Lama H Nazer, Naheel Said, Wedad Awad, Asma Kharabsheh, Musab Smadi, and Saad JaddouaTo cite: Nazer LH, Said N, Awad W, Kharabsheh A, Smadi M, Jaddoua S. An innovative approach to interdisciplinary training: a pharmacy resident’s day with a critical care nurse. Can J Hosp Pharm. 2025;78(2):e3780. doi: 10.4212/cjhp.3780
Nurses play a critical role in pharmaceutical care, extending beyond medication administration.1 This role becomes even more important in critical care settings, where patients are in an unstable condition and often receive at least twice as many medications as patients on general medical wards.2 The intersection of nurses’ and pharmacists’ roles in medication management, combined with the complexities and urgencies of managing the care of critically ill patients, necessitates close collaboration between these professions to ensure optimal pharmaceutical care and safe medication management.3,4
During the critical care learning experience for postgraduate year 1 (PGY-1) pharmacy residents, preceptors provide extensive teaching on medication management for critically ill patients, emphasizing key aspects relevant to this patient population. However, as preceptors, we observed that while our pharmacy residents developed a strong understanding of the conceptual approach to medication administration and various bedside assessment measures, they lacked a clear grasp of the practical aspects and challenges associated with these nurse-driven components of patient care. To address this gap, we implemented an educational activity in which pharmacy residents spend a full day at the bedside with a critical care nurse, an experience that allows them to gain first-hand experience and a deeper appreciation of the complexities involved in caring for critically ill patients, particularly in terms of medication management.
Here, we describe an interprofessional educational program that was implemented as part of the requirements for PGY-1 pharmacy residents and added to the critical care learning experience. We describe the goals and objectives of the program, the activities involved, and our experience in implementing the learning activity. The program involves having each pharmacy resident shadow a critical care nurse and actively engage in nurse-related patient care activities. The main goals of this program are for residents to gain a deeper understanding of the nurse’s role in critical care and to enhance their knowledge and skills in bedside patient monitoring and drug administration, both of which are necessary for optimizing medication management.
The program is conducted at King Hussein Cancer Center, a 352-bed comprehensive teaching cancer centre in Amman, Jordan. The hospital has 2 medical/surgical intensive care units (ICUs), with a total of 21 beds, and a full-time critical care clinical pharmacist, who is an active member of the multidisciplinary team, contributing to all aspects of patients’ medication management. The hospital has a PGY-1 pharmacy residency program, which has been accredited by the American Society of Health-System Pharmacists since 2019. The ICU learning experience consists of 6 weeks in the adult ICUs.
The program involves having each pharmacy resident spend a full day with a registered nurse in the ICU. The Nursing Day occurs 2–3 weeks after the start of the ICU rotation. At least 1 or 2 days before the Nursing Day, the preceptor meets with the resident to explain the goals and expectations of this activity. In addition, the nursing supervisor meets with the resident to review the main nursing practice policies, such as those related to dress code and infection control.
On the Nursing Day, the pharmacy resident’s schedule mirrors that of the assigned nurse, encompassing a 12-hour shift, starting with patient handover rounds from the night nurse and concluding with handover to the incoming night nurse. On this day, the resident shadows the assigned nurse and performs various patient-related nursing tasks, under the supervision of the nurse preceptor and within the boundaries of pharmacy and nursing regulations. To become fully immersed in the nursing role, the resident is restricted from accessing any pharmacy areas or performing any pharmacy-related activities.
During the Nursing Day, there are 3 main learning objectives:
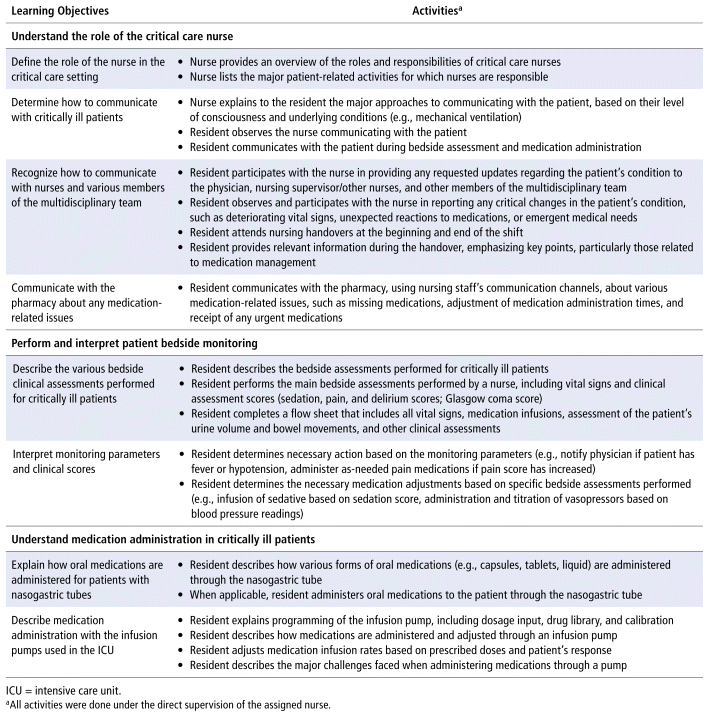
The following sections briefly discuss the 3 learning objectives; the activities associated with each objective are listed in Table 1.
TABLE 1 Learning Objectives and Related Activities on Nursing Day

In the intense environment of an ICU, nurses are not only caregivers, but also decision-makers, coordinating complex care and implementing life-saving interventions. Recognizing nurses’ pivotal role allows other health care professionals, including pharmacists, to understand their needs and the unique challenges they face.
Throughout their work, nurses are expected to communicate clearly and efficiently with their patients, as well as the multidisciplinary team, to convey critical patient information, discuss treatment plans, and respond promptly to patients’ changing conditions. During the Nursing Day, the pharmacy resident observes the nurse using various forms of communication with the patient and other providers. In addition, the resident takes on the responsibility of contacting the pharmacy and addressing any medication-related issues, using the nurse’s usual communication channels and procedures. By performing such tasks, residents are expected to gain a better understanding of nurses’ needs and the issues they encounter when they contact the pharmacy.
The clinical condition of a critically ill patient is inherently unstable, which necessitates close monitoring. Furthermore, to tailor medications to the patient’s needs and account for ongoing changes, pharmacists rely heavily on bedside assessments performed by nurses, such as determination of sedation and pain scores, evaluation of mental status, and measurement of vital signs and urine output. These assessments inform decisions regarding the initiation, adjustment, or discontinuation of medications, as well as the appropriate dosing, route of administration, fluid type, and volume for IV medications.
On the Nursing Day, the pharmacy resident conducts various clinical assessments for the assigned patient and is responsible for completing a nursing flow sheet for the day. Direct involvement in these assessments helps the resident understand how they are performed at the bedside and, more importantly, how they can be effectively interpreted to optimize medication therapy. This experience augments what is covered by the pharmacy preceptor throughout the ICU rotation to meet the required competencies for this learning experience.
As pharmacists, our primary responsibility is to ensure the safe and effective use of medications during all steps of the medication management cycle. Although our role is critical to medication administration, our involvement and contributions are significantly reduced after the medication is prepared and dispensed.
For critically ill patients, the administration of multiple medications by the IV route presents complexities, particularly for patients requiring multiple infusions but for whom IV access is limited. Similarly, there can be complexities for administration of oral medications to patients with nasogastric tubes—for example, tablets must be crushed or capsules opened—which may present challenges and limitations in certain situations. Pharmacists should understand all of these complexities to ensure safe and effective medication management.
The Nursing Day program was added to the critical care learning experience about 7 years ago, and to date a total of 11 pharmacy residents have completed the experience. The knowledge gained from the resident’s Nursing Day augments what is taught throughout the critical care rotation, reinforcing key concepts and practical applications. We have found this activity to be feasible, and both residents and nurses have described the experience in positive terms.
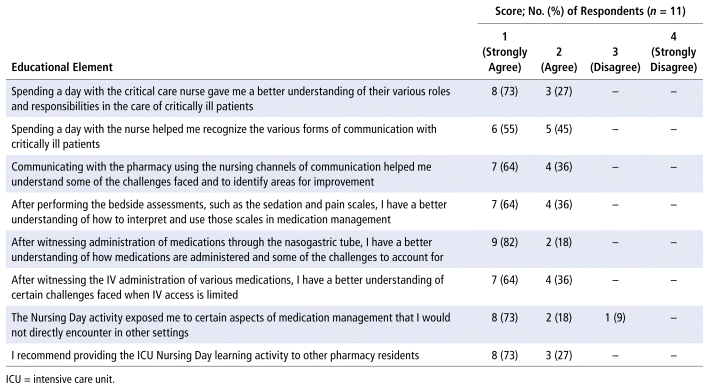
We conducted a survey of all residents who have participated in the Nursing Day to evaluate their perceptions about the impact and value of the program. The survey questions and results are outlined in Table 2. The majority of pharmacy residents agreed that the Nursing Day exposed them to aspects of medication management that they would not encounter in other settings, and all residents agreed with continuing to offer the Nursing Day experience to other pharmacy residents.
TABLE 2 Residents’ Perceptions of the ICU Nursing Day Learning Activity
Over the years, we have refined the program to enhance its effectiveness in achieving the intended outcomes. In the first year, we defined the main learning objectives but did not specify the corresponding activities. Subsequently, we have developed a set of structured learning activities aligned with each objective, to ensure completeness and consistency. In certain cases, we encountered challenges in meeting all elements of the learning objectives, particularly when our patient census was low or when the assigned patients did not have certain characteristics needed to meet the learning objectives. In these situations, we have asked the nurses to verbally explain procedures or scenarios that residents did not encounter. For future Nursing Days, we plan to collaborate with the nursing supervisor to schedule this activity at times when patient cases align with the predefined learning objectives and activities.
Over the years, we have also adjusted our planning for Nursing Day, so that it occurs earlier in the residents’ learning experience. This allows us to better accommodate pharmacy and nursing commitments, such as accreditation, training of new nurses, patient census, availability of nurse preceptors, and other logistic considerations.
Given that this is a relatively new program, with only 1 or 2 pharmacy residents participating each year, assessment of the activity has been limited to post-activity debriefing and the residents’ survey (Table 2). As we expand the program, we plan to implement structured pre- and post-activity surveys and/or focus groups to assess impacts and identify areas for improvement. We will also evaluate the feasibility of integrating this program into the orientation for new pharmacists, given that all of our pharmacists work on medication orders for critically ill patients and interact with critical care nurses both after-hours and on weekends.
1 Diles T, Heczkova J, Tziaferi S, Helgesen AK, Grøndahl VA, Van Rompaey B, et al. Nurses and pharmaceutical care: interprofessional, evidence-based working to improve patient care and outcomes. Int J Environ Res Public Health. 2021;18(11):5973.
Crossref
2 Moyen E, Camiré E, Stelfox HT. Clinical review: medication errors in critical care. Crit Care. 2008;12(2):208.
Crossref PubMed PMC
3 Morales Castro D, Dresser L, Granton J, Fan E. Pharmacokinetic alterations associated with critical illness. Clin Pharmacokinet. 2023; 62(2):209–20.
Crossref PubMed PMC
4 Jackson M, Cairns T. Care of the critically ill patient. Surgery (Oxf). 2021;39(1):29–36.
Crossref PubMed PMC
Address correspondence to: Dr Lama Nazer, Department of Pharmacy, King Hussein Cancer Center, Queen Rania Street, Amman, Jordan, email: lnazer@khcc.jo
Competing interests: None declared.
Funding: None received.
Acknowledgements: The authors sincerely appreciate the support of nursing administration for this educational activity and are deeply grateful to all the nurses who were involved with this program for their commitment, their team spirit, and their passion to teach.
Submitted: January 21, 2025
Accepted: March 21, 2025
Published: June 11, 2025
© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 2, 2025