Samantha Taylor, Caitlin Chew, Richard S Slavik, Olavo Fernandes, and Sean K GormanTo cite: Taylor S, Chew C, Slavik RS, Fernandes O, Gorman SK. Characteristics and factors influencing clinical pharmacy services in small hospitals in British Columbia: a theory-informed survey. Can J Hosp Pharm. 2025;78(4):e3787. doi: 10.4212/cjhp.3787
ABSTRACT
Background
Most hospitals in British Columbia have fewer than 200 beds, yet the clinical pharmacy services provided and factors influencing their delivery in this context are unknown.
Objectives
To describe on-site clinical pharmacy services and associated contextual barriers and enablers in small BC hospitals.
Methods
Between January and April 2022, an internet-based survey questionnaire was deployed to all pharmacy licence holders at BC hospitals with fewer than 200 beds (n = 23 licence holders representing 58 hospitals). Site characteristics, clinical activities, and barriers to and enablers of clinical pharmacy services (according to the Consolidated Framework for Implementation Research [CFIR]), as well as free-text responses, were captured.
Results
Of the 23 licence holders invited to participate, 18 (78%) responded, representing 37 (64%) of the small hospitals. Provision of clinical pharmacy services was reported at 27 (73%) of the 37 hospitals. Resolution of drug therapy problems and patient education were delivered at all of these hospitals. Conversely, the comprehensive patient care bundle and discharge medication reconciliation were never performed at 15 (56%) and 11 (41%), respectively, of these 27 hospitals. Of the 9 CFIR barriers, insufficient external networking and insufficient resources were reported by 17 (94%) and 16 (89%), respectively, of the 18 respondents. Funding and staffing barriers were reported, using free text, by 14 (78%) and 13 (72%), respectively, of the 18 respondents. Of the 21 CFIR enablers, the following 5 were reported by all respondents: agreement that clinical services are supported by adequate evidence, that such services will improve quality, that they will meet patient needs, that they will satisfy patients, and that a strong need exists for these services.
Conclusions
On-site clinical pharmacy services were delivered at most small BC hospitals; however, opportunities exist to expand clinical services. Pharmacy leaders should implement change strategies that overcome contextual barriers and enhance enablers.
KEYWORDS: small hospital, clinical pharmacy, clinical pharmacy key performance indicators, barriers and enablers, implementation science
RÉSUMÉ
Contexte
La plupart des hôpitaux de la Colombie-Britannique comptent moins de 200 lits, mais on ne sait pas quels sont les services de pharmacie clinique qui y sont offerts ni les facteurs influençant leur prestation dans ce contexte.
Objectifs
Décrire les services de pharmacie clinique sur place ainsi que les obstacles et les éléments facilitateurs contextuels associés dans les petits hôpitaux de la Colombie-Britannique.
Méthodologie
Entre janvier et avril 2022, un questionnaire en ligne a été envoyé à tous les titulaires d’une permis d’exercice en pharmacie dans les hôpitaux de la Colombie-Britannique comptant moins de 200 lits (n = 23 titulaires représentant 58 hôpitaux). Les caractéristiques des sites, les activités cliniques ainsi que les obstacles aux services de pharmacie clinique et les éléments facilitant ceux-ci (selon le Consolidated Framework for Implementation Research [CFIR], ou Cadre consolidé pour la recherche sur la mise en œuvre, en français), ainsi que des réponses libres, ont été recueillies.
Résultats
Sur les 23 titulaires de permis invités à participer, 18 (78 %) ont répondu, soit 37 des petits hôpitaux (64 %). Des services de pharmacie clinique ont été rapportés dans 27 des 37 hôpitaux (73 %). Tous les hôpitaux assuraient une résolution des problèmes liés à la pharmacothérapie et l’éducation des patients. En revanche, la gamme de soins complets aux patients et le bilan comparatif des médicaments au moment du congé n’ont jamais été offerts dans 15 (56 %) et 11 (41 %), respectivement, des 27 hôpitaux ayant déclaré offrir des services de pharmacie clinique. Parmi les 9 obstacles du CFIR, l’insuffisance du réseau externe et des ressources a été signalée par respectivement 17 (94 %) et 16 (89 %) des 18 répondants. Les obstacles liés au financement et au personnel ont été rapportés au moyen des réponses libres par 14 (78 %) et 13 (72 %) des 18 répondants. Parmi les 21 éléments facilitateurs du CFIR, les 5 suivants ont été rapportés par tous les répondants, qui s’accordent sur le fait que ces services cliniques : sont soutenus par des éléments probants adéquats; amélioreront la qualité; répondront aux besoins des patients; donneront satisfaction aux patients; répondent à un besoin important.
Conclusions
Des services de pharmacie clinique étaient offerts dans la plupart des petits hôpitaux de la Colombie-Britannique; toutefois, il y a des occasions de les élargir. Les leaders en pharmacie devraient mettre en place des stratégies de changement qui surmontent les obstacles contextuels et renforcent les éléments facilitateurs.
Mots-clés: petits hôpitaux, pharmacie clinique, indicateurs clés de performance en pharmacie clinique, obstacles et éléments facilitateurs, science de la mise en œuvre
Small hospitals are defined by the Canadian Institute for Health Information as facilities with fewer than 200 beds.1 Hospitals of this size are prevalent throughout Canada and in British Columbia, representing 77% and 70% of all hospitals, respectively.1,2 Although small hospitals face similar challenges in ensuring medication quality and safety as larger hospitals, they often have fewer resources available to address these issues.3,4 Small hospitals often have greater difficulty sustaining the required workforce, rely more on support from locum medical staff, and have access to fewer specialist services compared to their larger counterparts.5
Hospital-based clinical pharmacy services improve patient outcomes, patient experience, and economic measures.6–8 However, the evidence base describing these positive impacts has been derived primarily from hospital settings with 200 or more beds. Little is known about the clinical pharmacy services provided in small hospital settings, and there is a dearth of information describing barriers and enablers to delivering services in this context.
Clinical pharmacy key performance indicator (cpKPI) activities aim to “improve quality of care and advance clinical pharmacy practice, advance practice toward desired evidence-informed patient outcomes, define minimum standards and permit benchmarking within and between organizations, and elevate professional accountability and transparency”.9 These activities may be challenging to provide in the small hospital context.3,4 The 2020/21 Canadian Society of Hospital Pharmacists (now the Canadian Society of Healthcare-Systems Pharmacy) Hospital Pharmacy in Canada Survey Report described cpKPI activities delivered at hospitals with fewer than 200 beds but excluded those with fewer than 50 beds.10 Another survey of 24 Canadian hospitals outside of British Columbia with fewer than 50 beds reported that provision of cpKPI activities was highly variable across hospitals.11
Describing the delivery of clinical pharmacy services in small BC hospitals will help to frame opportunities for improvement. Moreover, characterizing the factors that influence clinical pharmacy service provision at small hospitals will guide the use of effective change strategies to improve service at small hospitals. Several possible contextual factors, such as workforce and funding, could influence clinical pharmacy implementation in small hospitals.5 A systematic review revealed that factors influencing clinical pharmacy service implementation are multifactorial and uniformly distributed across attitudinal, political, technical, and administrative domains.12 However, most hospitals included in that synthesis had more than 200 beds, and the results may not be generalizable to the small hospital setting.
The Consolidated Framework for Implementation Research (CFIR) is a validated, determinant framework that addresses contextual factors influencing the implementation of any health care intervention.11 It has been used to determine factors influencing implementation of pharmaceutical care in outpatient settings and is suitable for ascertaining factors associated with clinical pharmacy service implementation in small hospitals.13,14 The aims of this study were to characterize clinical pharmacy service delivery at small hospitals in British Columbia and to identify the context-specific barriers and enablers to providing those services.
This study involved an internet-based survey questionnaire (data collected through Qualtrics software). A total population sampling strategy was applied, targeting BC small hospital pharmacy licence holders. Licence holders of on-site pharmacy departments in BC hospitals with fewer than 200 acute care beds were included; however, licence holders of small hospital pharmacy departments designated as satellite pharmacies were excluded because their primary function is to provide drug distribution services. Potential participants could hold multiple pharmacy licences. To determine the target sample, 2 investigators (S.T., S.K.G.) independently cross-referenced the College of Pharmacists of British Columbia’s public directory of pharmacy licence holders15 with the Canadian Institute for Health Information’s 2019/20 report of beds staffed and in operation in Canada,2 as well as with individual hospital webpages.
The survey questionnaire consisted of 2 sections (Appendix 1). The first section was intended to be completed for each licensed hospital pharmacy and consisted of 8 questions that assessed characteristics of the hospital and pharmacy staff, the pharmacy practice model (where a hospital could report more than 1 model, if appropriate), the presence of on-site clinical pharmacy services (defined as all activities performed by a pharmacist that required in-person interaction with the inpatient and the health care team to optimize drug therapy), and the reported types of cpKPIs and the intensity of their delivery.
The 8 cpKPI activities assessed were admission medication reconciliation, development and implementation of a pharmaceutical care plan, assessment and resolution of drug therapy problems (DTPs), participation in interprofessional patient care rounds led by a prescriber, patient education during the hospital stay, discharge medication reconciliation, patient medication education at hospital discharge, and provision of a comprehensive direct patient care bundle that included all of the aforementioned cpKPI activities. A 4-point Likert-type scale (1, never; 2, for some patients; 3, for most patients; 4, for all patients) was used to quantify cpKPI delivery.
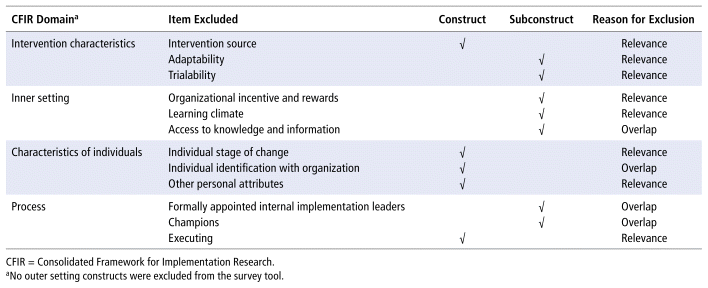
The second section of the survey was completed once by each participant and consisted of 32 statements that assessed barriers to and enablers of clinical pharmacy service implementation and improvement; again, a 4-point Likert-type scale (1, strongly disagree; 2, disagree; 3, agree; 4, strongly agree) was used to characterize responses. The 32 barrier and enabler statements were developed using the CFIR interview guide.11,16 The CFIR consists of 5 domains, 26 constructs, and 13 subconstructs that can influence implementation of an intervention. The domains are intervention characteristics, outer setting, inner setting, characteristics of individuals, and process. The survey tool included CFIR statements deemed by the investigators to be relevant to clinical pharmacy services. Of the 39 CFIR constructs and subconstructs, 12 were excluded because the investigator team determined they had little relevance to small hospital clinical pharmacy services or they had significant overlap with other CFIR items (Appendix 2). More than 1 statement was used to assess 6 of the constructs, and each of the other CFIR items was assessed using a single statement. There was also 1 optional free-text question soliciting participants’ perceptions of barriers to implementing and improving clinical pharmacy services. The survey tool was pretested by the investigator team to ensure the stem statements and response options were clear and functional.
Survey participation was anonymous, and the survey was open from January to April 2022. Once a participant had started the survey questionnaire, they were given 6 weeks to complete it. To help optimize response rate, a personalized prenotification email was sent 10 days before the formal survey invitation.17 This was followed by a formal invitation to participate, also sent by email, which included the link to the online survey. Reminder emails were sent 2 and 4 weeks after the formal invitation.17 The research was conducted in accordance with the ethical standards of the Interior Health research ethics board (2021-22-085-H) and the Helsinki Declaration. All participants were required to provide informed consent before completing the survey.
All quantitative data were analyzed using descriptive statistics. Likert-type scale data were analyzed using frequency distributions. Depending on the orientation of the CFIR statement stem, enablers and barriers were identified when more than 50% of respondents selected the agree or disagree options on the Likert-type scale. One investigator (S.T.) coded the free-text responses and grouped them into common themes using open semantic coding to identify the most common barriers to clinical pharmacy service delivery.
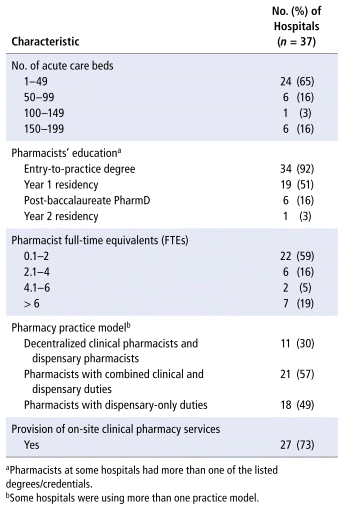
Of the 23 small hospital pharmacy licence holders invited to participate, 18 (78%) responded, representing 37 (64%) of the 58 small hospitals in British Columbia. Hospital and pharmacy department characteristics are shown in Table 1. Twenty-four (65%) of the hospitals had fewer than 50 beds, 19 (51%) hospitals employed pharmacists who had Accredited Year-1 Pharmacy Residency certification, 22 (59%) employed 0.1 to 2 pharmacist full-time equivalents (FTEs), 21 (57%) deployed a pharmacy practice model consisting of pharmacists who performed both clinical and drug distribution duties while on shift, and 27 (73%) had on-site clinical pharmacy services.
TABLE 1 Characteristics of Small Hospital Pharmacies

The 18 pharmacy licence holders, representing 27 small hospitals with clinical pharmacy services, provided information about cpKPI activities performed by on-site pharmacists (Figure 1). Resolution of DTPs and provision of patient education during the hospital stay were delivered for at least some patients at all 27 (100%) of these small hospitals. Resolution of DTPs, admission medication reconciliation, and participation in rounds were performed for all patients at 4 (15%), 3 (11%), and 3 (11%) of the 27 hospitals, respectively. The most common cpKPI activities reported as never being performed were the comprehensive patient care bundle (15/27, 56%) and discharge medication reconciliation (11/27, 41%). Admission medication reconciliation, discharge patient education, active participation in interprofessional patient care rounds, and pharmaceutical care planning were reported to never occur at 5 (19%), 4 (15%), 2 (8%), and 1 (4%) of the 27 hospitals, respectively.
|
| ||
|
FIGURE 1 Frequency of clinical pharmacy key performance indicator activities reported at small hospitals. | ||
There were 9 CFIR barriers to implementing and improving clinical pharmacy services (Figure 2a). The top barriers were the absence of regular exchange of information about clinical pharmacy service implementation and improvement with others outside the organization (17/18, 94%), not having sufficient resources (operating funds, dedicated personnel, space, equipment, and/or information technology) to implement and improve clinical pharmacy services (16/18, 89%), absence of a hospital-level plan for implementing and improving clinical pharmacy services (13/18, 72%), and inability to juggle competing work priorities with the implementation and improvement of clinical pharmacy services (12/18, 67%).
|
| ||
|
FIGURE 2 (a) Barriers to and (b) enablers of clinical pharmacy services, as outlined by the Consolidated Framework for Implementation Research. | ||
Perceived barriers to implementing and improving clinical pharmacy services, as determined from answers to the free-text question on this topic, are shown in Table 2. The 3 most common barriers were funding constraints (14/18, 78%), staff recruitment and retention challenges (13/18, 72%), and leadership structure (6/18, 33%).
TABLE 2 Analysis of Barriers to Clinical Pharmacy Services, as Reported in Free-Text Responses

There were 21 enablers of clinical pharmacy service implementation and improvement (Figure 2b). Five of these enablers had unanimous support among respondents: acknowledgement of published scientific evidence demonstrating the effectiveness of clinical pharmacy services, the perception that patients’ needs and preferences will be met with service implementation and improvement, the perception that patients will be satisfied with service implementation and improvement, the existence of a strong need to implement and improve clinical pharmacy services, and the perception that implementation and improvement of clinical pharmacy services will improve the overall quality of care. Pharmacists’ perceptions that there is enough supporting evidence for clinical pharmacy service implementation and improvement at their hospital and alignment of clinical pharmacy service implementation and improvement with organizational values and norms were also frequently cited (17/18 [94%] for each).
Characterizing on-site clinical pharmacy services establishes the improvement opportunities at small BC hospitals. Identifying factors that influence clinical service delivery informs the selection of effective implementation and improvement strategies. Three-quarters of all hospitals reported the provision of on-site clinical pharmacy services, and most of the hospitals surveyed had fewer than 50 beds. The predominant practice model for pharmacists was hybrid delivery of both clinical and distribution services while on shift, which could be explained by many of the small hospitals having no more than 2 pharmacist FTEs. Similar rates of the hybrid and distribution-only models have been reported for Canadian hospitals with 50 to 200 beds.10 In a survey of small hospitals in other Canadian provinces, the hybrid model was most prevalent.18
The cpKPI activities provided for at least some patients at all hospitals represented in this study were DTP resolution and patient education. Resolving DTPs can be performed both in patient care areas and in pharmacy departments, which may explain why this activity was provided, to some extent, at all hospitals. We hypothesize that the provision of patient education was widespread because it can be requested by other health care team members through distribution-based pharmacist consultation or it can be performed by ward-based clinical pharmacists. It is also possible that respondents mistakenly reported this activity in the context of outpatient dispensing services. A recent survey of pharmacy services in small hospitals reported that patient education was provided at more than half of responding hospitals,18 and a Canadian cpKPI registry study reported patient education as the activity most rarely performed.19 However, hospital size was not reported in the latter study, so comparability to the small hospital context is unclear. A few respondents in the current study reported that DTP resolution, participation in rounds, and admission medication reconciliation were performed for all patients. The finding related to rounds participation was unexpected because medical care in small hospitals is often delivered by family physicians who have combined office and acute care practices, which can prevent their participation in patient care rounds.20 It is also possible that respondents reported pharmacist participation on rounds that did not involve a physician. Medication reconciliation is an Accreditation Canada Required Organizational Practice,21 which may explain why it was reported as being provided for all patients at some hospitals. Conversely, at more than half of the hospitals, the comprehensive direct patient care bundle was never provided. This finding may be explained by the common use of hybrid and distribution-only practice models, both of which reflect competing demands on pharmacists’ time.
Nine barriers to clinical pharmacy service implementation and improvement were identified using the CFIR framework. Lack of regular exchange of information about clinical pharmacy services with others outside the organization was the most common barrier reported. It is possible that small hospital pharmacy licence holders do not have access to an organized network of colleagues in British Columbia with an agenda focusing on clinical pharmacy services. Three other common barriers were that clinical pharmacy services were not considered a top organizational priority, that no associated organizational goals existed, and that no evaluation plan was in place. These barriers are interrelated and could be addressed at the organizational level by emphasizing that clinical pharmacy services improve overall health care quality. Other change strategies to address these barriers include communicating how clinical pharmacy services can be tailored to meet local needs, implementing cpKPI tracking for quality monitoring, and communicating cpKPI results to organizational leaders.22
Open-ended (free-text) responses revealed funding constraints, personnel recruitment and retention, and pharmacy leadership structure as common barriers. Funding and staffing barriers align with the CFIR statement related to insufficient resources. A systematic review identified clinical capability and time requirements as the most crucial factors influencing clinical pharmacy service implementation.12 The applicability of these results to the small hospital context is limited because most of the studies included in the review were conducted at large hospitals. Tension between clinical and operational pharmacy leaders was reported as a barrier preventing operational leaders from implementing and improving clinical services. This barrier could be overcome by ensuring that clinical pharmacy governance is broadly represented by pharmacy leaders across a health region.
A total of 21 enablers were identified, and these could be used to implement and improve clinical pharmacy services. Participants most often indicated that clinical pharmacy services are strongly needed, that they will improve the quality of care and patient satisfaction, and that they align with organizational culture. These enablers suggest that pharmacy licence holders are capable and motivated to drive clinical service implementation and improvement.
Several strengths were associated with this study. The high response rate increased the probability that a representative sample of small hospitals was included. Systematically developed cpKPI activities were used to assess the type and intensity of clinical pharmacy services and allowed for service comparisons across hospitals. The validated CFIR framework was used to identify contextual factors associated with implementation and improvement that can be mapped to proven implementation strategies.22 Consideration of these contextual factors will improve the efficiency and effectiveness of change management in this area.
This study also had some limitations. The survey was not validated; instead, it was pretested by the investigator team, and the cpKPI reporting resembled other published surveys.10,18 It is possible that other clinical activities not considered cpKPIs were performed at the responding hospitals. Nevertheless, capturing cpKPI activities to characterize clinical services is valuable because these measures are associated with improved quality, safety, and patient experience.23 The survey used the CFIR, a validated implementation science framework, to identify contextual factors that influence implementation success.11 The CFIR statements were tailored to the hospital pharmacy context and aimed to improve survey clarity and conciseness. Even so, despite modifications and pretesting, it is possible that the CFIR statements were misunderstood. Semistructured interviews or focus groups could have been used to enhance participant comprehension, but that would have precluded use of a total population sampling method and would not have generated quantitative measures. A recently developed 14-item tool that quantitatively assesses CFIR implementation factors might have enhanced the clarity of questions within our survey tool.24 Because participants were exclusively pharmacy licence holders who typically have supervisory responsibilities, it is possible that the views captured in our survey differed from the views of front-line pharmacists working in these settings. Finally, this survey was deployed during the COVID-19 pandemic and thus may have yielded barriers and enablers differing from those that would be observed in the nonpandemic context.25
The factors identified in this study should be mapped to evidence-based change strategies to effectively implement and improve clinical pharmacy services.22 Future research is needed to assess the acceptability, practicability, effectiveness, affordability, and unintended adverse consequences of implementing these strategies in small hospitals across British Columbia. Moreover, future strategies to implement and improve clinical pharmacy services should be implemented based on meaningful patient engagement.
Most small hospitals in British Columbia reported on-site clinical pharmacy services; however, some cpKPI activities were never or rarely performed. Change strategies should be implemented that overcome barriers related to inadequate external networking, securing sufficient resources, planning, and managing competing priorities. Moreover, pharmacy leaders demonstrated an understanding of the value of and strong need for clinical pharmacy services, which can enable implementation and improvement at small hospitals.
1 Accessing core plan products and services. Canadian Institute for Health Information; 2021 [cited 2025 Jan 28]. Available from: https://secure.cihi.ca/estore/coreplan.htm
2 Hospital beds staffed and in operation, 2019–2020 [Excel spreadsheet]. Canadian Institute for Health Information; 2021 [cited 2025 Jan 28]. Available from: https://www.cihi.ca/sites/default/files/document/beds-staffed-and-in-operation-2020-2021-en.xlsx
3 American Hospital Association; American Society of Health-System Pharmacists; Hospitals & Health Networks. Medication Safety Issue Brief. Small and rural hospitals - unique challenges, unique solutions. Hosp Health Netw. 2005;79(11):45–6.
4 Rechel B, Dzakula A, Duran A, Fattore G, Edwards N, Grignon M, et al. Hospitals in rural or remote areas: an exploratory review of policies in 8 high-income countries. Health Policy. 2016;120:758–69.
Crossref PubMed
5 Vaughan L, Edwards N. The problems of smaller, rural and remote hospitals: separating facts from fiction. Future Healthc J. 2020;7(1): 38–45.
Crossref PubMed PMC
6 Kaboli PJ, Hoth AR, McClimon BJ, Schnipper JL. Clinical pharmacists and inpatient medical care: a systematic review. Arch Intern Med. 2006;166:955–64.
Crossref PubMed
7 Makowsky MJ, Koshman SL, Midodzi WK, Tsuyuki RT. Capturing outcomes of clinical activities performed by a rounding pharmacist practicing in a team environment: the COLLABORATE study. Med Care. 2009;47(6):642–50.
Crossref PubMed
8 Gillespie U, Alassaad A, Henrohn D, Garmo H, Hammarlund-Udenaes M, Toss H, et al. A comprehensive pharmacist intervention to reduce morbidity in patients 80 years or older: a randomized controlled trial. Arch Intern Med. 2009;169(9):894–900.
Crossref PubMed
9 Fernandes O, Toombs K, Pereira T, Lyder C, Bjelajac Mejia A, Shalansky S, et al. Canadian consensus on clinical pharmacy key performance indicators: quick reference guide. Canadian Society of Hospital Pharmacists; 2015 [cited 2025 Jan 28]. Available from: https://www.cshp.ca/common/Uploaded%20files/PDFs/CSPH-Can-Concensus-cpKPI-QuickReferenceGuide_June_2017.pdf
10 Bussières JF, Merrill D. Chapter B – Clinical pharmacy practice. In: Hospital Pharmacy in Canada Survey Board (editors). Hospital pharmacy in Canada survey report 2020/21. Canadian Society of Hospital Pharmacists; 2022 [cited 2025 Jan 28]. pp. 25–62. Available from: https://cshp.ca/common/Uploaded%20files/PDFs/HPCS-2020-21-Report-ENG.pdf
11 Damschroder LJ, Aron DC, Keith RE, Kirsh SR, Alexander JA, Lowery JC. Fostering implementation of health services research findings into practice: a consolidated framework for advancing implementation science. Implement Sci. 2009;4:50.
Crossref PubMed PMC
12 Onozato T, Francisca dos Santos Cruz C, Milhome da Costa Farre AG, Silvestre CC, de Oliveira Santos Silva R, Araujo dos Santos Júnior G, et al. Factors influencing the implementation of clinical pharmacy services for hospitalized patients: a mixed-methods systematic review. Res Social Adm Pharm. 2020;16(4):437–49.
Crossref
13 Pereira CE, Bambirra EF, Fernandes BD, Sousa MC, Mendoca SA, Chemello C. Factors influencing the implementation of pharmaceutical care in outpatient settings: a systematic review applying the Consolidated Framework for Implementation Research. Res Social Adm Pharm. 2022;18(4):2579–92.
Crossref
14 Moecker R, Terstegen T, Haefeli WE, Seidling HM. The influence of intervention complexity on barriers and facilitators in the implementation of professional pharmacy services - a systematic review. Res Social Adm Pharm. 2021;17(10):1651–62.
Crossref PubMed
15 Find a pharmacy or registrant [online directory of licensed hospital pharmacies]. College of Pharmacists of British Columbia; 2021 [cited 2021 Nov 14]. Available from: https://www.https://www.bcpharmacists.org/search-pharmacy
16 CFIR interview guide tool. CFIR Research Team; 2021 [cited 2021 Nov 14]. Available from: https://cfirguide.org/guide/app/#/
17 Sammut D, Griscti D, Norman P. Strategies to improve response rates to web surveys: a literature review. Int J Nurs Stud. 2021;123:104058.
Crossref PubMed
18 Newman P, Dhaliwall S, Polyakova O, McDonald K. Pharmacy distribution, clinical, and management services: a survey of small hospitals in Canada supported by telepharmacy services. Can J Hosp Pharm. 2021; 74(3):256–68.
Crossref PubMed PMC
19 Zhou Y, Fernandes O, Carroccia A, Saragosa J, Lowe D, Toombs K, et al. What type of clinical pharmacy key performance indicators (cpKPI) care are patients receiving across Canada? A 4-year national cpKPI patient care registry trending with clinical speciality analysis [abstract]. Can J Hosp Pharm. 2023;76(2):146.
20 Hedden L, Banihosseini S, Strydom N, McCracken R. Family physician perspectives on primary care reform priorities: a cross-sectional survey. CMAJ Open. 2021;9(2):E466–E473.
Crossref PubMed PMC
21 Required Organizational Practices: Qmentum global handbook – acute care. Health Standards Organization; 2024 May.
22 Powell BJ, Waltz TJ, Chinman MJ, Damschroder LJ, Smith JL, Matthieu MM, et al. A refined compilation of implementation strategies: results from the Expert Recommendations for Implementing Change (ERIC) project. Implement Sci. 2015;10:21.
Crossref PubMed PMC
23 Fernandes O, Gorman SK, Slavik RS, Semchuk WM, Shalansky S, Bussières JF, et al. Development of clinical pharmacy key performance indicators for hospital pharmacists using a modified Delphi approach. Ann Pharmacother. 2015;49(6):656–69.
Crossref PubMed
24 Robinson CH, Damschroder LJ. A pragmatic context assessment tool (pCAT): using a Think Aloud method to develop an assessment of contextual barriers to change. Implement Sci. 2023;4:3.
Crossref
25 Ring E, Isenor JE, Slayter K, MacInnis M, Black EK. Barriers and facilitators related to delivery of hospital pharmacy services to women, children, and their families during a pandemic: a qualitative study. Can J Hosp Pharm. 2022;75(3):210–8.
Crossref PubMed PMC
Address correspondence to: Dr Sean K Gorman, Interior Health Authority, 505 Doyle Ave, Kelowna BC V1Y 0C5, email: Sean.gorman@interiorhealth.ca
Competing interests: None declared.
Funding: None received.
Acknowledgement: For assistance with the preparation of this manuscript, the authors would like to thank Harsimran Dass, BSc, who, at the time of this submission, was a Doctor of Pharmacy student at the University of British Columbia.
Submitted: February 7, 2025
Accepted: July 7, 2025
Published: October 8, 2025
(Likert-type scale: 1-strongly disagree; 2-disagree; 3-agree; 4-strongly agree)
What are the top 3 barriers to implementing and/or improving clinical pharmacy services at your hospital(s)? ___________________________________________(free text)
© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 4, 2025