Sukhpreet Poonia, Mimi Nguyen, Anna Yee, Melanie Eaton, and Robin ChoTo cite: Poonia S, Nguyen M, Yee A, Eaton M, Cho R. Impact of clinical pharmacists on interdisciplinary mental health teams in a community setting: a retrospective chart review. Can J Hosp Pharm. 2025;78(3):e3737. doi: 10.4212/cjhp.3737
ABSTRACT
Background
Clinical pharmacists play a pivotal role within collaborative care environments, with well-documented contributions on multidisciplinary teams in these settings. Their specific impacts on community mental health and substance use (MHSU) teams remains to be characterized in a publicly funded regional program within Fraser Health.
Objectives
To describe the impact of medication reviews performed by clinical pharmacists and the uptake by prescribers of pharmaceutical interventions recommended by the clinical pharmacists in an ambulatory MHSU setting.
Methods
This study involved a retrospective chart review of 100 patients referred to Fraser Health Community MHSU Pharmacy Services across 20 communities within the Fraser Health Authority in British Columbia.
Results
Clinical pharmacists identified a total of 310 drug therapy problems (DTPs) among the 100 patients. The most common DTPs identified were adverse drug reactions (n = 97, 31%), ineffective drug therapy (n = 68, 22%), unnecessary medications (n = 46, 15%), and the need for additional drug therapy (n = 35, 11%). Prescribers accepted 1 or more of the recommendations made by the clinical pharmacist in 88% (81/92) of the cases with follow-up. More than half (55%, 171/310) of the identified DTPs were resolved within 6 months of the initial pharmacist assessment.
Conclusions
In this study, embedding clinical pharmacists within community MHSU care teams enhanced medication safety and therapeutic optimization, while reducing polypharmacy. Future investigation into the benefits for long-term clinical outcomes is warranted.
KEYWORDS: mental health, clinical pharmacist, retrospective chart review, multidisciplinary
RÉSUMÉ
Contexte
Les pharmaciens cliniciens jouent un rôle essentiel dans les environnements de soins collaboratifs, où leurs contributions au sein des équipes multidisciplinaires sont bien documentées. Leur impact précis sur les équipes en santé mentale communautaire et en toxicomanie (SMCT) doit encore être précisé dans un programme régional financé par des fonds publics au sein de l’Autorité sanitaire Fraser.
Objectifs
Décrire les conséquences des examens des médicaments menés par les pharmaciens cliniciens et l’adoption par les prescripteurs des interventions pharmaceutiques recommandées par les pharmaciens cliniciens dans un environnement ambulatoire en SMCT.
Méthodologie
Cette étude impliquait un examen rétrospectif des dossiers de 100 patients orientés vers les services pharmaceutiques en SMCT dans 20 communautés au sein de l’Autorité sanitaire Fraser, en Colombie-Britannique.
Résultats
Parmi les 100 patients, les pharmaciens cliniciens ont recensé 310 problèmes de traitement médicamenteux au total. Les plus courants étaient les réactions indésirables aux médicaments (n = 97, 31 %), l’inefficacité de la thérapie médicamenteuse (n = 68, 22 %), les médicaments inutiles (n = 46, 15 %) et le besoin d’une thérapie médicamenteuse supplémentaire (n = 35, 11 %). Les prescripteurs ont accepté une ou plusieurs des recommandations formulées par le pharmacien clinicien dans 88 % (81/92) des cas faisant l’objet d’un suivi. Plus de la moitié des problèmes de traitement médicamenteux recensés (55 %, 171/310) ont été résolus dans les 6 mois suivant l’évaluation initiale par le pharmacien.
Conclusions
Les résultats de cette étude ont montré que l’intégration des pharmaciens cliniciens au sein des équipes de soins en SMCT renforce la sécurité des médicaments et l’optimisation thérapeutique, tout en réduisant la polypharmacie. Des recherches futures sur les bénéfices pour les résultats cliniques à long terme sont nécessaires.
Mots-clés: santé mentale, pharmacien clinicien, revue rétrospective des dossiers, multidisciplinaire
Mental health and substance use (MHSU) disorders continue to represent one of the leading causes of disability in Canada. In this country, the estimated annual economic cost is more than $50 billion for mental illness and approximately $40 billion for substance use.1–3
Not only are MHSU disorders taxing for the health care system, but they are also extremely detrimental on an individual level. Collectively, MHSU conditions are estimated to reduce an individual’s life expectancy by 10 to 20 years, and they are linked to unemployment rates as high as 70%–90% for people with severe illness.4–6 About 4000 Canadians per year die by suicide related to mental health disorders, and the rate is disproportionately higher (typically by a factor of 6) for Indigenous people than for non-Indigenous people.7,8
Despite the enormous disease burden nationally, wait times to access mental health services remain exceptionally long.9 With the prevalence of mental health illnesses such as generalized anxiety disorder, depression, and bipolar disorder nearly doubling from 2012 to 2022, the demands simply are not being met by the traditional standard of care.10 In a recent survey conducted by Statistics Canada, only about half of the participants with a diagnosed mood, anxiety, or substance use disorder reported talking to a health care provider about their mental health, and 1 in 3 participants reported unmet or partially unmet needs for mental health services.11
Conversely, numerous studies have recently described improved clinical outcomes and client satisfaction with the addition of clinical pharmacists to interdisciplinary primary care and mental health teams.12–19 The integration of clinical pharmacists has been associated with decreased inappropriate medication use, in addition to an increased number of clients receiving appropriate care, improved client engagement, improved health literacy, and reduced time and energy demands on prescribers and other health care providers.20 The role of pharmacists in certain environments such as primary care has expanded in recent years, leading to reduced hospitalizations and improved client safety, medication adherence, and quality of life.21
The objective of this study was to describe the overall clinical impact of comprehensive medication reviews conducted by clinical pharmacists in a community mental health setting in the Fraser Health region of British Columbia. We sought to do this by quantifying the drug therapy problems (DTPs) identified by clinical pharmacists and the recommendations made after a clinical pharmacist consultation. We also assessed prescriber uptake of the pharmacist’s recommendations.
This retrospective chart review included clients referred to Fraser Health MHSU Pharmacy Services for a comprehensive clinical pharmacy review between August 15, 2022, and May 15, 2023, up to a sample size of convenience involving the first 100 clients assessed during this period.
The Fraser Health MHSU Pharmacy Services program is a referral-based program delivered by 2 clinical pharmacists (S.P., A.Y.) and 1 clinical pharmacy technician (M.E.), who provide clinical pharmacy consultation services for 20 communities under the Fraser Health umbrella. Referrals to the program can be made by any prescriber located within the described geographic region, by fax or email, where the main concern is related to mental health or substance use–related disorders. A clinical pharmacist in the Fraser Health MHSU team will complete a one-time comprehensive work-up, which includes a chart review, client interview and subsequent identification of DTPs, and a plan to address the client’s unmet needs. Once a consultation is completed, the pharmacist’s recommendations are communicated back to the prescriber either verbally or in writing for follow-up and implementation. Changes to medications and ongoing follow-ups are completed by the client’s prescriber(s).
During the time frame defined above, client charts were reviewed in chronological sequence starting with those who received a clinical pharmacist consultation on August 15, 2022, until the predetermined sample size was achieved.
Data collected included participant demographic characteristics, medication regimen before pharmacist intervention, number and category of DTPs identified by the pharmacist, the pharmacist’s recommendations after assessment, and the rate of implementation of those recommendations by the client’s prescriber(s) within 6 months after the assessment.
The study protocol was reviewed by the Fraser Health Research Ethics Board (REB) and received an REB exemption due to the quality assurance and quality improvement nature of the project.
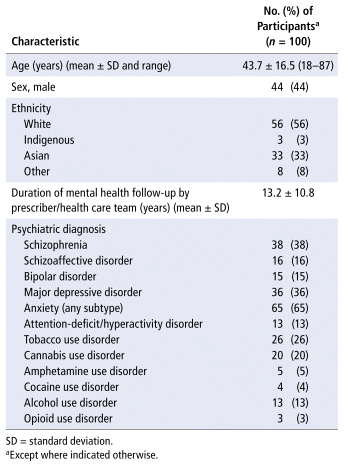
A total of 126 client charts were reviewed to reach the predefined sample size of 100 clients meeting the inclusion criteria. The remaining 26 client charts were excluded because these cases involved targeted questions relating to the client’s medication or were repeat referrals and therefore did not involve a comprehensive clinical pharmacist assessment. Client demographic and clinical characteristics are summarized in Table 1. The mean age of the group was 43.7 (range 18 to 87) years, and 44% of the participants were male. The average duration of mental health follow-up before the clinical pharmacist assessment was 13.2 years, and 73% of participants had more than 1 psychiatric diagnosis. All clinical pharmacy consultations were completed by a pharmacist within 2 months of receipt of the referral.
TABLE 1 Participant Characteristics

According to the 100 client charts reviewed, assessment by the clinical pharmacist identified a total of 310 DTPs. These DTPs were grouped in the following categories: experiencing adverse drug reaction (n = 97), prescribed drug therapy ineffective (n = 68), unnecessary medication (n = 46), needs additional drug therapy (n = 35), prescribed dose ineffective (n = 27), experiencing or at risk of experiencing a level C or D drug interaction as per Lexicomp’s drug interaction risk ratings22 (n = 16), experiencing medication nonadherence (n = 13) or prescribed dose too high (n = 8).
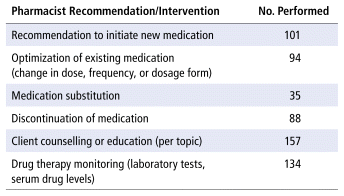
To address and resolve identified DTPs, the pharmacy team made recommendations that fell within the following categories (Table 2): initiation of 1 or more new medications, optimization of existing medication (change in dose, frequency, or dosage form), medication substitution, discontinuation of medication, client counselling or education, or drug therapy monitoring. A total of 609 such recommendations and interventions were either communicated to the prescriber, verbally or in writing, or implemented immediately during the client assessment.
TABLE 2 Summary of Recommendations and Actions across 100 Participants
Of the 100 participants, 92 saw their primary care provider following the pharmacist assessment. For these 92 participants, it was found that the prescribers agreed with and implemented 1 or more of the clinical pharmacist’s drug therapy recommendations in 88% (81/92) of cases with follow-up. Roughly 55% (171/310) of the DTPs identified by the clinical pharmacists were resolved within 6 months of the initial assessment.
Often, community treatment models for MHSU illnesses include psychiatrists, mental health nurses, social workers, and counsellors, but a clinical pharmacist may be lacking on such teams.15 This study aimed to look at the direct impacts of having clinical pharmacists embedded within community mental health teams at Fraser Health.
In our review, we found that consultation with the clinical pharmacist not only resulted in identification of numerous DTPs for each client, but also led to the resolution of such DTPs. Clients and their prescribers received recommendations from the clinical pharmacist for the resolution of these DTPs through optimization of medication regimens, client counselling or education, therapeutic drug monitoring, and/or laboratory monitoring recommendations.
Although we did not directly measure important patient outcomes such as hospitalization or reduction in polypharmacy, and we did not perform any cost-saving analyses, several other studies have previously shown that the pharmacy interventions described in this study do lead to positive patient outcomes.14,17,19,23–25
As mentioned above, the primary focus of this study was to quantify the impact of pharmacist assessment through direct care provided to clients. However, the importance and utility of clinical pharmacists within mental health teams is not solely limited to this aspect. The pharmacists working in this role within Fraser Health are also routinely expected to answer medication questions, assess and educate other health care providers about pertinent drug shortages, and provide formal education presentations to clients and health care workers, as well as performing movement disorder assessments and identifying other chronic disease management strategies for their clients.
Additionally, our clinical pharmacy consultation service accepts referrals from all prescribers in the Fraser Health region and is not limited to psychiatrist-initiated referrals. As such, we offer a low-barrier service to address client care needs for marginalized populations who may not otherwise have access to such services and resources in a timely manner.
The typical wait time that most clients experience to see a psychiatrist within our region is 3–6 months, longer in some cases.26 In contrast, the typical wait time to see a clinical pharmacist in our program is 6–8 weeks. By referring clients to the MHSU pharmacy team for medication optimization, family practitioners and nurse practitioners who lack extensive experience in caring for people with mental health conditions are able to have their clients’ concerns addressed in a more timely manner. As displayed here, the role of a clinical pharmacist within mental health teams has much potential, and, to our knowledge, this is the first study to date describing the impact of clinical pharmacists on community mental health teams in this type of publicly funded regional program within Fraser Health.
This study had some limitations. The clinical pharmacist services described here were provided in the community setting. Thus, a small proportion of participants were lost to follow-up (specifically, the 8 [8%] clients who never followed up with their prescribers after the clinical pharmacist assessment); this situation may be particularly challenging for clients with multiple or severe mental health illnesses. Additionally, despite 55% of DTPs being resolved within 6 months of the pharmacist assessment, it is probable that with a longer duration of follow-up, more recommendations might have been implemented, as the clinical pharmacists’ recommendations are usually made in a stepwise manner and are intended for gradual implementation over many months. Lastly, given that this was a retrospective chart review, the validity of the collected parameters was contingent on consistent, accurate, and complete documentation by the health care providers.
The scope and outcomes defined in this study provide a solid foundation for future research in this area. Future studies could evaluate the impact of clinical pharmacist interventions in a community setting on hospitalization rates, prevalence of and reduction in polypharmacy, and the actual or anticipated cost savings to clients or the health care system. Prior studies have assessed the benefits of pharmacists in acute care and primary care settings, and the results have been consistently favourable, highlighting the importance of including pharmacists on interdisciplinary teams.12–19 This study further highlights the role and impact of clinical pharmacists in a Canadian community mental health setting.
1 Smetanin P, Stiff D, Briante C, Adair CE, Ahmad S, Khan M. The life and economic impact of major mental illnesses in Canada: 2011 to 2041. RiskAnalytica, on behalf of Mental Health Commission of Canada; 2011.
2 Lim KL, Jacobs P, Ohinmaa A, Schopflocher D, Dewa CS. A new population-based measure of the economic burden of mental illness in Canada. Chronic Dis Can. 2008;28(3):92–8.
Crossref PubMed
3 Canadian Substance Use Costs and Harms Scientific Working Group. Canadian substance use costs and harms 2015–2017. Canadian Centre on Substance Use and Addiction; 2020.
4 Chesney E, Goodwin GM, Fazel S. Risks of all-cause and suicide mortality in mental disorders: a meta-review. World Psychiatry. 2014; 13(2):153–60.
Crossref PubMed PMC
5 Dewa CS, McDaid D. Investing in the mental health of the labor force: epidemiological and economic impact of mental health disabilities in the workplace. In: Schultz IZ, Rogers ES, editors. Work accommodation and retention in mental health. Springer; 2010. pp. 33–51.
6 Marwaha S, Johnson S. Schizophrenia and employment: a review. Social Psychiatry Psychiatr Epidemiol. 2004;39(5):337–49.
Crossref
7 Table 13-10-0392-01: Deaths and age-specific mortality rates, by selected grouped causes. Statistics Canada; 2020.
8 Kumar MB, Tjepkema M. Suicide among First Nations people, Métis and Inuit (2011–2016): findings from the 2011 Canadian Census Health and Environment Cohort. Catalogue no. 99-011-X2019001. Statistics Canada; 2019.
9 Mental illness and addiction: facts and statistics. Centre for Addition and Mental Health; [cited 2024 Oct 16]. Available from: https://www.camh.ca/en/driving-change/the-crisis-is-real/mental-health-statistics
10 Study: Mental disorders and access to mental health care. Statistics Canada; 2023 [cited 2024 Oct 16]. Available from: https://www150.statcan.gc.ca/n1/daily-quotidien/230922/dq230922b-eng.htm
11 Stephenson E. Mental disorders and access to mental health care. Statistics Canada; 2023 [cited 2024 Oct 16]. Available from: https://www150.statcan.gc.ca/n1/pub/75-006-x/2023001/article/00011-eng.htm
12 Hayhoe B, Cespedes JA, Foley K, Majeed A, Ruzangi J, Greenfield G. Impact of integrating pharmacists into primary care teams on health systems indicators: a systematic review. Br J Gen Pract. 2019; 69(687):e665–e674.
Crossref PubMed PMC
13 Davis B, Qian J, Ngorsuraches S, Jeminiwa R, Garza K. The clinical impact of pharmacist services on mental health collaborative teams: a systematic review. J Am Pharm Assoc (2003). 2020;60(5 Suppl): S44–S53.
Crossref PubMed PMC
14 Gisev N, Bell JS, O’Reilly CL, Rosen A, Chen TF. An expert panel assessment of comprehensive medication reviews of clients of community mental health teams. Soc Psychiatry Psychiatr Epidemiol. 2010; 45(11):1071–9.
Crossref
15 Gable KN, Stunson MJ. Clinical pharmacist interventions on an assertive community treatment team. Community Ment Health J. 2010; 46(4):351–5.
Crossref
16 Bell JS, Rosen A, Aslani PA, Whitehead P, Chen TF. Developing the role of pharmacists as members of community mental health teams: perspectives of pharmacists and mental health professionals. Res Social Admin Pharm. 2007;3(4):392–409.
Crossref
17 Chung B, Dopheide JA, Gregerson P. Psychiatric pharmacist and primary care collaboration at a skid-row safety-net clinic. J Natl Med Assoc. 2011;103(7):567–74.
PubMed
18 Tallian KB, Hirsch JD, Kuo GM, Chang CA, Gilmer T, Messinger M, et al. Development of a pharmacist-psychiatrist collaborative medication therapy management clinic. J Am Pharm Assoc (2003). 2012; 52(6):e252–8.
Crossref PubMed
19 Carvalhana V, Flak E. Role of the pharmacist on a multidisciplinary psychiatry team: impact on medication adherence in a community setting. J Pharm Technol. 2009;25(3):155–8.
Crossref
20 Innovation in primary care: integration of pharmacists into interprofessional teams. College of Family Physicians of Canada and Canadian Pharmacists Association; 2019 [cited 2024 Oct 16]. Available from: https://www.cfpc.ca/CFPC/media/Resources/Health-Policy/IPC-2019-Pharmacist-Integration.pdf
21 Gobis B, Reardon J, Yuen J, Meng Y, Mah S, Gill R, et al. A white paper on team-based primary health care in British Columbia. Context and opportunities for pharmacists. University of British Columbia, Faculty of Pharmaceutical Sciences; 2020 [cited 2024 Oct 16]. Available from: https://pharmsci.ubc.ca/white-paper-team-based-health-care-bc
22 UpToDate Lexidrug for individual clinicians and users [formerly Lexicomp]. Wolters Kluwer; [cited 2024 Oct 16]. Available from: https://store.wolterskluwercdi.com/CDI. Subscription required to access content.
23 Hattingh HL, Scahill S, Fowler JL, Wheeler AJ. Exploring an increased role for Australian community pharmacy in mental health professional service delivery: evaluation of the literature. J Ment Health. 2016; 25(6):550–9.
Crossref
24 Phan SV, VandenBerg AM. Financial impact of a pharmacist-managed clinic for long-acting injectable antipsychotics. Am J Health Syst Pharm. 2012;69(12):1014–5.
Crossref PubMed
25 Williams T, Purvis TL. Development of an outpatient pharmacist-managed clozapine clinic. Am J Health Syst Pharm. 2012;69(14):1192–5.
Crossref PubMed
26 Goldner EM, Jones W, Fang ML. Access to and waiting time for psychiatrist services in a Canadian urban area: a study in real time. Can J Psychiatry. 2011;56(8):474–80.
Crossref PubMed
Address correspondence to: Dr Sukhpreet Poonia, Lower Mainland Pharmacy Services, Fraser Health Authority, Langley Memorial Hospital, Marion Ward Pavilion, 22051 Fraser Highway, Langley BC V3A 4H4, email: Sukhpreet.poonia2@fraserhealth.ca
Competing interests: None declared.
Funding: None received.
Submitted: October 21, 2024
Accepted: April 9, 2025
Published: August 13, 2025
© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 3, 2025