Original Research
What Clinical Pharmacy Key Performance Indicator Processes of Care Were Patients Receiving across Canada in 2018? A National Patient Registry and Pooled Analysis
Amanda Carroccia, Olavo A Fernandes, Kent Toombs, Sean K Gorman, Sean P Spina, William M Semchuk, Andrea Meade, Donna Lowe, Tania Bayoud, Stephen Shalansky, Nadia M Facca, Winnie Seto, Jean-François Bussières, Gary G Wong, Philip Lui, Richard S Slavik, Douglas Doucette, Gali Latariya, and Clarence Chant
To cite: Carroccia A, Fernandes OA, Toombs K, Gorman SK, Spina SP, Semchuk WM, et al. What clinical pharmacy key performance indicator processes of care were patients receiving across Canada in 2018? A national patient registry and pooled analysis. Can J Hosp Pharm. 2025;78(4):e3819. doi: 10.4212/cjhp.3819
ABSTRACT
Background
National consensus-based clinical pharmacy key performance indicators (cpKPIs) are health quality indicators representing processes of care associated with an impact on meaningful patient outcomes. Canadian hospitals are measuring cpKPIs at the local level. However, variations exist regarding which cpKPIs are measured and the associated cpKPI practice profiles. At the time this study was undertaken, a national registry did not exist to capture real-world cpKPI patient data and to track pooled national progress.
Objectives
To develop a national cpKPI patient registry, to characterize cpKPI-related care delivered, and to generate pooled national summary cpKPI reports to inform the advancement of pharmacy practice and improve patient outcomes.
Methods
In this national, retrospective, observational quality improvement study, hospitals measuring at least one cpKPI in at least one inpatient area were enrolled and submitted aggregated, de-identified cpKPI patient data for the calendar year 2018 (January to December). Patient-proportion cpKPI data for individual hospitals were summarized, and pooled national reports were generated.
Results
Overall, 32 Canadian health care organizations were enrolled, capturing 275 896 patient visits. The core analysis focused on 25 acute care institutions that were continuously measuring cpKPIs. The most commonly delivered cpKPI processes of care were development of a pharmaceutical care plan (59% of patients), resolution of drug therapy problems (37% of patients), and participation in interprofessional patient care rounds (36% of patients). The least commonly delivered cpKPI care services were patient medication education during the hospital stay (7% of patients), medication reconciliation at discharge (15% of patients), and patient medication education at discharge (17% of patients).
Conclusions
The first national registry for capturing clinical pharmacy health quality indicators was established and used to characterize real-world cpKPI-related patient care delivery. The findings from this registry could facilitate hospital-level cpKPI benchmarking and could support national sharing of best practices to advance pharmacy practice and improve patient outcomes.
KEYWORDS: health quality indicators, key performance indicators, clinical pharmacy, patient registry, pharmaceutical care, medication reconciliation
RÉSUMÉ
Contexte
Les indicateurs clés de performance en pharmacie clinique (cpKPI) basés sur un consensus national sont des indicateurs de qualité de la santé liés à des processus de soins ayant une incidence sur des résultats significatifs pour la santé des patients. Les hôpitaux canadiens les mesurent à l’échelle locale. Cependant, on constate des variations quant aux cpKPI mesurés et aux profils de pratique qui y sont associés. Au moment où cette étude a été entreprise, aucun registre national n’existait pour collecter des données réelles en rapport avec les patients concernant les cpKPI et pour suivre les progrès nationaux consolidés.
Objectifs
Développer un registre national de patients pour les cpKPI, caractériser les soins associés aux cpKPI dispensés et produire des rapports nationaux consolidés afin d’éclairer les progrès de la pratique de la pharmacie et d’améliorer les résultats pour les patients.
Méthodologie
Dans cette étude nationale, rétrospective et observationnelle d’amélioration de la qualité, les hôpitaux mesurant au moins un cpKPI dans au moins un secteur de soins hospitaliers ont été inclus et ont soumis des données de patients agrégées et anonymisées relatives aux cpKPI pour l’année civile 2018 (de janvier à décembre). Les données des cpKPI, exprimées en proportion de patients pour chaque hôpital, ont été résumées avant de produire des rapports nationaux consolidés.
Résultats
Au total, 32 établissements de santé canadiens ont été inclus, représentant 275 896 visites de patients. L’analyse principale portait sur 25 établissements de soins de courte durée mesurant les cpKPI de façon continue. Les processus de soins les plus fréquemment réalisés mesurés avec les cpKPI étaient l’élaboration d’un plan de soins pharmaceutiques (chez 59 % des patients), la résolution de problèmes liés à la pharmacothérapie (37 % des patients) et la participation aux tournées de soins interprofessionnelles (36 % des patients). Les soins mesurés les moins fréquemment réalisés étaient l’éducation des patients sur les médicaments durant l’hospitalisation (7 % des patients), la conciliation des médicaments au moment du congé (15 % des patients) et l’éducation des patients sur les médicaments au moment du congé (17 % des patients).
Conclusions
Le premier registre national destiné à la collecte d’indicateurs de qualité des soins en pharmacie clinique a été établi et utilisé pour caractériser la prestation réelle de soins liés aux cpKPI. Les résultats tirés de ce registre pourraient faciliter l’évaluation comparative des cpKPI à l’échelle des hôpitaux et soutenir le partage national des meilleures pratiques afin de faire progresser la pratique de la pharmacie et d’améliorer les résultats pour les patients.
Mots-clés: indicateurs de qualité des soins, indicateurs clés de performance, pharmacie clinique, registre de patients, soins pharmaceutiques, conciliation des médicaments
INTRODUCTION
Health care key performance indicators are quantifiable measures of quality used to track a health care organization’s progress and critical success factors.1,2 There is a compelling body of pharmacy practice literature demonstrating that specific clinical pharmacist–led activities, performed within a bundle of interrelated processes of care, have an impact on meaningful patient outcomes, such as hospital readmissions.3–8 On the basis of this evidence, the Canadian National cpKPI Collaborative used a Delphi consensus process to establish a set of 8 evidence-informed, national clinical pharmacy key performance indicators (cpKPIs).2 The 5 characteristics of a cpKPI are that it reflects a desired quality practice, links to direct patient care, links to evidence of impact on meaningful patient outcomes, is feasible to measure, and is a pharmacy- or pharmacist-sensitive metric.2,9 The established set of 8 cpKPIs consists of medication reconciliation on admission; pharmaceutical care, including development of care plans and resolution of drug therapy problems (DTPs); active participation on interprofessional patient care rounds; provision of patient medication education during the hospital stay and at discharge; medication reconciliation at discharge; and provision of a bundle of proactive patient care activities.2,9 Each cpKPI is comprehensively defined in the cpKPI knowledge mobilization guide9 (see also Appendix 1).
With the establishment of the 8 cpKPIs, there now exists a standardized suite of clinical pharmacy processes of care that can be used to measure the quality of clinical hospital pharmacy practice. Some health care organizations across Canada are measuring data at the local level and submitting selected cpKPI data to local hospital score cards, hospital accreditation bodies, provincial health quality organizations, and national hospital pharmacy organizations. However, variations exist regarding which cpKPI care services are delivered, which cpKPIs are explicitly measured, the frequency of their measurement, and the associated cpKPI practice profiles.
A patient registry refers to a structured repository that systematically collects information about a specific population with a common characteristic, which can then be used to inform clinical practice, research, and quality improvement.10 Key characteristics of patient registries include centralization of the repository, focus on observational data, uniformity of the data collection process, and collection of data over time.10 In this article, we describe the creation of a national cpKPI patient registry intended to serve as a centralized repository to collect, store, and organize data on cpKPIs from multiple Canadian health care organizations over time. The term “patient-level” applies to specific cpKPI elements of care that individual patients receive. This cpKPI national health quality indicator registry, overseen by the Canadian National cpKPI Collaborative, may eventually facilitate national patient-proportion benchmarking and trend analysis across the country, allow tracking of national implementation progress, and enable meaningful comparisons of clinical pharmacy services within and among organizations.
Furthermore, a cpKPI patient registry may allow identification of key patient care gaps and achievements and may support the ability of the pharmacy profession to advocate to governments and organizations about the impact that pharmacists have on patient care. At the time this study was undertaken, a national registry to capture national cpKPI patient data and track national progress did not exist. The aim of this study was to develop a national cpKPI patient registry, to characterize delivery of cpKPI-related care, and to generate pooled national summary cpKPI reports to inform the advancement of pharmacy practice and improve patient outcomes.
METHODS
Study Design and Objectives
This national, retrospective, observational quality improvement study enrolled health care organizations across Canada that had implemented, at the local level, tracking of health quality indicators (i.e., cpKPIs) for patient care processes delivered by pharmacists.
The primary objectives were to design and develop a national cpKPI registry and to generate pooled national summary cpKPI reports that could be used to inform the advancement of pharmacy practice and improve the quality of patient care.
The primary end points were the proportions of patients who received each of the cpKPI processes of care (as defined in Appendix 1). The secondary end points were the absolute number of patients receiving each individual cpKPI and the total number of health care organizations measuring each cpKPI. The data were reported as pooled, de-identified, national patient-level and hospital-level data.
Study Participants and Inclusion Criteria
Health care organizations that were part of the Canadian National cpKPI Collaborative were invited during a national conference call and by email to participate in the cpKPI registry. Those that were measuring at least one cpKPI in at least one inpatient clinical patient care area between January and December 2018 were enrolled. Ethics approval for this study was provided by the University Health Network Research Ethics Board (REB), which served as the central study REB. Individual site-specific data transfer agreements were obtained.
Data Collection
This study was based on anonymized (de-identified), aggregate hospital-level cpKPI data submitted by local hospital teams to the national central measurement team. For this purpose, a standardized Microsoft Excel data collection form (spreadsheet) was used by all hospital sites. This data collection tool and a “How-To Guide” for data entry and submission were distributed by email to each local pharmacy site lead. Each health care organization submitted information about hospital and health care organization characteristics, including number of hospital beds, number of full-time equivalent pharmacists, type of institution (acute care, rehabilitation, or long-term care), involvement of pharmacy learners in cpKPI measurement, and teaching hospital status. In addition, each local pharmacy site lead reported the types of cpKPI that each hospital was measuring for all hospital visits and submitted data for each cpKPI during each fiscal quarter (reported as the number of patients who received the cpKPI event divided by the total number of patients either admitted or discharged, as applicable for the specific cpKPI) and whether the data were captured on an intermittent (less than 2-week period) or continuous basis. This numerator/denominator information represented high-level aggregate administrative data submitted without hospital, individual patient, or pharmacy clinician identifiers. To guide local cpKPI tracking, individual hospitals used the cpKPI knowledge mobilization guide9 (published online in affiliation with the Canadian Society of Hospital Pharmacists, now known as the Canadian Society of Healthcare-Systems Pharmacy), which includes detailed cpKPI definitions, with specifications for numerators and denominators. Of note, the hospitals conducted their own cpKPI tracking using local systems and approaches. Many of the participating hospitals had built cpKPI tracking tools into their local hospital information systems, while other hospitals had mobile cpKPI trackers.
Once the de-identified, aggregate data had been entered, the pharmacy site leads sent each hospital file to the study investigators electronically, using a secure, password-protected, REB-approved file-sharing portal. Data collected at the patient level were pooled to the local hospital level, and then further pooled to generate a national-level patient proportion for each cpKPI process of care (all relevant hospitals combined). The central measurement team screened all data submissions for anomalies and followed up as needed with local pharmacy leads for clarification before national-level pooling. All incoming data were uploaded to the national cpKPI patient registry, housed within a Microsoft Excel spreadsheet. Storage of the submitted data followed all REB requirements for privacy, data security, and electronic storage of research data on hospital-based secure servers.
Data Analysis
Organizational characteristics and cpKPI data were summarized using descriptive statistics, such as proportions. Results were displayed graphically. Confidential local data were shared with individual pharmacy site leads. The de-identified, pooled national summary results, along with confidential local benchmarking reports and a unique code, were also shared with the individual health care organizations. The unique code provided to each health care organization permitted sites to see their own health organization’s data compared to both national pooled proportions and de- identified data from other hospitals.
RESULTS
The cpKPI Registry: National Pooled Results
In 2018, the baseline year of data collection, data for a total of 275 896 patient visits were collected from 32 health care organizations located in 5 provinces across Canada. Of the 32 health care organizations, 27 (84%) were acute care hospitals, 2 (6%) were long-term care institutions, 2 (6%) were rehabilitation centres, and 1 (3%) was classified as “other” (mental health institution). This pooled national sample represented health care organizations with totals of 433.6 full-time equivalent pharmacists and 8079 beds, with 6106 (76%) of these beds covered by a clinical pharmacist and therefore eligible to receive at least one cpKPI during the period January to December 2018. Eleven (34%) of the 32 health care organizations reported that pharmacy students and pharmacy residents were involved in performing cpKPI-related activities. Overall, 20 (63%) of the 32 health care organizations were considered academic teaching centres.
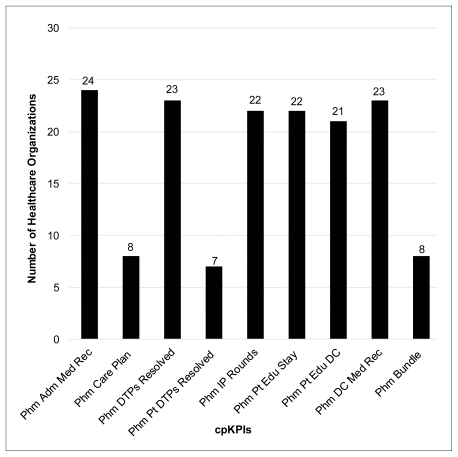
The participating health care organizations varied with respect to which cpKPIs were locally tracked and measured (Figure 1). From January to December 2018, all 8 cpKPIs were being measured by at least some organizations, with the most commonly measured indicator being admission medication reconciliation by a pharmacist (n = 24 [75%] of the 32 health care organizations), followed by resolution of DTPs expressed as an absolute number (n = 23 [72%]), discharge medication reconciliation by a pharmacist (n = 23 [72%]), participation in interprofessional patient care rounds (n = 22 [69%]), and patient education during the hospital stay (n = 22 [69%]). Notably, only 2 hospitals tracked cpKPIs on an intermittent (pulse) basis.
|
| |
|
FIGURE 1 Number of health care organizations (out of 32 that reported data) measuring each clinical pharmacy key performance indicator across Canada in 2018. The 32 health care organizations accounted for a total of 275 896 patient visits. Phm Adm Med Rec = medication reconciliation on admission performed by a pharmacist, Phm Care Plan = pharmaceutical care plan developed by a pharmacist, Phm DTPs Resolved = total number of drug therapy problems resolved by a pharmacist, Phm Pt DTPs Resolved = proportion of patients for whom a drug therapy problem was resolved by a pharmacist, Phm IP rounds = proportion of patients for whom a pharmacist participated in interprofessional patient care rounds, Phm Pt Edu Stay = provision of education during hospital stay by a pharmacist, Phm Pt Edu DC = provision of education at hospital discharge by a pharmacist, Phm DC Med Rec = medication reconciliation at discharge performed by a pharmacist, Phm Bundle = comprehensive direct patient care bundle performed by a pharmacist. |
The cpKPI Registry: Core Analysis
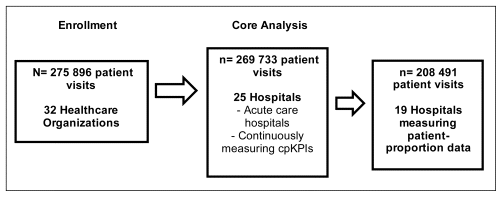
The core analysis was limited to acute care health care organizations that were continuously tracking cpKPIs. Of the 32 health care organizations in the study, 25 met these a priori criteria for inclusion in the core analysis. Among hospitals in this sample, the average number of beds was 239 and the average number of full-time equivalent pharmacists was 14. Eight (32%) and 10 (40%) of the 25 hospitals reported that pharmacy students and pharmacy residents, respectively, were involved in performing cpKPI-related activities. Overall, 15 (60%) of the 25 hospitals were considered academic teaching centres, and 19 hospitals (76%), with a total of 208 491 patient visits, measured cpKPIs as patient proportions (Figure 2).
|
| |
|
FIGURE 2 Initial enrolment and inclusion of health care organizations in the core analysis. Of the 32 organizations initially enrolled, 27 were acute care hospitals, 2 were long-term care homes, 2 were rehabilitation centres, and 1 was classified as “other”. Of note, 2 of the 32 organizations measured clinical pharmacy key performance indicators on an intermittent basis. |
For the cpKPI referring to resolution of DTPs by a pharmacist, 17 (68%) of the 25 core analysis hospitals, with a total of 192 210 patient visits, collected the data as the absolute number of DTPs resolved, not as the proportion of patients receiving this care activity. Of the remaining 8 core analysis hospitals, 5 reported data for this cpKPI as the patient proportion and 3 did not report data for either cpKPI (patient proportion and absolute number of resolved DTPs).
Patient-Proportion cpKPIs
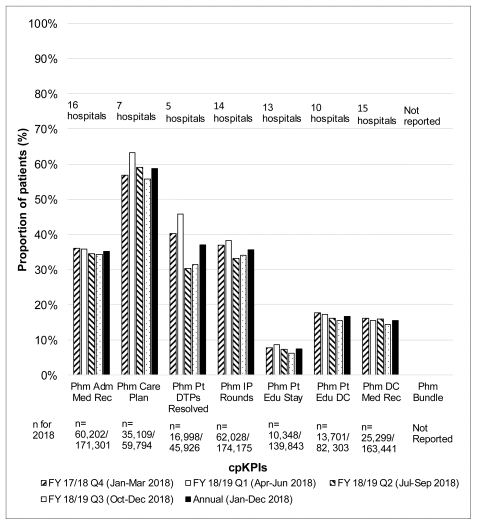
The most commonly delivered cpKPI-related care services were development of a pharmaceutical care plan (59% of patients), followed by resolution of DTPs (37% of patients), participation in interprofessional patient care rounds (36% of patients), and medication reconciliation on admission (35% of patients) (Figure 3). No hospitals submitted patient-level data for the proportion of patients receiving the direct patient care bundle. Pharmacist activities such as patient medication education during the hospital stay (7% of patients) and at discharge (17% of patients), as well as medication reconciliation on discharge (15% of patients), were performed for relatively fewer patients and may represent national care gaps.
|
| |
|
FIGURE 3 Core analysis: pooled proportion of patients receiving each clinical pharmacy key performance indicator (cpKPI) activity in Canada in 2018. Data are derived from a total of 19 individual acute care hospitals (representing 208 491 patient visits) that continuously measured cpKPIs on a patient-proportion basis in 2018. For each cpKPI, the number of hospitals contributing data is indicated at the top of the graph, and the number of patients who received the cpKPI event divided by the total number of patients either admitted or discharged is shown at the bottom. Data are presented for each quarter of the calendar year (January to December 2018), with the fiscal year (FY) designation also shown. Phm Adm Med Rec = medication reconciliation on admission performed by a pharmacist, Phm Care Plan = pharmaceutical care plan developed by a pharmacist, Phm Pt DTPs Resolved = proportion of patients for whom a drug therapy problem was resolved by a pharmacist, Phm IP rounds = proportion of patients for whom a pharmacist participated in interprofessional patient care rounds, Phm Pt Edu Stay = provision of education during the hospital stay by a pharmacist, Phm Pt Edu DC = provision of education at hospital discharge by a pharmacist, Phm DC Med Rec = medication reconciliation at discharge performed by a pharmacist, Phm Bundle = comprehensive direct patient care bundle performed by a pharmacist. |
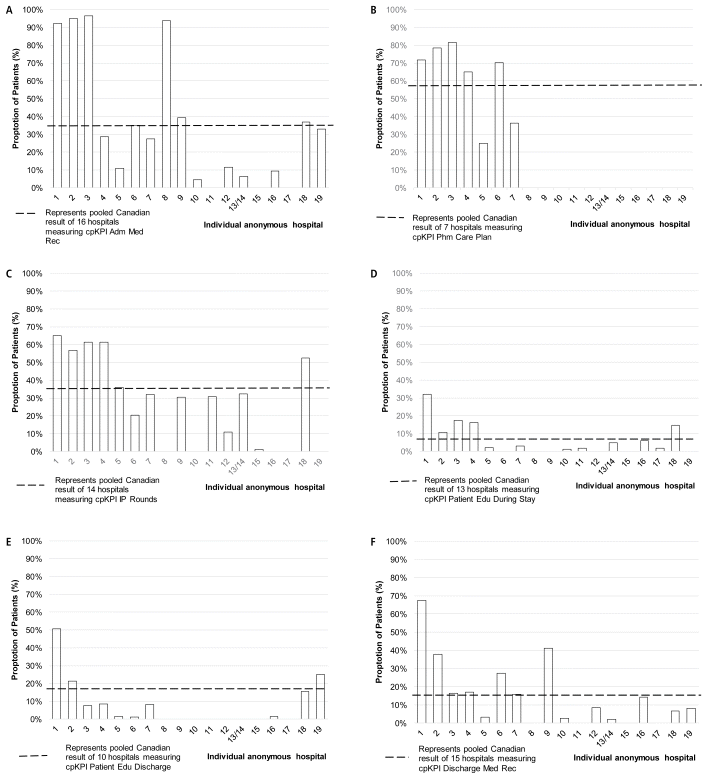
The patient-proportion data for each acute care hospital are presented in a comparative bar graph for each cpKPI that was measured and reported by more than 5 hospitals (Figure 4). There was wide variability in the delivery of cpKPI-related care among the participating hospitals.
|
| |
|
FIGURE 4 Core analysis: proportion of patients at individual acute care hospitals who received various clinical pharmacy key performance indicator (cpKPI) processes. Data were derived from the 19 acute care hospitals (representing 208 491 patient visits) that continuously measured cpKPIs on a patient-proportion basis in 2018. (A) Medication reconciliation by a pharmacist upon admission, based on 16 hospitals that measured this cpKPI, with pooled proportion of 35%. (B) Preparation of a pharmaceutical care plan by a pharmacist, based on 7 hospitals that measured this cpKPI, with pooled proportion of 59%. (C) Pharmacist participation in interprofessional patient care rounds, based on 14 hospitals that measured this cpKPI, with pooled proportion of 36%. (D) Patient education from a pharmacist during the hospital stay, based on 13 hospitals that measured this cpKPI, with pooled proportion of 7%. (E) Patient education from a pharmacist at discharge, based on 10 hospitals that measured this cpKPI, with pooled proportion of 17%. (F) Medication reconciliation from a pharmacist at discharge, based on 15 hospitals that measured this cpKPI, with pooled proportion of 15%. Data for hospitals 13 and 14 were pooled, as submitted by the health care organization, and are therefore represented as one combined bar. |
Resolution of DTPs
The total number of DTPs resolved, as reported by 17 health care organizations, was 147 000 for the baseline year of 2018. Future cpKPI registry studies may plan for more detailed DTP classification or medication type breakdown for this cpKPI, which may better characterize the pharmaceutical care delivered.
DISCUSSION
To our knowledge, this is the first national registry study reporting on clinical pharmacy health quality indicators that characterize real-world delivery of cpKPI-related care by hospital pharmacists. Since the establishment of consensus cpKPIs in 2013,2 there have been substantial efforts by health care organizations across the country to begin measuring multiple cpKPIs, as seen in Figure 1. Among the 32 health care organizations that participated in the current study, there has been significant implementation of cpKPI measurement, with 76% of the pooled 8079 beds represented being eligible to receive at least one cpKPI process of care from a pharmacist during 2018. However, there was variability among the cpKPI practice profiles across the country.
Measuring and reporting cpKPIs at the national level may facilitate identification of national strengths in care delivery, as well as gaps in care that represent opportunities for improvement. Furthermore, a national cpKPI registry could promote awareness of current national patient-level rates, facilitate external benchmarking, and permit analysis of national trends over time. It may also serve to motivate additional hospitals to track and expand cpKPI-related care delivery, which is based on interventions that have been shown, in randomized controlled trials (RCTs), to improve patient outcomes.5,6 In the core analysis for the 19 acute care hospitals that reported data in terms of patient proportions, the most common cpKPI care service, received by the highest proportion of patients, was pharmaceutical care planning (59% of patients), followed by resolution of DTPs (37% of patients), participation in interprofessional patient care rounds (36% of patients), and medication reconciliation on admission (35% of patients). These findings indicate that providing pharmaceutical care by developing a care plan and resolving DTPs, performing medication reconciliation on admission, and participating in interprofessional patient care rounds are 3 valuable clinical pharmacy processes of care that are most often delivered across Canada. No data were submitted by any participating organizations on the proportion of patients receiving the direct patient care bundle. The lack of data for this cpKPI during this inaugural round of the registry may be due to the high pragmatic complexity of capturing multiple cpKPIs for individual patients. Although it is a complex measure, this cpKPI is of importance given that the evidence demonstrating a positive impact on health care utilization has involved pharmacist-led interventions performed within a bundle of interrelated processes of care, rather than cpKPI-related care services delivered in isolation.11 We are hopeful that this measure will be reported in future rounds of data collection. Pharmacist activities such as patient medication education during the hospital stay and at discharge, as well as medication reconciliation at discharge, were performed for relatively fewer patients. These cpKPIs may represent clear care gap opportunities for most hospitals and may provide direction in refocusing future pharmacist-led efforts.
In addition, the comparison of acute care hospitals (Figure 4) may permit hospital profile benchmarking and support national sharing of best practices. The registry system allowed each health care organization to directly compare its confidential local results to de-identified findings from other hospitals across the country and to the national pooled results. This capability may encourage certain institutions to learn from the operations of a leading organization.12 However, in interpreting these results, it is important to consider the various hospital-level factors that may contribute to the observed variability, such as pharmacy practice model, bed size, amount of support/resources, and the electronic documentation tools and health information systems available to capture clinical workload and cpKPIs. Therefore, direct comparisons between institutions can be challenging. Of the cpKPIs included in the core analysis of acute care hospitals, pharmacist-led admission medication reconciliation showed the most variability (Figure 4A). Interprofessional admission medication reconciliation is a hospital accreditation standard in Canada, so it was notable that the pooled national result for pharmacist-led admission medication reconciliation was so low (35%). This finding may have been due to the distinction between hospitals where pharmacists perform medication reconciliation on admission and those that have other health professionals, such as nurses or physicians, leading this activity. Alternatively, a resource-intensive intervention such as pharmacist-led admission medication reconciliation may be targeted for high-risk patients, who may derive the most benefit.11 It is also possible that some institutions were in the early phase of implementing cpKPI tracking, such that admission medication reconciliation was under-reported. A total of 147 000 DTPs were resolved among the 17 acute care hospitals measuring resolution of DTPs as the total number (not patient proportion). This result may be more meaningful if it could be expressed in relation to the corresponding number of patients in the sample with analysis of any trends over several years.
This appears to be the first national registry capturing real-world cpKPI patient data in Canada and worldwide. Cillis and others13 conducted a trial in Belgium involving development of a benchmarking tool that included clinical pharmacy activities and non–direct patient care activities. The next phase of their study was to include implementing the tool on a national scale to identify the most efficient practices.13 Similarly, in New Zealand, Ng and Harrison14 developed a set of key performance indicators for clinical pharmacy services but recognized the importance and challenges of measuring these data nationwide. Although we believe that ours is the first national registry to capture cpKPIs, there is already a fully operational National Database of Nursing Quality Indicators.15 Data from this registry have facilitated advocating for more nursing staff, have allowed demonstration of the impact of staffing on important patient outcomes such as incidence of falls, and have facilitated the sharing of best practices among various nursing units.15 Tracking key performance indicators for the nursing profession has been valuable, and we believe that continuous measurement of key performance indicators for pharmacy is just as promising.
Our study had several strengths. It was a large, national study conducted in various practice settings (i.e., acute care, long-term care, rehabilitation) and involving a large number of patient visits and health care organizations. In addition, this work led to the first national patient registry in Canada to capture real-world cpKPI patient-proportion data.
Our study also had several limitations. There may have been some minor nuanced variability in how different sites defined the denominator for proportion-level cpKPI data. To minimize such variability, standard definitions from the published cpKPI knowledge mobilization guide9 were included in the submission tool to guide local sites, and to promote consistency and alignment of data reporting. Of note, the cpKPI definitions in the guide were developed using relevant published acute care RCTs to guide decision-making.5,6 We included only those acute care sites that were continuously measuring cpKPIs in the core analysis to align with these acute care RCTs. Another limitation was the self-reporting of cpKPI data by pharmacists (without independent verification). Given that this study was based on submission of local hospital cpKPI data to a national central measurement team, independent auditing of the local hospitals’ cpKPI tracking or individual pharmacists’ cpKPI reporting was beyond the scope of the investigation. As such, as is the case with many health quality indicators, local under-reporting was possible. Conversely, many hospitals were documenting cpKPIs directly into the hospital information system or electronic patient chart, an approach that promotes transparency and data integrity.
Overall, our findings demonstrate that health care organizations across Canada had variable cpKPI practice profiles. Future directions include establishing a more precise breakdown of patient-proportion results by clinical area (e.g., critical care, surgery, medicine) to permit more relevant and specific benchmarking. In addition, enhanced use of technology to track cpKPIs locally and to generate a database for national submissions could be explored. Furthermore, future studies could include multiple years of data to assess year-to-year longitudinal trends in cpKPI-related care and to investigate real-world impact on patient outcomes (such as readmissions) at the national level.
CONCLUSION
The first national registry for capturing clinical pharmacy health quality indicators in Canada (in the form of real-world, patient-level cpKPI data) was established. The findings from this registry could facilitate identification of strengths, care gaps, and opportunities for the provision of cpKPI-related processes of care across the country, and could also support national sharing of best practices to advance pharmacy practice and improve patient outcomes.
References
1 Doucette D. Should key performance indicators for clinical services be mandatory? The “pro” side. Can J Hosp Pharm. 2011;64(1):55–6.
2 Fernandes O, Gorman SK, Slavik RS, Semchuk WM, Shalansky S, Bussières JF, et al. Development of clinical pharmacy key performance indicators for hospital pharmacists using a modified Delphi approach. Ann Pharmacother. 2015;49(6):656–69.
Crossref PubMed
3 Kaboli PJ, Hoth AR, McClimon BJ, Schnipper JL. Clinical pharmacists and inpatient medical care: a systematic review. Arch Intern Med. 2006;166(9):955–64.
Crossref PubMed
4 Bond CA, Raehl CL. Clinical pharmacy services, pharmacy staffing, and hospital mortality rates. Pharmacotherapy. 2007;27(4):481–93.
Crossref PubMed
5 Makowsky MJ, Koshman SL, Midodzi WK, Tsuyuki RT. Capturing outcomes of clinical activities performed by a rounding pharmacist practicing in a team environment: the COLLABORATE study. Med Care. 2009;47(6):642–50.
Crossref PubMed
6 Gillespie U, Alassaad A, Henrohn D, Garmo H, Hammarlund-Udenaes M, Toss H, et al. A comprehensive pharmacist intervention to reduce morbidity in patients 80 years or older: a randomized controlled trial. Arch Intern Med. 2009;169(9):894–900.
Crossref PubMed
7 Ravn-Nielsen LV, Duckert ML, Lund ML, Henriksen JP, Nielsen ML, Eriksen CS, et al. Effect of an in-hospital multifaceted clinical pharmacist intervention on the risk of readmission. JAMA Intern Med. 2018; 178(3):375–82.
Crossref PubMed PMC
8 Mekonnen AB, McLachlan AJ, Brien JE. Effectiveness of pharmacist-led medication reconciliation programmes on clinical outcomes at hospital transitions: a systematic review. BMJ. 2016;6(2):e010003.
9 Fernandes O, Toombs K, Pereira T, Lyder C, Bjelajac Mejia A, Shalansky S, et al. Canadian consensus on clinical pharmacy key performance indicators: knowledge mobilization guide. Canadian Society of Hospital Pharmacists; 2015.
10 Gliklich RE, Leavy MB, Dreyer NA. Patient registries. In: Gliklich RE, editor. Registries for evaluating patient outcomes: a user’s guide. 4th ed. Agency for Healthcare Research and Quality; 2020. p. 8–22.
11 Fernandes O, Baker M. Can pharmacists collaborate with patients and interprofessional teams to reduce medication-related risk at interfaces of care and improve meaningful patient outcomes? [editorial]. J Pharm Pract Res. 2017;47(5):331–2.
Crossref
12 Fernandes OA, Le Piane F, Ahmed H, Toombs K. Should key performance indicators be a component of performance assessment for individual clinical pharmacists? The “con” side. Can J Hosp Pharm. 2014; 67(2):166–8.
13 Cillis M, Spinewine A, Krug B, Quennery S, Wouters D, Dalleur O. Development of a tool for benchmarking of clinical pharmacy activities. Int J Clin Pharm. 2018;40(6):1462–73.
Crossref PubMed
14 Ng J, Harrison J. Key performance indicators for clinical pharmacy services in New Zealand public hospitals: stakeholder perspectives. J Pharm Health Serv Res. 2010;1(2):75–84.
Crossref
15 Montalvo I. The National Database of Nursing Quality Indicators® (NDNQI®). Online J Issues Nurs. 2007;12(3). doi:10.3912/OJIN.Vol12No03Man02
Crossref
Amanda Carroccia, PharmD, is with the University Health Network, Toronto, Ontario.
Olavo A Fernandes, PharmD, is with the University Health Network and the Leslie Dan Faculty of Pharmacy, University of Toronto, Toronto, Ontario.
Kent Toombs, MHS, is with Nova Scotia Health, Halifax, Nova Scotia.
Sean K Gorman, PharmD, is with the Interior Health Authority, Kelowna, British Columbia, and the Faculty of Pharmaceutical Sciences, The University of British Columbia, Vancouver, British Columbia.
Sean P Spina, PharmD, is with Island Health, Victoria, British Columbia, and the Faculty of Pharmaceutical Sciences, The University of British Columbia, Vancouver, British Columbia.
William M Semchuk, PharmD, is with the Saskatchewan Health Authority, Regina, Saskatchewan, and the College of Pharmacy and Nutrition, University of Saskatchewan, Saskatoon, Saskatchewan.
Andrea Meade, BScPhm, is with Nova Scotia Health, Halifax, Nova Scotia.
Donna Lowe, PharmD, is with the University Health Network, Toronto, Ontario.
Tania Bayoud, PharmD, is with St Joseph’s Health Care London, London, Ontario.
Stephen Shalansky, PharmD, is with Providence Health Care and the Faculty of Pharmaceutical Sciences, The University of British Columbia, Vancouver, British Columbia.
Nadia M Facca, MHS, was, at the time of this study, with the London Health Sciences Centre, London, Ontario. She is now with Alexandra Hospital Ingersoll, Ingersoll, Ontario, and the Tillsonburg District Memorial Hospital, Tillsonburg, Ontario.
Winnie Seto, PharmD, is with The Hospital for Sick Children and the Leslie Dan Faculty of Pharmacy, University of Toronto, Toronto, Ontario.
Jean-François Bussières, MSc, is with CHU Sainte-Justine and the Faculté de pharmacie, Université de Montréal, Montréal, Quebec.
Gary G Wong, BScPhm, is with the University Health Network, Toronto, Ontario.
Philip Lui, PharmD, is with the University Health Network, Toronto, Ontario.
Richard S Slavik, PharmD, is with the Interior Health Authority, Kelowna, British Columbia, and the Faculty of Pharmaceutical Sciences, The University of British Columbia, Vancouver, British Columbia.
Douglas Doucette, PharmD, is with Horizon Health Network, Moncton, New Brunswick, and the College of Pharmacy, Dalhousie University, Halifax, Nova Scotia.
Gali Latariya, PharmD, is with Nova Scotia Health, Halifax, Nova Scotia.
Clarence Chant, PharmD, is with Unity Health Toronto and the Leslie Dan Faculty of Pharmacy, University of Toronto, Toronto, Ontario.
Address correspondence to: Dr Olavo A Fernandes, Pharmacy Department, Toronto Western Hospital, University Health Network, Fell 4-213, 399 Bathurst Street, Toronto ON M5G 2S8, email: olavo.fernandes@uhn.ca
(Return to Top)
Competing interests: Andrea Meade serves on the National Professional Practice Advisory Committee of the Canadian Society of Healthcare-Systems Pharmacy (CSHP) and is the CSHP’s Nova Scotia Branch Advocacy Representative (volunteer roles). Sean Spina served (until 2024) as a Presidential officer with the CSHP and is a founding Board member of the Indigenous Pharmacy Professionals of Canada. No other competing interests were declared.
Disclaimer: Stephen Shalansky is the Editor and Clarence Chant is an Associate Editor with the Canadian Journal of Hospital Pharmacy. They were not involved in the editorial decision-making process for this article.
Funding: No funding was received for this project; however, in-kind support was provided by the University Health Network pharmacy residency program.
Acknowledgements: The authors thank Bob Maclean, Erin MacNeil, Sandra Zaikos, members of the Canadian National cpKPI Collaborative, and various students and local team members who were involved in various stages of the national cpKPI project.
Submitted: April 9, 2025
Accepted: August 4, 2025
Published: November 12, 2025
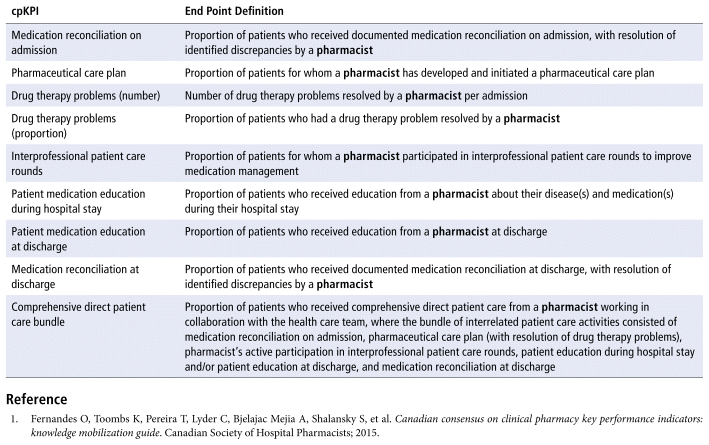
APPENDIX 1 Definitions of end points for clinical pharmacy key performance indicators (cpKPIs).1
© 2025 Canadian Society of Healthcare-Systems Pharmacy | Société canadienne de pharmacie dans les réseaux de la santé
Canadian Journal of Hospital Pharmacy, VOLUME 78, NUMBER 4, 2025




