Doson Chua, Brittany Buffone, Hayley Hefford, Ricky Turgeon, and Jasmine GrewalTo cite: Chua D, Buffone B, Hefford H, Turgeon R, Grewal J. Clinical pharmacists’ activities and patient outcomes in an adult congenital heart disease clinic. Can J Hosp Pharm. 2025;78(4):e3800. doi: 10.4212/cjhp.3800
The management of adult congenital heart disease (ACHD) is challenging due to patients’ complex cardiac physiology, cardiac and noncardiac comorbidities, the prevalence of polypharmacy, and the lack of strong treatment evidence.1 Congenital heart disease is diagnosed during infancy, and its treatment involves multiple complex cardiac surgeries to correct abnormalities such as tetralogy of Fallot, transposition of the great arteries, and various cardiac shunts. Due to altered cardiac physiology, disease states such as heart failure (HF), atrial fibrillation, and cardiac valvular abnormalities are common in ACHD. As a consequence of these cardiac abnormalities, noncardiac disorders, including pulmonary hypertension, thromboembolism, ascites, protein-losing enteropathy (PLE), and chronic kidney disease, are frequently encountered as well.1 In the context of these multiple and complex cardiac and noncardiac comorbidities, polypharmacy is commonplace among patients with ACHD.
In British Columbia (BC), patients with congenital heart disease are followed by the BC Children’s Hospital from birth until age 19 years, after which their ongoing medical care is transferred to St Paul’s Hospital (SPH), the province’s quaternary cardiac referral centre for ACHD, which currently follows more than 3000 affected patients. As the complexity and volume of this patient population has increased, SPH incorporated a 0.2 full-time equivalent (FTE) clinical cardiac pharmacist dedicated to the ACHD program and an HF medication optimization pharmacist (consult basis only) specifically to manage HF pharmacotherapy in selected patients with ACHD at SPH.
Clinical pharmacists have well-established roles in the management of several cardiovascular conditions, including HF, atrial fibrillation, dyslipidemia, and hypertension, as well as intensive care management of patients with these conditions; however, the role of clinical pharmacists in the care of patients with ACHD and the resulting patient outcomes have not been delineated in the literature.2
The 0.2 FTE clinical pharmacist position (role fulfilled by B.B. and H.H.) and the HF medication optimization pharmacist (R.T.) support the ACHD program primarily in the SPH ACHD clinics for outpatients and on a consult basis. The HF pharmacist already has an established role in other SPH clinics, independently managing patients’ pharmacotherapy for HF; as such, it was easy to expand this service to ACHD clinics.3 The 0.2 FTE clinical pharmacist position is specifically funded by the ACHD program, and their schedule is structured to have dedicated time on Fridays to support the ACHD program (largely to help with drug-related issues outside HF management); in practical terms, however, ACHD consults are received continually on weekdays. The HF medication optimization pharmacist is available to assume management of HF guideline-directed medical therapies (GDMTs) for patients with ACHD on a consult basis. More specifically, this pharmacist sees patients independently (in the SPH ACHD clinics or virtually) to initiate, titrate, and monitor GDMT through a hospital- and medical program–approved collaborative prescribing practice.3 The ACHD clinical pharmacist carries out clinical interventions through multidisciplinary team–based clinics and the prescribing and prescription adaptation bylaws of the provincial college of pharmacists.4,5 The clinical pharmacists in both of these roles may independently follow the patient longitudinally, depending on the patients’ needs and the nature of the consult.
The 0.2 FTE clinical pharmacists and the HF medication optimization pharmacist are closely supported by the SPH pharmacy department and its inpatient cardiac clinical pharmacists. The clinical pharmacists supporting the ACHD program have a strong background in cardiology pharmacotherapeutics, a well-established role and presence in the SPH Division of Cardiology, and strong relationships with SPH cardiologists. The clinical pharmacists’ support for the ACHD program is available on weekdays only.
ACHD pathophysiology is complex and can have multi-organ manifestations, which influence drug selection, dosing, and monitoring. A common scenario is ACHD-related PLE, characterized by chronic diarrhea, significant hypoalbuminemia, congestive hepatopathy, and kidney disease. The clinical pharmacist is commonly involved in drug selection and is specifically responsible for monitoring the efficacy and toxicity of anticoagulant, anticonvulsant, antimicrobial, and PLE-related drug therapies. This work can include adjusting drug therapies based on chromogenic Factor Xa levels, anticonvulsant drug levels, select antimicrobial drug levels, α-1-antitrypsin clearance, and serum protein levels, as well as treating vitamin deficiencies that may be associated with PLE.
Another common scenario involves patients with ACHD who become pregnant or who have recently given birth. Patients with ACHD routinely take cardiovascular, anticoagulant, and pulmonary vasodilator drugs, and these specific drug therapies must be reviewed when a patient becomes pregnant. Selection and monitoring of drug therapies in the peripartum phase require careful consideration of drug teratogenicity and changes in maternal protein binding and maternal ACHD cardiovascular hemodynamics during pregnancy. As well, pharmacists are routinely involved in postpartum selection of cardiovascular drugs for patients who breastfeed their infants.
For this quality improvement project, we retrospectively reviewed aggregate data collected by the 0.2 FTE ACHD clinic pharmacists and HF optimization pharmacist as part of their daily clinical duties and provision of support to the SPH ACHD program. Data collected included (but were not limited to) the type of clinical pharmacist activity, the number and nature of clinical pharmacy consult requests (from physicians, allied health professionals, and patients), and outcomes for patients with ACHD following the addition of the 0.2 FTE clinical pharmacist position and the pharmacist-led HF GDMT optimization service. Data were collected for all consecutive patients seen in the ACHD clinic for whom a clinical pharmacist was consulted between September 1, 2023, and April 30, 2024, as well as for patients with a consult from the HF medication optimization pharmacist between September 1, 2023, and July 31, 2024. Patients with ACHD who could not be contacted by the clinical pharmacists or who did not show up to appointments were excluded. The results are presented using descriptive statistics.
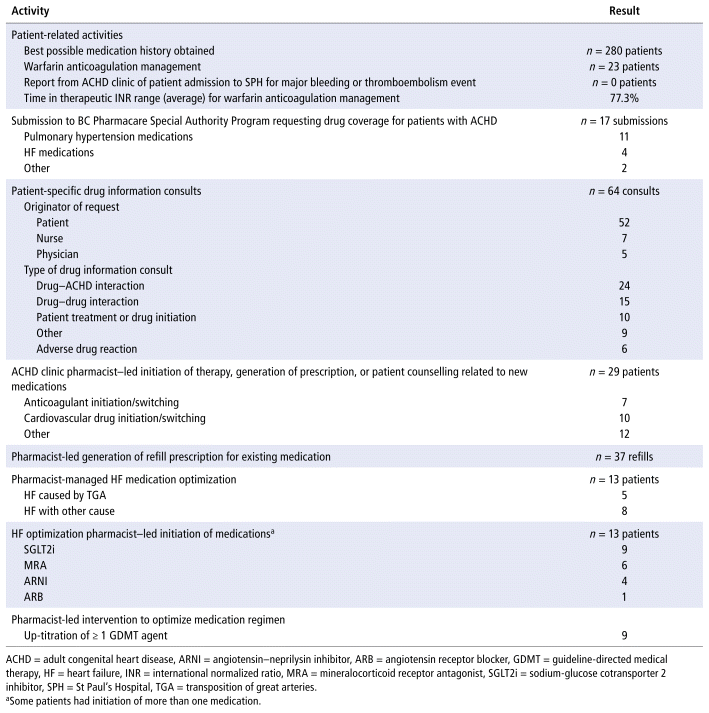
The data collected for the study period are summarized in Table 1. Clinical pharmacists completed 280 best possible medication histories (BPMHs) for patients who were to be seen virtually in the ACHD clinics. As well, clinical pharmacists managed and titrated warfarin to international normalized ratio targets for 23 patients, with no reports of major bleeding requiring intervention or thromboembolic events. Provincial medication drug coverage requiring prior authorization (British Columbia Pharmacare Special Authority Program) was obtained for 17 patients; prior authorization involves completing an application with patient-specific information and the rationale for the medication coverage request. A substantial number of these prior authorizations were for pulmonary hypertension–related medications, which can be costly for patients. Clinical pharmacists were frequently asked to provide drug information, mainly by patients seeking information about their specific medication regimens. The majority of drug information consults were related to disease–drug interactions (i.e., drug-related concerns in the context of ACHD) and potential drug–drug interactions. Clinical pharmacists were also active in medication management and prescriptive activities, such as managing prescriptions for anticoagulation, switching cardiovascular drugs, and providing prescription refills. We estimated that each activity required an average of 30 minutes, depending on the complexity of the consult and request.
TABLE 1 Clinical Pharmacist Activities and Patient Outcomes in ACHD Program, St Paul’s Hospital, Vancouver, British Columbia

The HF medication optimization pharmacist was consulted to manage the cases of 13 patients with ACHD and stable HF and was able to initiate and optimize GDMT for these patients. More specifically, the HF optimization pharmacist followed the institution’s approved protocols to independently assess and prescribe appropriate HF GDMT for these patients, as well as to manage medications for diuresis and arrange follow-up visits and laboratory testing. There were no reports of significant adverse outcomes leading to hospitalization or urgent SPH ACHD clinic visits for patients whose care was managed by the HF medication optimization pharmacist.
To our knowledge, this is the first study describing and quantifying the activities and roles of clinical pharmacists supporting ACHD clinics and the associated patient outcomes. Several previous publications highlighting the activities of clinical pharmacists in atrial fibrillation clinics, anticoagulation clinics, and HF clinics established the benefit of clinical pharmacists in terms of clinical outcomes for patients treated within these focused areas.6–9 Given that patients with ACHD commonly have many cardiac comorbidities, it is not surprising that clinical pharmacists’ contributions to the management of other cardiovascular disease states can be easily transferred to the management of ACHD. Our results highlight that clinical pharmacists provide support in a multitude of ways, from disease state management (such as HF and anticoagulation management) to the provision of patient-specific drug information and the performance of procedural tasks such as applying for drug coverage and managing prescriptions.
The benefit of a pharmacy-led HF medication optimization service has been previously documented, and our results are consistent with prior observations.3,10 The HF medication optimization pharmacist was able to independently see patients, optimize GDMT and diuretic therapy, order appropriate laboratory tests, and arrange follow-up, thereby freeing up ACHD clinic visits for the ACHD cardiologist to see other patients, which in turn has the potential to increase overall patient capacity in the ACHD clinic.
Clinical pharmacists obtained a substantial number of BPMHs during the study period. The BMPH is critical to patient care, as medical decisions and the prescribing of drug therapy are dependent on an accurate assessment of the patient’s current drug therapies. Additionally, the clinical pharmacists responded to a substantial number of patient-specific drug information requests. Patients with ACHD have complex cardiac physiology and other noncardiac manifestations of ACHD, and there is a lack of treatment evidence in ACHD; as such, drug therapy choices can be difficult. In addition, given the possibility of significant polypharmacy in ACHD, clinical pharmacists are well suited to augment not only treatment of the cardiac condition, but also medication management and adherence.11
Clinical pharmacists provided a wide range of pharmacy services to patients with ACHD receiving care at SPH, with positive outcomes. As the complexity of ACHD cases increases, comorbidities and polypharmacy will likely increase as well. Clinical pharmacists have the potential to address drug-related concerns for these patients, allowing more time for physicians and nurses to address other medical issues in the ACHD clinic.
Although our small pilot quality improvement initiative showed promise, further research into the role of clinical pharmacists supporting ACHD clinics and associated patient outcomes is warranted.
1 Marelli A, Beauchesne L, Colman J, Ducas R, Grewal J, Keir M, et al. Canadian Cardiovascular Society 2022 guidelines for cardiovascular interventions in adults with congenital heart disease. Can J Cardiol. 2022; 38(7):862–96.
PubMed
2 Dunn S, Birtcher K, Beavers C, Baker WL, Brouse SD, Page RL, et al. the role of the clinical pharmacist in the care of patients with cardiovascular disease. J Am Coll Cardiol. 2015;66(19):2129–39.
Crossref PubMed
3 Ladhar S, Hawkins N, Virani SA, Turgeon RD. Evaluation of PHARM-HF, a pharmacist-led heart failure medication titration clinic: a pre-post study. J Am Coll Clin Pharm. 2024;7:416–25.
Crossref
4 PPP-58: Adapting a prescription [policy]. College of Pharmacists of British Columbia; [cited 2025 Jun 15]. Available from: https://www.bcpharmacists.org/adapting-prescription
5 Pharmacist prescribing for minor ailments and contraception (PPMAC). College of Pharmacists of British Columbia; 2023 [cited 2025 Jun 15]. Available from: https://www.bcpharmacists.org/ppmac
6 Andrade JG, Aguilar M, Atzema C, Bell A, Cairns JA, Cheung CC, et al. The 2020 Canadian Cardiovascular Society/Canadian Heart Rhythm Society comprehensive guidelines for the management of atrial fibrillation. Can J Cardiol. 2020;36(12):1847–948.
PubMed
7 Shalansky S, Basi S, Yu C. Practice spotlight: pharmacists in a multidisciplinary atrial fibrillation clinic. Can J Hosp Pharm. 2011;65(5):370–1.
8 Beauchesne AB, Koshman SL, Beavers CJ, Gorman SK, Turgeon RD. Defining pharmacist activities in ambulatory heart failure clinics: North American survey and modified Delphi study. J Am Coll Clin Pharm. 2023;6:1180–90.
Crossref
9 Hache J, Bonsu KO, Chitsike R, Nguyen H, Young S. Assessment of a pharmacist-led direct oral anticoagulant monitoring clinic. Can J Hosp Pharm. 2021;74(1):7–14.
Crossref PubMed PMC
10 Cao V, Cowley E, Koshman SL, MacGillivary J, Sidsworth M, Turgeon RD. Pharmacist-led optimization of heart failure medications: a systematic review. J Am Coll Clin Pharm. 2021;4(7):862–70.
Crossref
11 Woudstra OI, Kuijpers JM, Meijboom FJ, Post MC, Jongbloed MRM, Duijnhouwer AL, et al. High burden of drug therapy in adult congenital heart disease: polypharmacy as marker of morbidity and mortality. Eur Heart J Cardiovasc Pharmacother. 2019;5(4):216–25.
Crossref PubMed PMC
Address correspondence to: Dr Doson Chua, Pharmacy Department, St Paul’s Hospital, 1081 Burrard Street, Vancouver BC V6Z 1Y6, email: dchua@providencehealth.bc.ca
Competing interests: None declared.
Funding: None received.
Submitted: February 19, 2025
Accepted: July 19, 2025
Published: October 8, 2025
© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 4, 2025