Catherine Biggs and Anne TruongTo cite: Biggs C, Truong A. Joy in work among hospital pharmacists. Can J Hosp Pharm. 2025;78(4):e3768. doi: 10.4212/cjhp.3768
ABSTRACT
Background
With the prevalence and severity of burnout among health care providers increasing after the COVID-19 pandemic, there have been calls to manage burnout with a more proactive approach: joy in work. Ample literature is available on burnout experienced by pharmacists, but not on their joy in work.
Objective
To build an understanding of hospital pharmacists’ perspectives on joy in work by determining how they defined joy and what they viewed as contributors and barriers to joy.
Methods
This study was conducted over 9 nonconsecutive weeks between December 2023 and March 2024. An anonymous electronic survey was used to capture information from pharmacists working in a provincial health authority in Alberta. Follow-up interviews were conducted with respondents who consented at the end of the survey.
Results
A total of 152 complete survey responses were collected (representing an estimated 17.7% response rate), and 9 interviews were held. Three themes representing contributors to joy were constructed: purpose, connection and belonging, and autonomy and agency. Two additional themes—systemic factors and large-scale changes—had both positive and negative impacts on joy. Barriers to joy were feeling undervalued, conflict, and feeling unsupported.
Conclusions
This study helps in understanding joy in work specifically among hospital pharmacists. Further research is needed to understand joy in work among pharmacists working outside of hospitals (e.g., community pharmacists) and to assess the efficacy of implementing strategies to improve joy within a pharmacy team.
KEYWORDS: hospital pharmacy, pharmacists, joy in work, job satisfaction, burnout
RÉSUMÉ
Contexte
Avec l’augmentation de la prévalence et de la sévérité de l’épuisement professionnel chez les prestataires de soins de santé après la pandémie de COVID-19, des appels ont été lancés pour adopter une approche plus proactive : la joie au travail. Une abondante littérature existe sur l’épuisement professionnel vécu par les pharmaciens, mais pas sur la joie qu’ils éprouvent au travail.
Objectif
Comprendre les points de vue des pharmaciens d’hôpitaux sur la joie au travail en déterminant comment ils définissent la joie et ce qu’ils considèrent comme des facteurs qui contribuent à la joie et qui y font obstacle.
Méthodologie
Cette étude a été menée sur 9 semaines non consécutives entre décembre 2023 et mars 2024. Un sondage électronique anonyme a été utilisé pour recueillir des informations auprès des pharmaciens travaillant au sein d’une autorité sanitaire provinciale en Alberta. Des entrevues de suivi ont été réalisées avec les répondants ayant donné leur consentement à la fin du sondage.
Résultats
Un total de 152 réponses complètes au sondage ont été recueillies (soit un taux de réponse estimé à 17,7 %) et 9 entretiens ont été réalisés. Trois thèmes représentant les facteurs contribuant à la joie au travail ont été dégagés : le sens du travail, les relations et le sentiment d’appartenance, ainsi que l’autonomie et le pouvoir d’action. Deux thèmes supplémentaires — les facteurs systémiques et les changements à grande échelle — influaient à la fois positivement et négativement la joie au travail. Les obstacles à la joie étaient le sentiment de ne pas être valorisé, les conflits et le sentiment d’un manque de soutien.
Conclusions
Cette étude permet de mieux comprendre la joie au travail, en particulier chez les pharmaciens d’hôpitaux. Des recherches supplémentaires sont nécessaires pour explorer la joie au travail chez les pharmaciens exerçant en dehors des hôpitaux (par exemple, les pharmaciens communautaires) et pour évaluer l’efficacité de la mise en œuvre de stratégies visant à améliorer la joie au sein d’une équipe de pharmacie.
Mots-clés: pharmacie hospitalière, pharmaciens, joie au travail, satisfaction professionnelle, épuisement professionnel
Health care professionals experienced burnout during the COVID-19 pandemic.1 The prevalence of severe burnout among health care professionals rose from 30% to 40% in spring 2020 to over 60% by fall 2020.1 Higher burnout rates led to lower-quality patient care, through higher health care system costs, greater personnel turnover, higher rates of depression and suicidal ideation in providers, and more medication errors.1–3
Focusing on joy in work is a proactive approach to managing burnout.2 Joy in work stems from “doing meaningful work”, “fostering and nurturing positive relationships with patients and other healthcare team members”, and “having adequate resources to meet work demands.”4 In 2017, the Institute for Healthcare Improvement (IHI) published a 4-step Framework for Improving Joy in Work for leaders and managers to follow.4 In the field of nursing, use of the IHI framework to educate unit leaders led to an 18% decrease in mean anticipated turnover scores.5 Another research team implemented the first step of the IHI framework, asking employees “What matters to you?” and found that employees felt constantly expected to respond to emails outside of work hours.6 The policy on handling email was changed, which led to 80% of employees reporting they felt more respect for their personal time.6
For pharmacists, there is a large body of literature on burnout, but nothing on joy in work.7–9
This study aimed to build an understanding of hospital pharmacists’ perspectives on joy in work by asking them to define joy and to identify the contributors and barriers to joy.
Pharmacists working for a provincial health authority in Alberta were the focus of the study. Data were gathered between December 11, 2023, and March 9, 2024, by means of an anonymous survey administered through REDCap (Research Electronic Data Capture) software. The survey contained 6 multiple-choice, multi-select, and open-ended questions.
Pharmacists who had been in practice for less than 6 months were excluded by means of an initial screening question. Pharmacists who did not have an Alberta Health Services email address were excluded from participating due to organizational logistics and time constraints.
After completing the survey, respondents could indicate their willingness to participate in a 1-hour semistructured interview. Verbal consent was obtained before proceeding. Interviews were transcribed using Microsoft Teams software. Interview participants had up to 14 days after their interview to withdraw from the study.
The co-investigator (A.T.) used familiarization and inductive methods with open coding to construct themes from the open-ended survey questions, interview transcripts, and field notes. Ambiguities were discussed between the 2 investigators to obtain consensus. The study was reviewed and approved by the University of Alberta’s Ethics Review Board.
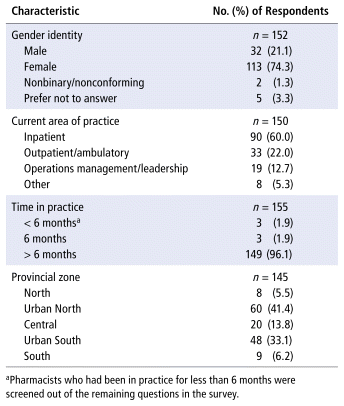
According to the health authority, approximately 858 hospital pharmacists were eligible to participate. A total of 152 survey responses were received, for an estimated response rate of 17.7%. Most respondents were women who had been in practice for more than 6 months (Table 1). Of the 152 respondents, 22 expressed interest in an interview, and 9 interviews were conducted, at which point content saturation was achieved. The 9 interview participants consisted of 6 women, 2 men, and 1 participant who preferred not to reveal their gender identity. None of the interview participants withdrew after completion of the interview.
TABLE 1 Demographic Characteristics of Survey Respondents

In the multiple choice and multi-select survey questions, participants reported that the following activities brought them joy: interpersonal activities (interacting with patients, pharmacy team members, or other members of the health care team; working within an interdisciplinary team) and activities that strongly relied on pharmacists’ expertise and knowledge (making therapeutic recommendations, practising to full scope). Work activities that participants found mundane or dull and that detracted from joy were performing administrative tasks, troubleshooting the provincial clinical information system, and attending meetings.
A definition of joy was constructed, and 5 themes were formed from responses to the open-ended survey questions and interview responses. Three of these themes contributed to creating and feeling joy: purpose, connection and belonging, and autonomy and agency. The other 2 themes—systemic factors and large-scale changes—had both positive and negative effects.
The definition of joy varied, ranging from an emotion synonymous with general happiness to something very profound, even spiritual. Commonalities were that joy is positive, related to happiness, contentment, fulfilment, satisfaction, and peace. Some defined joy as the absence of negative feelings like fear, dread, frustration, and stress. Sources of joy were internal (from oneself) or external (from other people or one’s surroundings).
Feeling happiness as a result of satisfaction, something well done. More intentional and broader than happiness alone. More sustained. (Participant 150)
Joy is [the] warm fuzzy feeling of knowing that your work has a positive impact on others. (Participant 8)
Feeling fulfilled at the end of each day, knowing my family is safe and healthy, and people and patients from work benefited from my existence. (Participant 124)
Lastly, joy was described as static (independent of external factors) or fluctuant (dependent on external factors).
The amount of joy at work for me depends a lot on my interactions with other team members, ... interactions with my patients, [and] having adequate resources for the task at hand. (Participant 108)
[Joy is] the ongoing internal feeling of pleasure, satisfaction, contentment, peace, [and] confidence that is not dependent or determined by external factors. (Participant 118)
Purpose encompassed having a positive impact, feeling recognized, and doing meaningful work. Having a positive impact on patients, colleagues, and students or contributing to system-level change by using their expertise and knowledge as pharmacists made participants’ work meaningful and satisfying.
What makes my work meaningful [is] patient interactions that give positive results. For patients and families to feel supported and hopefully ... leave my care better than they came into it. ... It’s to make my little world a better place. (Participant 50)
Being a clinical pharmacist on a multidisciplinary team gives me an opportunity to advocate for patients, educate other health care providers about potential barriers to care, and help with troubleshooting so that patients can successfully navigate the health care system. It makes me proud to forge respectful, trusting relationships with both clients and team members. (Participant 71)
Recognition and appreciation, especially from colleagues and patients, made participants’ work satisfying. Expressions of gratitude from colleagues reinforced participants’ value on a team, while gratitude from patients and families validated that a participant’s work made a difference in their lives.
The best thing is when a patient tells me I have made them feel better or made a difference in their lives. There is nothing better! (Participant 227)
Even just a little comment from a patient or family [like] “That was clear. Thank you very much” or “I really appreciate the Med schedule.” Things ... we do automatically as part of our process, [those comments are] a constant reminder that ... this is a life-changing experience for a patient. Being part of that journey for them, I think it’s very meaningful. (Participant 100)
When asked to describe working at their best, participants depicted work that aligned with their values. Examples of these values included providing care to their perceived best standard or effort, using most of their time in a day to directly interact with patients, and doing engaging work.
... I have adequate time to do a thorough job reviewing a patient, making recommendations, and feeling ... sure that I didn’t miss something. ... If I’m too overloaded with work, ... I feel like I’m doing less quality work and that doesn’t reflect [the work] I like to produce. (Participant 8)
Connection and belonging encompassed interpersonal relationships, supporting others, and feeling cared for. Bonds forged with colleagues and patients were very meaningful to participants.
I think the most meaningful part is direct interaction with patients because I work in a chronic disease clinic. We ... get to know our patients and meet them from the time of their diagnosis, which can be quite traumatic and emotional. ... Seeing them thrive in the weeks or months or years to come is really meaningful. (Participant 16)
… in hospital, you don’t get that longitudinal view with your patients, but you do ... with your colleagues. ... You ... develop relationships where you can collaborate with your fellow pharmacist, the nurses on your teams, [and] the physicians. ... I find that very meaningful to have ... good people to learn from and to bounce ideas off of every day. (Participant 8)
For participants to build positive connections, they felt their work environment needed to be psychologically safe—where they could be themselves and share ideas without fear of judgment or punishment. In a psychologically safe space, participants could voice concerns and be vulnerable in front of others, which fosters trust and camaraderie.
I can be collaborative with my colleagues and not feel judged or ridiculed for not knowing something. ... That adds to mental health in the workplace—the idea that I can trust my colleagues, or I know that they’ll have my back and ... I have theirs too. (Participant 22)
I have a very supportive workplace. ... I feel completely safe. My opinions are valued. (Participant 57)
Participants described feeling seen as a person rather than an employee when they were shown support and care. Working in a kind, caring environment with a strong support network helped participants to overcome challenges.
That [time] was very difficult [to go through] and I was very supported by [my colleagues] and the director. ... They were always reaching out asking if I was okay. (Participant 57)
A supportive manager has made a world of difference. I feel [cared] for as a person, and my professional and personal goals feel achievable. (Participant 102)
Autonomy and agency involved participants’ ability to have flexibility. Trust and confidence from colleagues and managers enabled participants to feel self-efficacious and respected as an equal. Participants felt they had adequate autonomy when they could implement recommendations, work independently, and practise to full scope.
[I appreciate] a manager who has your back and gives you support or advice when it is needed but also the freedom to complete your work. (Participant 68)
[I feel supported by] a team that allows me to practice independently yet [provides] easy routes of communication if I have questions. [I feel supported by the] encouragement to practice at full scope. (Participant 95)
Managerial support was vital to uphold participants’ autonomy, as managers control systemic factors (i.e., resource provision, task delegation, role clarity). Participants appreciated managers who listened, advocated for them, and actively supported them.
I had [solo] shifts coming up ... and I [felt that] I didn’t know the process [or] the team well enough to really do a good job. ... I said [to my boss], “Hey, I think I could use some more training days.” ... “No question”, she said, “Yeah, sure. We’ll figure it out.” That took a huge weight off the shoulders. ... I felt my issues were heard and there was some action about it. (Participant 11)
The times I’ve felt really supported is when my manager sticks up for me. (Participant 58)
Having agency made work feel like a part of participants’ lives, rather than their lives revolving around work. When participants had flexibility, especially with management, they could prioritize their personal lives over work when needed. This helped preserve work–life balance.
The support that I appreciate the most is from supervisors or managers who understand ... when you have to really juggle things. I feel [supported] when [I] have a little bit of flexibility ... in timing or in scheduling. ... It would be a lot more difficult if that was not the case because we all struggle to ... balance family life and work life. (Participant 100)
[I appreciate] being supported to take vacation when I need to, instead of feeling like I need to compete for time off. (Participant 236)
Systemic factors, like job stability, compensation, work resources (e.g., mental health supports, staffing, space), and patient resources (e.g., social supports, care access, medication coverage) had both positive and negative effects on joy.
[Stressors at work are] constantly changing schedules, scopes, ... uncertainty with job stability (temporary positions) [and the] patient care environment (under-staffing and over capacity). (Participant 148)
These factors demonstrate the interconnectedness of the themes and show that unstable funding combined with increased demand can cause collective burnout among staff, leading to a higher-stress environment (affecting connection and belonging) and poorer quality of care (affecting purpose).
A main stressor for me ... is the number of off service patients that require pharmacy intervention in addition to my current workload. I feel burnt out due to the amount asked of us with the current level of staffing. (Participant 37)
A lot of [patients] are in crisis with mental health issues and ... addictions. ... There’s ... a feeling of hopelessness or helplessness not being able to connect people to the services that they desperately need. ... I can do the best job I can as a pharmacist, but not being able to really help them with their basic needs and mental health is quite discouraging right now. (Participant 16)
Finally, large-scale changes, like the provincial transition to a new electronic health record and restructuring of the health care system, affect joy among health care providers. Despite reporting some positive effects of such transitions, most participants found change stressful, reporting diminished morale, fatigue, and frustration.
[The new electronic health record] and [it’s caused] a complete flip of the workflow. ... There’s never enough hours in the day to ... do my best for my patients, and I find it frustrating. (Participant 50)
... despite our team being excellent and solid, the uncertainty around the future of our health care system is affecting how I feel about my work. (Participant 16)
Barriers were described as the lack, absence, or opposite of the themes that contributed to joy. Feeling undervalued and having to complete tasks that are not connected to direct patient care made pharmacists feel unsupported.
I think having team members that don’t value the role of a pharmacist or [who] see pharmacists as there to provide clerical support greatly [diminishes] the joy I feel when I am [providing] clinical [care]. (Participant 28)
Reviewing orders for another hospital has increased the volume of work that I need to do when verifying orders on weekends and on evenings, and when I notice orders are sloppy and I need to miss my breaks, I question whether management realizes the decisions they made may be wrong. (Participant 52)
Feeling unsupported by management, colleagues, or team members also contributed to lack of joy at work.
I do not feel very supported at work. ... I feel health care in this province is not appreciated ... and it is highly disconcerting. ... Pharmacists always seem to be on the “outside” of the clinical team, rather than being fully accepted as part of the team (there are exceptions) and it often makes it difficult to give input into the running of the clinical area. (Participant 227)
Pharmacists also described lack of trust and feeling micromanaged as barriers to fully engaging at work. Systemic changes that negatively affected work–life balance increased stress for participants.
Night shifts are a huge stressor. The rotating day and night shifts have impacted my morale at work because it has an impact on my sleep and mood. It has caused me to question if I want to continue in acute care practice after being here for more than a decade. (Participant 234)
During the pandemic, pharmacists experienced significant burnout and stress due to multiple factors. There is extensive literature describing burnout and moral distress experienced by pharmacists and other health care providers but few studies describing why individuals come to work. Here, pharmacists were asked to share what joy was to them, what created joy, and what detracted from joy while at work.
From the survey and interview data collected, a definition of joy was developed and themes were constructed. Pharmacists did not have a single, consistent definition of joy, although there were common elements, such as contentment and happiness or the absence of negative feelings. Interestingly, joy had both internal and external sources.
The constructed themes that positively influenced joy—purpose, connection and belonging, and autonomy and agency—were contributors to meaningful and satisfying work. Pharmacists discussed making a positive impact and receiving recognition as factors influencing purposeful work. Working to better patients’ lives and being appreciated by patients were examples provided. Developing relationships with patients and colleagues contributed to a sense of belonging at work. Pharmacists described aspects of psychological safety as contributing to resilience. Managerial support affected autonomy and agency. Managers can provide some flexibility to schedules and can support employees during times of conflict, both of which promoted self-efficacy.
Two themes had positive and negative impacts on joy. Certain systemic factors, such as lack of funding, were often mentioned as stressors. To meet increased demands without adequate funding for the required resources, participants felt pressured to work longer hours or miss breaks, which affected their autonomy and agency. Large-scale changes also affected pharmacists positively and negatively. These changes can improve efficiency in the long term, but implementation and adaptation can cause increased fatigue and frustration.
To the authors’ knowledge, this study is the first to focus on joy in work among pharmacists specifically; as such, there exist multiple opportunities for future research. Examples include evaluating joy in work for pharmacists employed outside hospitals (e.g., community pharmacists) or observing the effects of implementing the IHI framework on a pharmacy team. By sharing perspectives on joy in work among hospital pharmacists, this study serves as a building block to shift the focus from burnout to empowering joy.
1 Maunder RG, Heeney ND, Strudwick G, Shin HD, O’Neill B, Young N, et al.; Ontario COVID-19 Science Advisory Table and Mental Health Working Group. Burnout in hospital-based healthcare workers during COVID-19 [Science Brief]. Ontario COVID-19 Science Advisory Table; 2021 Oct 7 [cited 2023 Jul 29];2(46). Available from: https://doi.org/10.47326/ocsat.2021.02.46.1.0
2 Holliday M, Solomon G, Springer K, Anim M, Aron D, Hargraves D. Avoiding burnout by increasing joy in work: opportunities for the healthcare system. Ohio Cardiovascular and Diabetes Health Collaborative; 2021 Nov 30 [cited 2023 Jul 25]. Available from: https://cardi-oh.org/assets/best-practices/effective-teams/Cardi-OH-Avoiding-Burnout-by-Increasing-Joy-in-Work-Opportunities-for-the-Healthcare-System.pdf
3 Shanafelt T, Goh J, Sinsky C. The business case for investing in physician well-being. JAMA Intern Med. 2017;177(23):1826–32.
Crossref PubMed
4 Perlo J, Balik B, Swensen S, Kabnecell A, Landsman J, Feeley D. IHI framework for improving joy in work [white paper]. Institute for Healthcare Improvement; 2017 [cited 2023 Jul 25]. Available from: https://www.ihi.org/resources/Pages/IHIWhitePapers/Framework-Improving-Joy-in-Work.aspx
5 Reid A. Implementing IHI joy in work framework to decrease turnover among unit leaders. Doctor of Nursing Practice project 143. University of San Francisco; 2018 [cited 2023 Jul 25]. Available from: https://repository.usfca.edu/dnp/143
6 Chunta KS. New nurse leaders: creating a work-life balance and finding joy in work. J Radiol Nurs. 2020;39(2):86–8.
Crossref
7 Blue CL, Gould ON, Clarke C, Naylor H, MacKenzie M, Burgess S, et al. Burnout among hospital pharmacists in Canada: a cross-sectional analysis. Can J Hosp Pharm. 2022;75(4):326–34.
Crossref PubMed PMC
8 Watson KE, Schindel TJ, Chan JCH, Tsuyuki RT, Al Hamarneh YN. A photovoice study on community pharmacists’ roles and lived experiences during the COVID-19 pandemic. Res Social Adm Pharm. 2023;19(6):944–55.
Crossref PubMed PMC
9 Zahoor Z, Papadopoulos A, Nowrouzi-Kia B, Ibrahim P, Tadrous M, Gohar B. Behind the counter: exploring pharmacists’ stressors and lessons learned during the pandemic in Ontario, Canada. Health Serv Insights. 2023;16. doi:10.1177/11786329231169937
Crossref
Address correspondence to: Catherine Biggs, c/o Transitional Care Centre, Alberta Health Services, 18415 127 Street NW, Edmonton AB T6V 1B1, email: Catherine.biggs@ahs.ca
Competing interests: None declared.
Funding: This study was supported by Alberta Health Services, through its support of the Alberta Pharmacy Practice Residency Program.
Submitted: January 2, 2025
Accepted: May 12, 2025
Published: October 8, 2025
© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 4, 2025