Caitlin Olatunbosun, Kory Sloan, Laura Miskimins, Hazel Gabert, Rekha Jabbal, and Catherine BiggsTo cite: Olatunbosun C, Sloan K, Miskimins L, Gabert H, Jabbal R, Biggs C. Medication utilization at a provincial remand centre. Can J Hosp Pharm. 2025;78(3):e3766. doi: 10.4212/cjhp.3766
ABSTRACT
Background
Evaluation of medication utilization highlights health needs and facilitates rational drug use in a population. Data on medication utilization in correctional facilities are limited.
Objective
To describe the types and volumes of medications used at a provincial remand centre, by drug schedule and therapeutic classification.
Methods
In this retrospective review of medications used at the Edmonton Remand Centre over a 1-year period (September 2022 to August 2023), the data were analyzed descriptively. Data were compared by sex and age using the unpaired 2-sided t test and by medication type using the χ2 test.
Results
Of 8772 persons admitted to the remand centre during the study period, 6296 (71.8%) had medication orders. Of these, 5446 (86.5%) had orders for over-the-counter medications, 5591 (88.8%) for prescription medications, and 2513 (39.9%) for narcotics. Patients 40 years of age or younger had proportionally more orders for narcotic medications. The therapeutic classes with the highest proportions of patients were those for treating mental health problems, substance use disorder, pain, constipation, and infectious diseases.
Conclusions
Most patients in this corrections facility were receiving medications. Utilization trends specific to the corrections setting should be considered to support patient care.
Keywords: medication utilization, remand centre, medication, correctional health care, pharmacy
RÉSUMÉ
Contexte
L’évaluation de l’utilisation de médicaments fait ressortir les besoins en matière de santé et facilite l’utilisation rationnelle de médicaments au sein d’une population donnée. Les données portant sur l’utilisation de médicaments dans les établissements correctionnels sont limitées.
Objectif
Décrire les types et les volumes de médicaments utilisés dans un centre de détention provincial provisoire, selon l’annexe des médicaments et la classe thérapeutique.
Méthodologie
Dans cette revue rétrospective des médicaments utilisés au Centre de détention d’Edmonton sur une période d’un an (de septembre 2022 à août 2023), les données ont été analysées de manière descriptive. Les données ont été comparées selon le sexe et l’âge à l’aide du test t bilatéral non apparié, et selon le type de médicament avec le test du χ2.
Résultats
Sur les 8772 personnes admises au centre de détention provisoire durant la période de l’étude, 6296 (71,8 %) avaient des ordonnances de médicaments. Parmi celles-ci, 5446 (86,5 %) avaient des ordonnances pour des médicaments en vente libre, 5591 (88,8 %) pour des médicaments sur ordonnance et 2513 (39,9 %) pour des narcotiques. Les patients âgés de 40 ans ou moins avaient proportionnellement plus d’ordonnances pour des médicaments narcotiques. Les classes thérapeutiques regroupant les proportions les plus élevées de patients concernaient le traitement des problèmes de santé mentale, des troubles liés à l’utilisation de substances, de la douleur, de la constipation et des maladies infectieuses.
Conclusions
La plupart des patients dans cet établissement correctionnel recevaient des médicaments. Les tendances propres au milieu correctionnel quant à l’utilisation de médicaments devraient être prises en compte pour soutenir les soins aux patients.
Mots-clés: utilisation de médicaments, centre de détention provisoire, médication, soins de santé en milieu correctionnel, pharmacie
Individuals in correctional facilities have more health concerns than the general population.1 There are higher prevalences of infectious diseases and chronic illness, with overrepresentation of people who have been marginalized in society, have poor health, have untreated chronic illnesses, or have behaviours that pose a health risk.1 Given the vulnerability of these individuals and the characteristics of the environment, people in prison are at risk of numerous infectious diseases, including hepatitis B, hepatitis C, HIV, and tuberculosis.1 In addition, disease rates for other chronic diseases are elevated in this population relative to adults not in the corrections setting.1 The most common conditions reported in US prisons are respiratory, cardiovascular, and sexually transmitted infections.2 In the United Kingdom, 90% of prisoners have a mental illness, addiction, or personality disorder.1
Data from Canadian correctional facilities, though limited, point to similar trends, and the health status of inmates in Canada is poor, with higher rates of communicable diseases, mental illness, and substance use disorder (SUD).3 Infectious diseases are overrepresented among persons in corrections facilities, with higher prevalences of hepatitis C, HIV, and tuberculosis than in the general population.3–5 In a provincial remand centre in Alberta, there was a lifetime prevalence of mental disorders of 91.7%, compared with 43.7% in the general community, and a lifetime prevalence of SUD of 87.2%, compared with 39.6% in the community.3 Little is known about the prevalence of chronic diseases among people incarcerated in Canada, although limited evidence suggests that cardiovascular disease, diabetes, and asthma occur at higher-than-expected rates.3
It is unknown whether medication utilization trends by age and sex are similar between the general and incarcerated populations. To the authors’ knowledge, information about medication utilization in correctional facilities in Canada is limited to one study of a single day of medications prescribed for federally incarcerated women.6 In that study, the most common categories of medications were psychotropics (used by 42% of participants), nonsteroidal anti-inflammatory drugs (34%), peptic ulcer therapy (23%), asthma treatment (21%), and allergy treatment (18%).6 Other available data have been restricted to targeted drug classes,7–9 and no data on overall medication utilization are available for provincial correctional facilities in Canada. Provincial facilities house people for shorter sentences (less than 2 years), and those awaiting trial,10 which results in shorter stays than in federal facilities.
In this study, we describe medication utilization at a provincial remand centre, the Edmonton Remand Centre, in Edmonton, Alberta, in terms of the types and volumes of medications, with the goal of better understanding the health needs of this population.
This retrospective review used the provincial DOSE Database (Drug Optimization, Sustainability, and Evaluation), which included information for all persons housed in the Edmonton Remand Centre from September 1, 2022, to August 31, 2023. This facility houses 1500–1900 individuals, with an average stay of 28 days. A study period of 1 year was chosen to account for seasonal variations. All regimens (short-course, long-term, as-needed, any route) and types (over-the-counter or prescription) of medications were included in the analysis; repeat orders for the same medication for a given patient were counted only once. All medications used on site are entered into the facility’s pharmacy system. The DOSE database integrates data from pharmacy information systems in all settings into a single provincial dataset. The database is then used as the foundation for data-driven, evidence-based programs to manage drug budgets and address pharmacy-related analytics.
The data were analyzed using descriptive statistics. Medications were classified by type, according to the schedules of the National Association of Pharmacy Regulatory Authorities, where Schedule I refers to prescription medications, Schedule II refers to medications requiring professional intervention and possibly referral, and Schedule III refers to over-the counter medications.11 Any medications requiring pharmacist oversight (i.e., Schedules I and II) were deemed, for the purposes of this study, to be prescription medications. Prescription medications included controlled substances as defined by Canada’s Controlled Drugs and Substances Act12 (which has schedules distinct from those of NAPRA). Medications were also classified therapeutically, using the World Health Organization’s Anatomical Therapeutic Chemical (ATC) classification system.13
The proportion of patients with a prescribed medication in each class was controlled for repeat orders, but we did not account for a single patient having medications in similar classes (e.g., psycholeptics and psychoanaleptics). For the most frequently used categories, “high-use medications” were defined as the top 5 medications in the category or those used for more than 400 patients; for categories with lower use, “high-use medications” were defined as the top 2 medications in the category.
The data were analyzed descriptively using Excel spreadsheet software (Microsoft Corporation), and the MedCalc tool14 was used for comparisons. Comparisons based on sex and age used the unpaired 2-sided t test, and those based on medication type used the χ2 test. A p value less than 0.005 was considered significant.
This study received approval from the University of Alberta Ethics Review Board (Pro00134226).
From September 1, 2022, to August 31, 2023, a total of 8772 persons were admitted to the remand centre, of whom 7068 (80.6%) were men, and 6282 (71.6%) were 40 years of age or younger. Of those admitted, 6296 (71.8%) had medication orders, of whom 5110 (81.2%) were men and 4268 (67.8%) were 40 years of age or younger. Of the 6296 patients with medication orders, 3405 (54.1%) had 5 or more unique medications; the mean number of medications per patient was 6.0 (standard deviation 4.3), and the mean number of prescription medications was 4.2 (standard deviation 3.2). Of the total population admitted to remand, 3405 (38.8%) of the 8772 individuals had 5 or more unique medications.
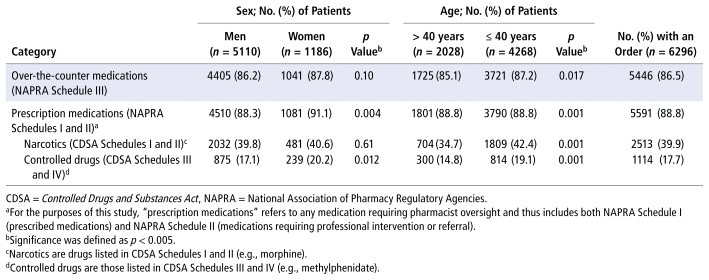
Of the 6296 patients taking medications, 5446 (86.5%) had orders for an over-the-counter medication and 5590 (88.8%) had orders for a prescription medication, with 2513 (39.9%) having an order for a narcotic medication. The proportion of patients with an order for a narcotic medication was higher among younger (≤ 40 years) than among older (> 40 years) individuals (Table 1).
TABLE 1 Categorization of Medications Used by Patients in a Remand Centre (n = 6296)

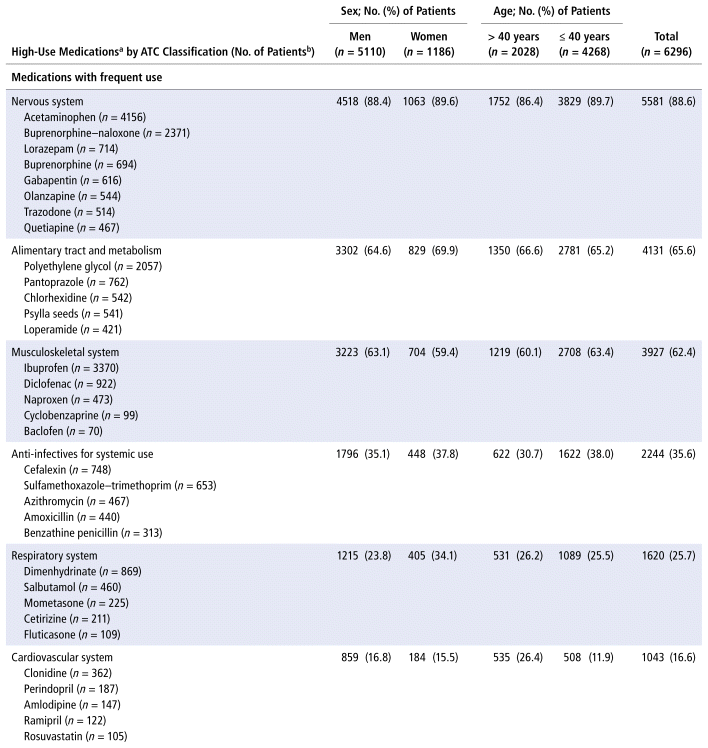
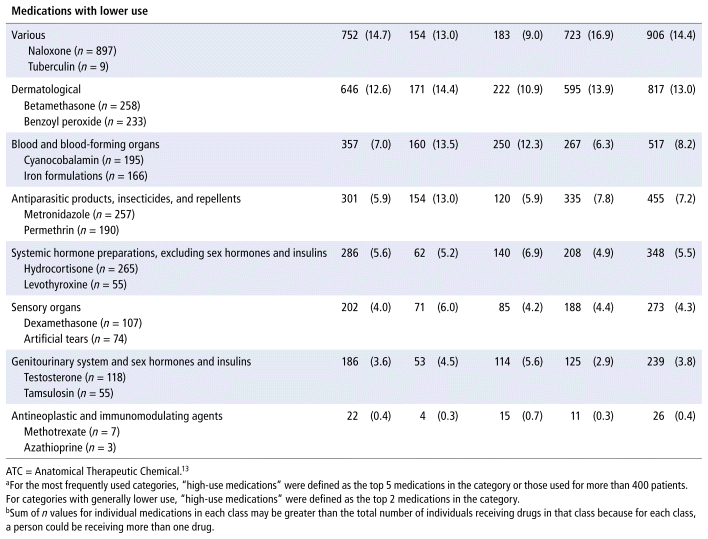
The ATC categories with the highest proportions of patients were nervous system (used by 88.6% of the study group), alimentary tract and metabolism (65.6%), musculoskeletal (62.4%), anti-infectives for systemic use (35.6%), respiratory system (25.7%), and cardiovascular system (16.6%). Medications ordered for the highest proportion of patients in each class, as described in Table 2, were those typically used for mental health, SUD, pain, constipation, and infections. The highest-use medications were acetaminophen, ibuprofen, buprenorphine–naloxone, and polyethylene glycol (Table 2).
TABLE 2 Number and Proportion of Patients Receiving Medications in Each Therapeutic Class, by Sex and Age
This study showed high medication utilization by people held in a provincial remand centre, with a significant proportion of the medications being prescription drugs involving the therapeutic classes of nervous system, alimentary tract and metabolism, musculoskeletal, and anti-infective medications. Most of the patients were receiving at least 1 prescription medication, with higher proportions of women and of people 40 years of age or younger having orders for prescription medications. These patterns were true for analyses by drug schedule and therapeutic class, with younger patients having greater use of nervous system medications, particularly buprenorphine–naloxone. This finding could be attributed to overdoses and opioid use disorder, which are primarily seen in men 30 to 39 years of age,15 and translates to age-related trends for relevant treatment in the corrections setting. Age- and sex-related differences were also seen for the less commonly used therapeutic classes. Although it was not surprising that women had more orders for blood-forming products and that use of cardiovascular medications was higher among older patients, it is unclear why utilization of respiratory and antiparasitic medications was higher among women than men.
This study was limited in terms of its generalizability, and was also limited by the constraints of a drug utilization study. Medication utilization depends on local patterns for prescribing, local public health initiatives for screening and treatment, and formulary compliance. In addition, medications may be used for indications outside of their listed therapeutic classification; for example, clonidine is classified in the ATC system as an antihypertensive but is commonly used for opioid withdrawal. However, it appears that off-label use occurred only in a minority of cases, and listing the most frequently used medications for each class allowed for an understanding of the primary medications used in each class. This study assessed only medication utilization, and data on diagnoses and clinical outcomes would be needed to assess whether patients were adequately treated while in the facility. Despite these limitations, the data highlight patterns of use that can be considered broadly when planning the deployment of pharmacy and other health resources in correctional facilities.
In this study, 63.7% (5591/8772) of all individuals in the facility had at least 1 prescription medication, which is higher than the general population in Canada, where 55% of adults aged 18 to 79 years used at least 1 prescription medication in the previous month (data for 2016–2019)16; however, differences in age and time period limit the comparison. In terms of utilization of multiple medications, our study population had a high proportion of patients (38.8% of all individuals) with 5 or more unique medications, whereas only 24% of people in the general population were receiving 3 or more medications in the period 2016–2019.16 In that same period, the most common prescription medications used in the general adult population in Canada were medications for blood pressure (16%), high cholesterol (12%), and mood disorders (10%),16 whereas the medications used most frequently at the provincial remand facility in the current study were for nervous system disorders (mental health and SUD), alimentary conditions, and infections.
Evaluating medication utilization provides insight into prescribing trends that can inform clinical and pharmacy practice to promote rational drug use and evidence-based medicine. More specifically, this study provides insights that can be used to develop health services in correctional facilities through appropriate resource allocation and program focus. These data support the ongoing need for addiction and mental health services, as well as primary care. The high number of chronic diseases indicated by the medication utilization patterns we observed represent an opportunity for involvement of allied health professionals and nursing-led protocols to improve the efficiency of care.
Patients in the correctional facility where this study took place had high utilization of prescription medications, regardless of sex or age, with large proportions of the population receiving medications that are typically prescribed for psychiatric conditions, SUDs, pain, constipation, and infectious diseases. Medication utilization trends in this facility differed from those of the general population, and these differences should be taken into consideration in the provision of patient care in correctional facilities.
1 Enggist S, Møller L, Galea G, Udesen C, editors. Prisons and health. World Health Organization; 2014 [cited 2024 Dec 3]. Available from: https://www.who.int/europe/publications/i/item/9789289050593
2 Bai JR, Befus M, Mukherjee DV, Lowy FD, Larson EL. Prevalence and predictors of chronic health conditions of inmates newly admitted to maximum security prisons. J Correct Health Care. 2015;21(3):255–64.
Crossref
3 Kouyoumdjian F, Schuler A, Matheson FI, Hwang SW. Health status of prisoners in Canada: narrative review. Can Fam Physician. 2016; 62(3):215–22.
PubMed PMC
4 Popovic N, Williams A, Périnet S, Campeau L, Yang Q, Zhang F, et al. National hepatitis C estimates: incidence, prevalence, undiagnosed proportion and treatment, Canada, 2019. Can Commun Dis Rep. 2022; 48(11/12):540–9.
Crossref
5 Estimates of HIV incidence, prevalence, and Canada’s progress on meeting the 90-90-90 HIV targets, 2020. Public Health Agency of Canada; 2022 [cited 2024 Dec 3]. Available from: https://www.canada.ca/en/public-health/services/publications/diseases-conditions/estimates-hiv-incidence-prevalence-canada-meeting-90-90-90-targets-2020.html
6 Langner N, Barton J, Mcdonagh D, Noel C, Bouchard F. Rates of prescribed medication use by women in prison. Forum Correct Res. 2002;14(2):10–4.
7 Kurz M, Dale LM, Min JE, Hongdilokkul N, Greiner L, Olley M, et al. Opioid agonist treatment uptake within provincial correctional facilities in British Columbia, Canada. Addiction. 2022;117(5):1353–62.
Crossref
8 Bozinoff N, DeBeck K, Milloy MJ, Nosova E, Fairbairn N, Wood E, et al. Utilization of opioid agonist therapy among incarcerated persons with opioid use disorder in Vancouver, Canada. Drug Alcohol Depend. 2018;193:42–7.
Crossref
9 Brown G. Prescription practices for psychotropic medications in the community and in prison populations: review of current literature. Res Rep R-382. Correctional Service of Canada; 2017 [cited 2024 Mar 17]. Available from: https://www.canada.ca/en/correctional-service/corporate/library/research/glance/382.html
10 Adult correctional and remand centres [webpage]. Government of Alberta; 2025 [cited 2025 Mar 17]. Available from: https://www.alberta.ca/adult-correctional-remand-centres
11 Drug scheduling in Canada. National Association of Pharmacy Regulatory Authorities; 2024 [cited 2024 Dec 3]. Available from: https://www.napra.ca/national-drug-schedules/drug-scheduling-in-canada/#:~:text=The%20NDS%20program%2C%20which%20consists,sale%20for%20each%20drug%20schedule
12 Controlled Drugs and Substances Act, S.C. 1996, c. 19 [cited 2024 Dec 3]. Available from: https://laws-lois.justice.gc.ca/eng/acts/c-38.8/
13 Collaborating Centre for Drug Statistics Methodology. ATC/DDD index 2024. World Health Organization; updated 2024 Jan 26 [cited 2024 Dec 3]. Available from: https://atcddd.fhi.no/atc_ddd_index/
14 Comparison of proportions calculator [online tool]. Version 23.1.7. MedCalc Software Ltd; [cited 2025 Mar 17]. Available from: https://www.medcalc.org/calc/comparison_of_proportions.php
15 Substance-related Overdose and Mortality Surveillance Task Group, on behalf of Council of Chief Medical Officers of Health. Opioid- and stimulant-related harms in Canada. Public Health Agency of Canada; 2024 [cited 2024 Dec 3]. Available from: https://health-infobase.canada.ca/substance-related-harms/opioids-stimulants/
16 Prescription medication use among Canadian adults, 2016 to 2019. Statistics Canada; 2021 [cited 2024 Dec 3]. Available from: https://www150.statcan.gc.ca/n1/daily-quotidien/210628/dq210628e-eng.htm
Address correspondence to: Caitlin Olatunbosun, Pharmacy Services, Alberta Health Services, 8440 112 Street NW, Room 0G1.24, Edmonton AB T6G 2B7, email: caitlin.olatunbosun@ahs.ca
Competing interests: Rekka Jabbal serves as Board Co-Chair for Provincial Correctional Health Services Calgary. No other competing interests were declared.
Funding: None received.
Submitted: December 20, 2024
Accepted: March 31, 2025
Published: July 9, 2025
© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 3, 2025