastrointestinal agent (laxative or acid reducer), among their top medications. ACCW and SPSC had antipsychotics (first- and second-generation) as the fifth most commonly prescribed PRN medication.
The high prevalence of OAT was reflected in the data for high-risk medications (Table 3). Nonparenteral narcotics, primarily buprenorphine/naloxone and slow-release forms of oral morphine, was the leading category at all facilities. Except at PGRCC, liquid methadone was the next most frequently prescribed agent, followed by parenteral narcotics, which consisted exclusively of extended-release buprenorphine.
The DTPs identified in this study were all considered “potential” due to our inability, in the absence of a chart review, to confirm their relevance. The most common potential DTP category was ADR, encompassing issues such as drug–drug interactions, drug–disease interactions, and unsafe medication due to client risk factors (e.g., low renal function)12 (Figure 1). All ADR-related DTPs were due to drug–drug interactions, primarily additive sedation from concomitant prescribing of OAT, sedating antipsychotics (e.g., olanzapine, quetiapine), sedating antidepressants (e.g., mirtazapine, trazodone, tricyclic antidepressants), hydroxyzine, cyclobenzaprine, and/or gabapentinoids. Other drug–drug interactions observed in this study included additive anticholinergic burden and QTc prolongation.
|
| ||
|
FIGURE 1 Breakdown of drug-related problems by facility. ACCW = Alouette Correctional Centre for Women, FRCC = Fraser Regional Correctional Centre, PGRCC = Prince George Regional Correctional Centre, SPSC = Surrey Pretrial Services Centre, VIRCC = Vancouver Island Regional Correctional Centre. | ||
The next most common potential DTP category was unnecessary drug therapy. This category included long-term use of natural health products for unclear indications, duplication of therapy (e.g., co-prescription of a selective serotonin reuptake inhibitor and a serotonin–norepinephrine reuptake inhibitor), triple or quadruple antipsychotic therapy, and extensive prescription lengths for medications that would warrant earlier reassessment (e.g., 1-year course of antidiarrheal, proton pump inhibitor, or scheduled high-dose NSAID).
Use of medications with limited evidence was captured under the potential DTP of “ineffective drug”. This category included long-term cyclobenzaprine for low-back pain13 and hydroxyzine for sleep.14 Lastly, under the potential DTP of “dose too high”, we found a total of 5 clients who were taking quantities of NSAIDs exceeding the daily allowable dose.
Polypharmacy was present in all facilities, ranging from 23% to 41% of clients in each centre, although its prevalence was likely underestimated, given that PRN medications were excluded from the count. While often associated with adults 65 years or older,15 polypharmacy also affects younger populations due to factors such as mental health conditions, lack of a primary care physician, poor medical record keeping, and disjointed transitions in care.16 Staff turnover,6 incomplete medication histories, and health complexities,4 in addition to environmental factors inducing or aggravating poor health, have also been identified in the correctional health literature as potential contributors to inappropriate prescribing and polypharmacy.
The top scheduled medications in BC correctional facilities (OAT, psychotropics) were unsurprising. According to 2022 BC Correctional Health Services statistics, more than 60% of clients had mental health or substance use concerns,17 which would explain the high prevalence of OAT and psychotropics. Sleep disorders are also extremely prevalent in correctional facilities due to overcrowding, excessive noise, interruption of daily routines, temperature variation, substance withdrawal, uncomfortable bedding, and concomitant mental health conditions.18 Due to the risk of diversion and misuse, antihistamines, melatonin, and psychotropics with a sedating profile are prescribed preferentially over hypnotics for treatment of sleep problems.8
The high prevalence of substance use and conditions resulting from incarceration, such as anxiety or sleeping issues, may lead to somatic disturbances requiring analgesia.19 This factor may have contributed to non-opioid analgesics being the most prescribed among the PRN medications. Laxatives were also among the top PRN medications prescribed, possibly due to opioid-induced constipation or constipation from poor dietary intake. Use of short-acting bronchodilators may be explained by the higher prevalence of tobacco use disorder, asthma, and chronic obstructive pulmonary disease observed in incarcerated individuals, as described in the literature.20 Interestingly, we observed greater prescribing of PRN antipsychotics for female clients. Gender-related differences in prescribing were highlighted in a point prevalence study of European inmates.9 In that study, there was greater psychotropic prescribing among female clients, potentially due to greater mental health concerns, as well as social and situational factors of imprisonment disproportionately affecting women.9
In the current study, there was substantial use of high-alert medications, mostly accounted for by the large quantities of OAT prescribed. Use of high-alert medications carries an inherently greater risk of harm if the drugs are administered incorrectly. These observations support the need for periodic review of medication administration policies and procedures based on patient safety event data and best practice guidelines to ensure client safety.
Despite limited data, we would like to highlight our results for the Indigenous client subgroup, which in Canada consists of First Nations, Métis, and Inuit peoples.21 Indigenous peoples make up approximately 6% of the BC population22 and were overrepresented in our study, accounting for approximately 16% of the clients. Nonetheless, our data may still underrepresent the proportion of Indigenous clients in custody in British Columbia, given that 2022 data estimated an average of 35% of individuals who self-identified as Indigenous.22 We hypothesize that underreporting may be rooted, in part, in the extensive history of systemic racism faced by this population, leading individuals to avoid self-identifying as Indigenous out of fear of discrimination, mistrust, and stereotyping at the point of care.23 Indigenous peoples are also at increased risk of polypharmacy, as they tend to have a higher prevalence of chronic conditions than non-Indigenous individuals.24 However, disparities in access and fears of mistreatment leading to avoidance of the health care system contribute to potential undertreatment in this population.23
The lack of a chart review hindered us from performing a comprehensive DTP assessment. As a result, not all DTP categories were assessed, and DTPs identified were considered “potential”, as their clinical relevance could not be accurately determined. The DTPs identified are hypothesis-generating, however, providing areas for potential optimization and justifying the performance of comprehensive chart reviews to better understand prescribing practices. For example, the large quantities of hydroxyzine prescribed, presumably for sleep, may indicate a need to review approaches to insomnia management, including correcting underlying factors such as pain, mood disorders, environment, and routines. Another example is the use of multiple antipsychotics observed in some clients, including at subtherapeutic doses. It may be beneficial to perform an in-depth assessment for prescribing appropriateness, such as determining whether adequate medication trials are being performed before adding or switching agents. Additionally, it would be worthwhile to investigate whether clinicians are performing an in-depth psychiatric history to determine the pattern of past medication trials to prevent using agents that offer minimal benefit to clients.
Overall, the results of this study enhance our understanding of polypharmacy in BC correctional centres. To our knowledge, this study is the first of its kind in British Columbia, laying the foundation upon which subsequent studies can explore prescribing practices in these centres, the appropriateness of medications prescribed, and the concept of rational polypharmacy through an in-depth chart review. Within our own setting, it may also be important to compare the appropriateness of medication use at centres with and without an on-site clinical pharmacist. Clinical pharmacists play an integral part in interdisciplinary teams, ensuring effective, safe medication therapy. Their active role in overseeing and optimizing medication management may reduce the risks of polypharmacy. Moreover, insights from future studies may highlight prescribing practices and direct future education for the health care team to optimize patient care outcomes.
Several factors limit the interpretation of results in this study. The point prevalence design allows only a snapshot of medication use, without accounting for changes over time. As well, we only considered individuals who were taking medications on the census date at each centre; therefore, our medication counts may be inflated. Additionally, the methodology may have introduced sampling bias. Several factors may have affected each client’s medication count on the census date. For example, if the client recently entered the facility, regular medications may not have been reviewed and reordered by the on-site physician. Conversely, extra medications may have been added temporarily for acute substance withdrawal upon admission. Also, certain days may have underrepresentation of medications due to lack of an on-site prescriber.
Another limitation of our methodology was the exclusion of PRN medications from the analysis, which may have led to underestimation of polypharmacy. Future studies should include data from medication administration records to capture PRN use and thus allow for more accurate medication counts. Differences in bed counts across the 5 sites led to inconsistent representation of clients from each facility, affecting generalizability. Our data source also lacked the ability to distinguish between new and re-admitted clients, leading to potential data duplication. Finally, the absence of a comprehensive chart review prevented us from thoroughly assessing medication appropriateness and ascertaining the presence of certain DTPs.
In this study of correctional centres in British Columbia, the rate of polypharmacy ranged from 23% to 41%. The most frequent prescriptions aligned largely with expectations for this unique population; however, opportunities to optimize therapy remain. Future studies should include chart reviews to allow better characterization of medication use and quantification of polypharmacy in this vulnerable population.
1 Medication safety in polypharmacy [technical report]. WHO/UHC/SDS/2019.11. World Health Organization; 2019 [cited 2024 Jun 22]. Available from: https://www.who.int/docs/default-source/patient-safety/who-uhc-sds-2019-11-eng.pdf
2 Annaheim B, Wangmo T, Bretschneider W, Handtke V, Elger BS, Belardi A, et al. Polypharmacy and drug-drug interactions among older and younger male prisoners in Switzerland. Int J Prison Health. 2019; 15(3):250–61.
Crossref PubMed
3 Masnoon N, Shakib S, Kalisch-Ellett L, Caughey GE. What is polypharmacy? A systematic review of definitions. BMC Geriatr. 2017;17(1):230.
Crossref PubMed PMC
4 Magola-Makina E, Abuzour AS, Ashcroft DM, Dunlop J, Brown P, Keers RN. Exploring the challenges to safer prescribing and medication monitoring in prisons: a qualitative study with health care staff. PLoS One. 2022;17(11):e0275907.
Crossref PubMed PMC
5 Griffiths EV, Willis J, Spark MJ. A systematic review of psychotropic drug prescribing for prisoners. Aust N Z J Psychiatry. 2012;46(5):407–21.
Crossref PubMed
6 Abuzour AS, Magola-Makina E, Dunlop J, O’Brien A, Khawagi WY, Ashcroft DM, et al. Implementing prescribing safety indicators in prisons: a mixed methods study. Brit J Clin Pharmacol. 2022;88(4):1866–84.
Crossref
7 Kjelsberg E, Hartvig P. Too much or too little? Prescription drug use in a nationwide prison population. Int J Prison Health. 2005;1(1):75–87.
Crossref
8 Bicknell M, Farmer D, Watson C. Safer prescribing in prisons: guidance for clinicians. 2nd ed. Royal College of General Practitioners; 2019 [cited 2024 Jun 22]. Available from: https://elearning.rcgp.org.uk/pluginfile.php/176185/mod_book/chapter/620/RCGP-safer-prescribing-in-prisons-guidance-jan-2019.pdf
9 Hassan L, Senior J, Webb RT, Frisher M, Tully MP, While D, et al. Prevalence and appropriateness of psychotropic medication prescribing in a nationally representative cross-sectional survey of male and female prisoners in England. BMC Psychiatry. 2016;16:346.
Crossref PubMed PMC
10 High-alert medications [policy]. Version 4. Provincial Health Services Authority, BC Mental Health & Substance Use Services, Pharmacy & Therapeutics Committee; 2024 [cited 2024 Jun 22]. Available from: http://shop.healthcarebc.ca/phsa/bcmhsus/C-03-11-50134.pdf
11 Independent double check and double check of medication administration [procedure]. Version 5.1. Provincial Health Services Authority, BC Mental Health & Substance Use Services, Pharmacy & Therapeutics Committee; 2024 [cited 2024 Jun 22]. Available from: http://shop.healthcarebc.ca/phsa/bcmhsus/C-03-11-50354.pdf
12 Fernandes O, Toombs K, Pereira T, Lyder C, Bjelajac Mejia A, Shalansky S, et al. Canadian consensus on clinical pharmacy key performance indicators: quick reference guide. Canadian Society of Hospital Pharmacists; 2015 [cited 2024 Jun 22]. Available from: https://www.cshp.ca/common/Uploaded%20files/PDFs/CSPH-Can-Concensus-cpKPI-QuickReferenceGuide_June_2017.pdf
13 Browning R, Jackson JL, O’Malley PG. Cyclobenzaprine and back pain: a meta-analysis. Arch Intern Med. 2001;161(13):1613–20.
Crossref PubMed
14 Matheson E, Hainer BL. Insomnia: pharmacologic therapy. Am Fam Physician. 2017;96(1):29–35.
PubMed
15 Delara M, Murray L, Jafari B, Bahji A, Goodarzi Z, Kirkham J, et al. Prevalence and factors associated with polypharmacy: a systematic review and meta-analysis. BMC Geriatr. 2022;22:601.
Crossref PubMed PMC
16 Halli-Tierney A, Scarbrough C, Carroll D. Polypharmacy: evaluating risks and deprescribing. Am Fam Physician. 2019;100(1):32–8.
PubMed
17 Profile of BC Corrections. Government of British Columbia; 2023 [cited 2024 Jun 22]. Available from: https://www2.gov.bc.ca/assets/gov/law-crime-and-justice/criminal-justice/corrections/reports-publications/bc-corrections-profile.pdf
18 Griffiths C, Hina F. Prisoner’s insomnia prevalence, insomnia associated factors and interventions with sleep as an outcome: a review and narrative analysis. Int J Prison Health. 2022;18(1):27–42.
Crossref
19 Elger BS, Bindschedler M, Goehring C, Revaz SA. Evaluation of drug prescription at the Geneva prison’s outpatient service in comparison to an urban outpatient medical service. Pharmacoepidemiol Drug Saf. 2004;13(9):633–44.
Crossref PubMed
20 Viglianti EM, Iwashyna TJ, Winkelman TNA. Mass incarceration and pulmonary health: guidance for clinicians. Ann Am Thorac Soc. 2018;15(4):409–12.
Crossref PubMed PMC
21 Focus on geography series, 2021 Census of Population. British Columbia province. Statistics Canada; 2022 [cited 2024 Jun 22]. Available from: https://www12.statcan.gc.ca/census-recensement/2021/as-sa/fogs-spg/page.cfm?lang=E&topic=8&dguid=2021A000259
22 BC Corrections adult custody statistics [interactive tool]. BC Ministry of Public Safety and Solicitor General; 2024 [cited 2024 Jun 22]. Available from: https://app.powerbi.com/view?r=eyJrIjoiNzE2ZmM5MTMtN2U5ZC00ZGQ1LTk4YWUtY2UwNDdiYWI5NTQyIiwidCI6IjZmZGI1MjAwLTNkMGQtNGE4YS1iMDM2LWQzNjg1ZTM1OWFkYyJ9&pageName=ReportSection69506dda63e5b4460c64
23 Turpel-Lafond ME. In plain sight: addressing Indigenous-specific racism and discrimination in B.C. health care [Addressing Racism Review summary report]. Government of British Columbia; 2020 [cited 2024 Jun 22]. Available from: https://engage.gov.bc.ca/app/uploads/sites/613/2020/11/In-Plain-Sight-Summary-Report.pdf
24 Gaspard G, Gadsby C, Preston C. Promoting healthy medication use through Indigenous knowledge sharing: a coyote story. Int J Indig Health. 2021;16(2):166–76.
Address correspondence to: Dr Lillian Lo, Royal Columbian Hospital, 330 East Columbia Street, New Westminster BC V3L 3W7, email: lillian.lo@fraserhealth.ca
Competing interests: None declared.
Funding: None received.
Acknowledgements: The authors thank Felix Loo, Strategic Information Management Analyst at the British Columbia Provincial Health Services Authority, for providing support in accessing the research data.
Submitted: August 24, 2024
Accepted: November 23, 2024
Published: May 14, 2025
© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 2, 2025